THE JAPANESE JOURNAL OF ANTIBIOTICS ( 79)
|
|
|
- ひでより いざわ
- 5 years ago
- Views:
Transcription
1 346 ( 78) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ ,919 NTT
2 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 79)
3 348 ( 80) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4
4 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 81) ,919 Streptococcus pyogenes Streptococcus pneumoniae Moraxella catarrhalis Haemophilus influenzae (FQs) S. pyogenes Escherichia coli FQs E. coli 30% FQs Staphylococcus aureus (MRSA) FQs Sitafloxacin (STFX) 45% 95% S. aureus (MSSA) FQs 10% Staphylococci (MRCNS) FQs Staphylococci (MSCNS) MRSA MSCNS FQs MSSA Enterococcus faecalis FQs 22.5% 29.6% Enterococcus faecium FQs STFX (58.3%) 85% Pseudomonas aeruginosa FQs 21 27% 13 21% 5.6% 1.8% Acinetobacter spp. FQs 2.7% Neisseria gonorrhoeae FQs 86 88% 15 FQs Staphylococci Enterococci E. coli P. aeruginosa N. gonorrhoeae 90%
5 350 ( 82) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 (FQs) b- FQs DNA IV (LVFX) 1,2) FQs FQs 1992 LVFX FQs 3,4) FQs Escherichia coli 2000 FQs FQs b (ESBL) MRSA Streptococcus pneumoniae (PRSP) ESBL E. coli Klebsiella pneumoniae b- MBL DNA 5) FQs FQs , ,919 Table 1 Table BML 80 C 2 Levofloxacin (LVFX) Ciprofloxacin (CPFX) Tosufloxacin (TFLX) Sitafloxacin (STFX) Benzylpenicillin (PCG) Ampicillin (ABPC) Clavulanic acid Amoxicillin (CVA/AMPC) Piperacillin (PIPC) Oxacillin (MPIPC) Cefaclor (CCL) Cefotiam (CTM) Cefdinir (CFDN) Cefpodoxime (CPDX) Ceftazidime (CAZ) Cefotaxime (CTX) Ceftriaxone (CTRX) Cefpirome (CPR) Meropenem (MEPM) Panipenem (PAPM) Imipenem (IPM) Aztreonam (AZT) Minocycline (MINO) Clarithromycin (CAM) Azithromycin (AZM) Telithromycin (TEL) Vancomycin (VCM) Sulfamethoxazole Trimethoprim (ST) Gentamicin (GM) Amikacin (AMK)
6 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 83) Table 1. The number of isolates and their source.
7 352 ( 84) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 Table 2. List of the levofloxacin surveillance group. Chloramphenicol (CP) 3 (MIC) Neisseria gonorrhoeae MIC Table 3 Clinical and Laboratory Standards Institute (CLSI, 2008) 6) MIC S. pneumoniae CLSI (2007) S. pneumoniae (PSSP) PCG MIC 0.06 mg/ml PRSP PCG MIC 2
8 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 85) Table 3. Test drugs and the range of their concentrations for determination of MIC.
9 354 ( 86) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 Table 4. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. mg/ml CLSI 1 1) Table 4 Table 7 Streptococcus pyogenes CPFX (86.8%) MINO (90.4%) CAM (76.8%) AZM (74.5%) 98% STFX FQs 6 8 FQs (QRDR) (Table 4) S. pneumoniae FQs CPFX (87.0%) 98% MIC m g/ml STFX MIC mg/ml FQs VCM TEL CVA/AMPC PAPM CTRX 100% 99.7% 99.3% 99.3% 97.3% IPM 84.2%
10 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 87) Table 5. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. 18.3% 61.3% 80% (Table 4) PSSP S. pneumoniae (PISP) PRSP 52.3% 40.2% 7.5% PRSP CTRX 90% Staphylococcus aureus (MSSA) FQs MIC mg/ml FQs % STFX FQs 90% ABPC 60.3% CAM AZM CPDX 76.4% 76.4% 61.5% 80% Table 5 FQs S. aureus (MRSA) MIC 90 STFX 8.0 m g/ml >16 mg/ml >64 mg/ml FQs % FQs VCM 0.0% 35.2% VCM (Table 5) Staphylococci (MSCNS) FQs MIC mg/ ml FQs % CAM 79.9% AZM 79.5%
11 356 ( 88) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 Table 6. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. 86.6% 100% FQs STFX (Table 6) Staphylococci MRCNS MIC 90 MRSA FQs MIC >16 mg/ml % STFX MIC mg/ml MINO 97.9% VCM (Table 6) Enterococcus faecalis FQs 70.4% 77.5% 100% ABPC CVA/AMPC VCM (Table 7) Enterococcus faecium VCM (100%) MINO (48.7%) STFX (41.7%) TEL (38.4%) 15% (Table 7) 2) Table 8 Moraxella catarrhalis FQs MIC mg/ml 534 FQs ABPC 15.2% CVA/ AMPC b CTM 86.1% 95%
12 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 89) Table 7. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. N. gonorrhoeae FQs MIC mg/ml % STFX MIC mg/ml FQs MIC 90 CTRX 0.12 mg/ml AZM 1.0 mg/ml CFDN 0.5 mg/ml MINO 0.5 mg/ml CAM 2.0 mg/ml ABPC 4.0 mg/ml CVA/AMPC 4.0 mg/ml ABPC CVA/AMPC (NPPNG) NPPNG CTX 92.3% CTRX 100% CAZ 54.5% MINO 50% 44.5% 3) Table 9 Table 14 E. coli FQs MIC mg/ml STFX (91.8%) 73.6% 73.8% 30% CTM (12.8%) (Table 9) K. pneumoniae FQs MIC mg/ml FQs % IPM PAPM (Table 9) Citrobacter spp. Enterobacter spp. FQs MIC mg/ml 0.25
13 358 ( 90) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 Table 8. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. 1.0 m g/ml FQs Citrobacter spp % Enterobacter spp % IPM PAPM (Table 10) Proteus mirabilis FQs MIC mg/ml % MINO 6.4% ST CP 70.0% 74.6% FQs (Table 11) Proteus FQs MIC mg/ml % FQs PAPM (100%) IPM (99.6%) CTX (97.4%) CAZ (96.7%) 4.3% 80.7% (Table 11) Serratia marcescens FQs MIC mg/ml % IPM PAPM CAZ MIC 90 CAZ CTX CPDX mg/ml 5% (Table 12) Salmonella spp. FQs MIC mg/ml % FQs 90% (Table 12) Haemophilus influenzae FQs MIC mg/ml STFX FQs
14 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 91) Table 9. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. (LVFX MIC 8.0 mg/ml) (Table 13) b- (BLNAR) (50.1%) (92.0%) CFDN b- (BLPAR) 48 (7.1%) CVA/AMPC (CVA/AMPC MIC 8.0 mg/ml) 20 Acinetobacter spp. FQs MIC mg/ml % MINO IPM PAPM CAZ 97.5% 96.3% 94.8% 88.0% 50% (Table 13) (2.7%) Acinetobacter baumannii Pseudomonas aeruginosa FQs MIC mg/ml % FQs STFX 80% PIPC (92.0%) AMK (92.0 %) CAZ (86.6%) MEPM (86.2%) GM (85.9%) (Table 14) P. aeruginosa FQs MIC m g/ml % FQs AMK 97.3% PIPC 93.9% GM 91.2% (Table 14) CPFX, IPM, AMK (MDRP)
15 360 ( 92) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 Table 10. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. 5.6% % 12 MDRP b 66.7% 83.3% FQs MSSA MRSA MRSA FQs MRSA MRSA (Hospital-associated MRSA) Pandemic clone Multilocus Sequence Typing ST5 SCCmec type II PFGE type USA100 7) FQs 8) S. pyogenes CPFX (86.8%) FQs 98% CAM 1996; 5.6%, 1998; 6.5%, 2000; 7.5%, 2002; 9.0%, 2004; 14.8%, 2007; 23.2% AZM 2000; 7.9%, 2002; 9.2%, 2004; 13.2%, 2007; 25.5% T 9)
16 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 93) Table 11. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. prtf1 b- 10) S. pyogenes S. pneumoniae 47.7% PISP PRSP S. pneumoniae CAM AZM 80% 23S RNA S. pneumoniae ermb mefa ermb MIC ermb mefa 11)
17 362 ( 94) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 Table 12. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. S. pneumoniae 12) S. pneumoniae FQs CPFX (13.0%) % FQs DNA IV 2 13) FQs CPFX MIC LVFX FQs 14) LVFX CPFX MIC 1 mg/ml S. pneumoniae QRDR LVFX (MIC 4 mg/ml) CPFX (MIC 4 mg/ml) QRDR CPFX LVFX MIC 1 2 mg/ml QRDR LVFX 8 3 FQs
18 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 95) Table 13. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. PRSP 15) FQs FQs E. coli FQs 2007 E. coli FQs % LVFX 1994; 2.1%, 1996; 2.5%, 1998; 3.3%, 2000; 8.2%, 2002; 11.8%, 2004; 18.8% 2007; 26.2% E. coli FQ E. coli K. pneumoniae P. mirabilis CFDN % CFDN ESBL PCR E. coli 64 (8.6%) K. pneumoniae 35 (5.3%) P. mirabilis 59 (10.8%) ESBL ESBL 16) E. coli P. mirabilis E. coli ESBL
19 364 ( 96) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 Table 14. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of CLSI. FQs ESBL E. coli 47 K. pneumoniae 3 P. mirabilis 25 LVFX Salmonella Salmonella typhimurium DT104 17) FQs 18) ABPC CP MINO ST 4 Salmonella spp. 1 LVFX (MIC: 8.0 mg/ml) H. influenzae BLPAR BLNAR BLPAR BLNAR BLNAR BLPAR 7 19) BLNAR CFDN H. influenzae b- PBPs BLNAR BLNAR FQs P. aeruginosa FQs 7 FQs
20 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 97) P. aeruginosa FQs 20) 5.6% % % % 50 b- b- bla IMP-1 P. aeruginosa S. marcescens K. pneumoniae Citrobacter freundii A. baumannii 21) P. aeruginosa bla IMP-1 P. aeruginosa UTI 5.3% RTI 2.1% 16 Acinetobacter spp. 14 A. baumannii 15 FQs Staphylococci Enterococci E. coli N. gonorrhoeae P. aeruginosa 90% 1) HOOPER, D. C.: Mechanisms of action and resistance of older and newer fluoroquinolones. Clin. Infect. Dis. (2 Suppl.): S24 28, ) CROOM, K. F. & K. L. GOA: Levofloxacin: a review of its use in the treatment of bacterial infections in the United States. Drugs 63: , ) YAMAGUCHI, K.; A. OHNO & Levofloxacin Surveillance Group: Investigation of the susceptibility trends in Japan to fluoroquinolones and other antimicrobial agents in a nationwide collection of clinical isolates: a longitudinal analysis from 1994 to Diagn. Microbiol. Infect. Dis. 52: , ) ,639 Jpn. J. Antibiotics 59: , ) SUMMERS, A. O.: Genetic linkage and horizontal gene transfer, the roots of the antibiotic multi-resistance problem. Anim. Biotechnol. 17: , ) Clinical and Laboratory Standards Institute: Performans standards for antimicrobial susceptibility testing; Fifteenth informational Supplement. Approved Standard M100-S18. CLSI 28: ) BOUCHER, H. W. & G. R. COREY: Epidemiology of methicillin-resistant Staphylococcus aureus. Clin. Infect. Dis. 46 (Suppl. 5): S344 S349, ) MARANGON, F. B.; D. MILLER, M. S. MUALLEM, et al.: Ciprofloxacin and levofloxacin resistance among methicillin-sensitive Staphylococcus aureus isolates from keratitis and conjunctivitis. Am. J. Ophthalmol. 137: , ) FACINELLI, B.; C. SPINACI, G. MAGI, et al.: As-
21 366 ( 98) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 sociation between erythromycin resistance and ability to enter human respiratory cells in group A streptococci. Lancet 358: 30 33, ) SELA, S. & A. BARZILAI: Why do we fail with penicillin in the treatment of group A Streptococcus infections? Ann. Med. 31: , ) FARRELL, D. J.; S. G. JENKINS, S. D. BROWN, et al.: Emergence and spread of Streptococcus pneumoniae with erm (B) and mef (A) resistance. Emerg. Infect. Dis. 11: , ) NIEDERMAN, M. S.; J. B. Jr. BASS, G. D. CAMP- BELL, et al.: Guidelines for the initial management of adults with community-acquired pneumonia: diagnosis, assessment of severity, and initial antimicrobial therapy. American Thoracic Society. Medical Section of the American Lung Association. Am. Rev. Respir. Dis. 148: , ) WEIGEL, L. M.; G. J. ANDERSON, R. R. FACK- LAM, et al.: Genetic analyses of mutations contributing to fluoroquinolone resistance in clinical isolates of Streptococcus pneumoniae. Antimicrob. Agents Chemother. 45: , ) PIDDOCK, L. J.; M. JOHNSON, V. RICCI, et al.: Activities of new fluoroquinolones against fluoroquinolone-resistant pathogens of the lower respiratory tract. Antimicrob. Agents Chemother. 42: , ) FORWARD, K. R.: The epidemiology of penicillin resistance in Streptococcus pneumoniae. Semin. Respir. Infect. 14: , ) KOMATSU, M.; M. AIHARA, K. SHIMAKAWA, et al.: Evaluation of MicroScan ESBL confirmation panel for Enterobacteriaceae-producing, extended-spectrum beta-lactamases isolated in Japan. Diagn. Microbiol. Infect. Dis. 46: , ) DAVIS, M. A.; D. D. HANCOCK & T. E. BESSER: Multiresistant clones of Salmonella enterica: The importance of dissemination. J. Lab. Clin. Med. 140: , ) IZUMIYA, H.; K. MORI, T. KURAZONO, et al.: Characterization of isolates of Salmonella enterica serovar typhimurium displaying high-level fluoroquinolone resistance in Japan. J. Clin. Microbiol. 43: , ) TRISTRAM, S.; M. R. JACOBS, P. C. APPELBAUM: Antimicrobial resistance in Haemophilus influenzae. Clin. Microbial. Rev. 20: , ) TAKEYAMA, K.; Y. KUNISHIMA, M. MATSUKAWA, et al.: Multidrug-resistant Pseudomonas aeruginosa isolated from the urine of patients with urinary tract infection. J. Infect. Chemother. 8: 59 63, ) WALSH, T. R.: The emergence and implications of metallo-beta-lactamases in Gramnegative bacteria. Clin. Microbiol. Infect. 11 (6 Suppl.): 2 9, 2005
22 THE JAPANESE JOURNAL OF ANTIBIOTICS ( 99) In vitro susceptibilities to levofloxacin and various antibacterial agents of 12,919 clinical isolates obtained from 72 centers in 2007 KEIZO YAMAGUCHI, AKIRA OHNO, YOSHIKAZU ISHII and KAZUHIRO TATEDA Department of Microbiology and Infectious Diseases, Toho University School of Medicine MORIHIRO IWATA Department of Clinical Laboratory, Toho University Omori Medical Center and Levofloxacin-Surveillance Group MAKOTO KANDA Asahikawa City Hospital MINORU YASUJIMA Hirosaki University Hospital KOUJI AKIZAWA and CHIKARA SHIMIZU Hokkaido University Hospital MAKOTO MIKI Japanese Red Cross Sendai Hospital SHINICHIROU KON, KASTUSHI NAKAMURA and KEIKO MATSUDA Municipal Muroran General Hospital MASATO HAYASHI, SYUNJI OKUBO and SYUNKOU TOYOSHIMA Hiraka General Hospital MAKOTO TOMINAGA Yamagata University Hospital TAKUO NAKAGAWA Kozirakawa Shiseidou Hospital AKIHIRO SUGITA, TATSUMI ITO and JUN KATO Yuri-Kumiai General Hospital MITSUO KAKU Tohoku University Graduate School of Medicine IMAO SEKINE and JOJI SHIOTANI The Cancer Institute Hospital of JFCR HAJIME HORIUCHI and YOKO TAZAWA Kanto Medical Center, NTT EC AKIRA SUWABE and KUMIKO YAMAHATA Iwate Medical University Hospital AKIKO YONEYAMA Toranomon Hospital CHIZUKO KAWAMURA Aomori Prefectural Central Hospital HIROMI TASHIRO, HIROKO HORIUCHI and YOSEI KATAYAMA Hachinohe City Hospital KAZUNARI KUMASAKA Nihon University Itabashi Hospital (Present: Ageo Chuo sogo Hospital) KAZUHIKO KOIKE The University of Tokyo Hospital
23 368 (100) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 SHIGEMI KONDOU and SHIGEKI MISAWA Juntendo University School of Medicine NOBUYUKI TANIGUCHI Jichi Medical School MISTURU MURATA and YOSHIO KOBAYASHI Keio University School of Medicine YUKIO OZAKI and TAKASHI UCHIDA University of Yamanashi Hospital HIDEYUKI OKAMOTO Kawaguchi Municipal Medical Center KENICHIRO YAMAZAKI Saitama Red Cross Hospital MOTOI OKADA Koshigaya Municipal Hospital KOSUKE HARUKI Dokkyo Medical University Koshigaya Hospital HARUSHIGE KANNO and MASANORI AIHARA Takane Hospital SHIGEFUMI MAESAKI and GIICHI HASHIKITA Saitama Medical University Hospital EIJI MIYAJIMA Yokohama City University Medical Center MIDORI SUMITOMO Yokohama City University Hospital TAKEFUMI SAITO Ibarakihigashi National Hospital NOBUO YAMANE, CHIEKO KAWASHIMA and TAKAHISA AKIYAMA Ashikaga Red Cross Hospital TAMIO IEIRI, YOSHITAKA YAMAMOTO and YUKI OKAMOTO Dokkyo Medical University Hospital MASAMI MURAKAMI Gunma University Hospital KAZUHISA INUZUKA Anjo Kosei Hospital HIDEO GONDA and IKUO YAMAGUCHI Toyohashi Municipal Hospital YOSHINORI FUJIMOTO, JUNJI IRIYAMA and YUKO ASANO Ogaki Municipal Hospital HITOSHI GENMA Fukuroi Municipal Hospital (Present: Genma Clinic) MASATO MAEKAWA Hamamatsu University School of Medicine HITOSHI YOSHIMURA Mie Prefectural Shima Hospital KANAME NAKATANI Mie University Hospital HISASHI BABA Nagoya University Hospital SATOSHI ICHIYAMA Kyoto University Hospital SHINICHI FUJITA Kanazawa University Hospital
24 THE JAPANESE JOURNAL OF ANTIBIOTICS (101) HIDETOSHI OKABE, KUNIHIKO MORO and MASAYO SHIGETA Shiga University of Medical Science HARUYOSHI YOSHIDA, MASANOBU YAMASHITA and YUKIO HIDA University of Fukui Hospital TAKAYUKI TAKUBO and TADASHI KUSAKABE Osaka Medical College Hospital HIROYA MASAKI, HITOSHI HEIJYOU and HIDEO NAKAYA Kansai Medical University Takii Hospital KUNIMITSU KAWAHARA Osaka Prefectural Medical Center for Respiratory and Allergic Diseases MASAO KUWABARA Hirosima Prefectural Hospital TOSHIRO OKAZAKI, HIROMITSU FUJIWARA and HIROMI OTA Tottori University Hospital ASTUSHI NAGAI Shimane University Hospital JUN FUJITA and KIYOSHI NEGAYAMA Kagawa University Hospital TETSURO SUGIURA and MIKIO KAMIOKA Kochi Medical School MITSUHARU MURASE Ehime University Hospital REIKO SANO Nara Medical University Hospital SYUJI MATSUO and HISASHI KONO Tenri Hospital YOSUKE YUZUKI, NORIO IKEDA and MASAYA IDOMUKI Japanese Red Cross Society Wakayama Medical Center NOBUHISA YAMANE and ISAMU NAKASONE Faculty of Medicine, University of the Ryukyus AKIHIKO OKAYAMA University of Miyazaki Hospital YOSUKE AOKI, KOJI KUSABA and YUKARI NAKASHIMA Saga Medical School Hospital MASAYUKI SOMA and GO YAMAMOTO Nishi-kobe Medical Center SYOHIRO KINOSHITA and SEIJI KAWANO Kobe University Hospital MIKIO OKA Kawasaki Medical School NOBUCHIKA KUSANO Okayama University Hospital HIROAKI MIYANOHARA Kagoshima University Medical and Dental Hospital KAZUFUMI HIRAMATSU and TETSUNORI SAIKAWA Oita University Hospital KATSUNORI YANAGIHARA, JUNICHI MATSUDA and SHIGERU KOHNO Nagasaki University Hospital of Medicine and Dentistry
25 370 (102) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 DONGCHON KANG Kyushu University Graduate School of Medical Sciences KOICHI MASHIBA Kitakyushu Municipal Medical Center JUNKO ONO Fukuoka University Hospital We have reported in this journal in vitro susceptibilities of clinical isolates to antibiotics every year since In this paper, we report the results of an analysis of in vitro susceptibilities of 12,919 clinical isolates from 72 centers in Japan to selected antibiotics in 2007 compared with the results from previous years. The common respiratory pathogens, Streptococcus pyogenes, Streptococcus pneumoniae, Moraxella catarrhalis and Haemophilus influenzae maintained a high susceptibility to fluoroquinolones (FQs). The resistance of S. pyogenes to macrolides has been increasing every year and this was especially clear this year. Most strains of Enterobacteriaceae except for Escherichia coli showed a high susceptibility to FQs. Almost 30% of E. coli strains were resistant to FQs and the resistance increased further this year. FQs resistance of methicillin-resistant Staphylococcus aureus (MRSA) was approximately 95% with the exception of 45% for sitafloxacin (STFX). FQs resistance of methicillin-susceptible S. aureus (MSSA) was low at about 10%. FQs resistance of methicillin-resistant coagulase negative Staphylococci (MRCNS) was higher than that of methicillin-susceptible coagulase negative Staphylococci (MSCNS), but it was lower than that of MRSA. However, FQs resistance of MSCNS was higher than that of MSSA. FQs resistance of Enterococcus faecalis was 22.5% to 29.6%, while that of Enterococcus faecium was more than 85% except for STFX (58.3%). In clinical isolates of Pseudomonas aeruginosa derived from urinary tract infections, FQs resistance was 21 27%, which was higher than that of P. aeruginosa from respiratory tract infections at 13 21%, which was the same trend as in past years. Multidrug resistant strains accounted for 5.6% in the urinary tract and 1.8% in the respiratory tract. Acinetobacter spp. showed high susceptibility to FQs. The carbapenem resistant strains, which present a problem at present, accounted for 2.7%. Neisseria gonorrhoeae showed high resistance of 86 88% to FQs. The results of the present survey indicated that although methicillin-resistant Staphylococci, Enterococci, E. coli, P. aeruginosa, and N. gonorrhoeae showed resistance tendencies, and other species maintained high susceptibility rates more than 90% against FQs, which have been used clinically for over 15 years.
2 2 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb Neisseria gonorrhoeae ceftriaxone CTRX % 2010 CTRX 20 FQ staphylococci, E. faecium, N.
 Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 1 1 2013 69 11,762 2015 11 16 1994 2013 69 19 11,762 FQ 33 Streptococcus pyogenes, Streptococcus pneumoniae, Moraxella catarrhalis, Haemophilus influenzae
Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 1 1 2013 69 11,762 2015 11 16 1994 2013 69 19 11,762 FQ 33 Streptococcus pyogenes, Streptococcus pneumoniae, Moraxella catarrhalis, Haemophilus influenzae
日本化学療法学会雑誌第61巻第6号
 β Moraxella catarrhalis Escherichia coli Citrobacter Klebsiella pneumoniae Enterobacter cloacae Serratia marcescens Proteus Pseudomonas aeruginosa Acinetobacter Bacteroides fragilis β Haemophilus influenzae
β Moraxella catarrhalis Escherichia coli Citrobacter Klebsiella pneumoniae Enterobacter cloacae Serratia marcescens Proteus Pseudomonas aeruginosa Acinetobacter Bacteroides fragilis β Haemophilus influenzae
日本化学療法学会雑誌第64巻第4号
 β β Moraxella catarrhalisescherichia colicitrobacter Klebsiella pneumoniaeenterobacter cloacaeserratia marcescens Proteus Providencia Pseudomonas aeruginosaacinetobacter Bacteroides fragilis β β E. colik.
β β Moraxella catarrhalisescherichia colicitrobacter Klebsiella pneumoniaeenterobacter cloacaeserratia marcescens Proteus Providencia Pseudomonas aeruginosaacinetobacter Bacteroides fragilis β β E. colik.
THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 June 2012 NTT
 June 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 181 27 201072 12,866 JA 182 28 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 June 2012 NTT June 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 183 29 2012 3
June 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 181 27 201072 12,866 JA 182 28 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 June 2012 NTT June 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 183 29 2012 3
Staphylococcus epidermidis Streptococcus pneumoniae Staphylococcus epidermidis Streptococcus pneumontae S. epidermidis Table 1. Summary of the organis
 Staphylococcus aureus S. aureus (MRSA) vancomycin (VCM), arbekacin (ABK) Streptococcus pneumoniae cefuzonam (CZON), cefpirome (CPR) S. pneumoniae Enterococcus faecalis ampicillin (ABPC), imipenem (IPM)
Staphylococcus aureus S. aureus (MRSA) vancomycin (VCM), arbekacin (ABK) Streptococcus pneumoniae cefuzonam (CZON), cefpirome (CPR) S. pneumoniae Enterococcus faecalis ampicillin (ABPC), imipenem (IPM)
CHEMOTHERAPY aureus 0.10, Enterococcus faecalis 3.13, Escherichia coli 0.20, Klebsiella pneumoniae, Enterobacter spp., Serratia marcescens 0.78, Prote
 aureus 0.10, Enterococcus faecalis 3.13, Escherichia coli 0.20, Klebsiella pneumoniae, Enterobacter spp., Serratia marcescens 0.78, Proteus mirabilis 3.13, Proteus vulgaris 1.56, Citrobacter freundii 0.39,
aureus 0.10, Enterococcus faecalis 3.13, Escherichia coli 0.20, Klebsiella pneumoniae, Enterobacter spp., Serratia marcescens 0.78, Proteus mirabilis 3.13, Proteus vulgaris 1.56, Citrobacter freundii 0.39,
Streptococcus pneumoniae,streptococcus pyogenes,streptococcus agalactiae,neisseria gonorrhoeae,h.influenzae,moraxella subgenus Branhamella catarrharis
 Streptococcus pneumoniae,streptococcus pyogenes,streptococcus agalactiae,neisseria gonorrhoeae,h.influenzae,moraxella subgenus Branhamella catarrharis, E.coil,Klebsiella pneumoniae,klebsiella oxytoca,proteus
Streptococcus pneumoniae,streptococcus pyogenes,streptococcus agalactiae,neisseria gonorrhoeae,h.influenzae,moraxella subgenus Branhamella catarrharis, E.coil,Klebsiella pneumoniae,klebsiella oxytoca,proteus
03-b-„FŒ{›xŒ¾-4.02
 518( 30 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 Dec. 25 2003 1. * * Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 519( 31 ) 9 5 2003 8 2004 7 14 565 701 258 (36.8%) 443 (63.2%) Staphylococcus aureus
518( 30 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 Dec. 25 2003 1. * * Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 519( 31 ) 9 5 2003 8 2004 7 14 565 701 258 (36.8%) 443 (63.2%) Staphylococcus aureus
VOL.48 NO.7 lase negative staphylococci, Escherichia coli, Klebsiella spp., Citrobacter freundii, Enterobacter spp., indole-positive Proteus, Serratia
 ceftazidime, cefpirome, cefepime, cefoperazone/sulbactam (2: 1), imipenem Staphylococcus aureus oxacillin coagulase negative staphylococci Escherichia coli piperacillin Klebsiellac spp. Citrobacter Pseudomonas
ceftazidime, cefpirome, cefepime, cefoperazone/sulbactam (2: 1), imipenem Staphylococcus aureus oxacillin coagulase negative staphylococci Escherichia coli piperacillin Klebsiellac spp. Citrobacter Pseudomonas
THE JAPANESE JOURNAL OF ANTIBIOTICS 68 3 June 2015 Streptococcus pneumoniae, Haemophilus influenzae, Moraxella catarrhalis % 2 S. pneumon
 June 2015 THE JAPANESE JOURNAL OF ANTIBIOTICS 68 3 189 49 1 : 14 1 2 2 3 1 2 3 2015 4 3 1 : 14 CVA/AMPC 1 : 14 27 CVA/AMPC 1 : 14 88.5% Streptococcus pneumoniae, Haemophilus influenzae, Moraxella catarrhalis
June 2015 THE JAPANESE JOURNAL OF ANTIBIOTICS 68 3 189 49 1 : 14 1 2 2 3 1 2 3 2015 4 3 1 : 14 CVA/AMPC 1 : 14 27 CVA/AMPC 1 : 14 88.5% Streptococcus pneumoniae, Haemophilus influenzae, Moraxella catarrhalis
Table 1. Antimicrobial drugs using for MIC
 Table 1. Antimicrobial drugs using for MIC Table 2. Susceptibilities determined with the VITEK 2 system and agar dilution reference by interpretive eategory for Staphylococcus aureus Table 3. Interpretive
Table 1. Antimicrobial drugs using for MIC Table 2. Susceptibilities determined with the VITEK 2 system and agar dilution reference by interpretive eategory for Staphylococcus aureus Table 3. Interpretive
CHEMOTHERAPY
 CHEMOTHERAPY VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin CHEMOTHERAPY AUG. 1993 VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin Table 1. Comparative in vitro activity of teicoplanin
CHEMOTHERAPY VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin CHEMOTHERAPY AUG. 1993 VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin Table 1. Comparative in vitro activity of teicoplanin
Oct THE JAPANESE JOURNAL OF ANTIBIOTICS Pseudomonas aeruginosa 186 P. aeruginosa piperacillin PIPC, taz
 Oct. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 5 327 27 2013 2014 2016 7 5 2013 2014 Pseudomonas aeruginosa 186 P. aeruginosa piperacillin PIPC, tazobactam/piperacillin TAZ/PIPC, ceftazidime CAZ, cefepime
Oct. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 5 327 27 2013 2014 2016 7 5 2013 2014 Pseudomonas aeruginosa 186 P. aeruginosa piperacillin PIPC, tazobactam/piperacillin TAZ/PIPC, ceftazidime CAZ, cefepime
 172( 38 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 2 Apr. 2002 1 19 6 2002 5 8 4 254 254 (PBP) 90 83 65 142 PBP pbp1a, pbp2x, pbp2b 121 (49%), pbp1a, pbp2x 30 (12%), pbp2x, pbp2b 16 (6%), pbp2x 61 (24%),
172( 38 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 2 Apr. 2002 1 19 6 2002 5 8 4 254 254 (PBP) 90 83 65 142 PBP pbp1a, pbp2x, pbp2b 121 (49%), pbp1a, pbp2x 30 (12%), pbp2x, pbp2b 16 (6%), pbp2x 61 (24%),
THE JAPANESE JOURNAL OF ANTIBIOTICS 63 13 243 ( 37 ) 2007 12 2008 5 19 863 methicillin-susceptible Staphylococcus aureus (MSSA) Escherichia coli levof
 242 ( 36 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 63 _ 3 prulifloxacin * ** ** CMC * ** 2010 2 22 Prulifloxacin ulifloxacin (UFX) 3 1 2003 12 2004 5 19 534 2 2005 12 2006 5 19 805 3 THE JAPANESE JOURNAL OF
242 ( 36 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 63 _ 3 prulifloxacin * ** ** CMC * ** 2010 2 22 Prulifloxacin ulifloxacin (UFX) 3 1 2003 12 2004 5 19 534 2 2005 12 2006 5 19 805 3 THE JAPANESE JOURNAL OF
VOL. 43 NO. 4
 VOL. 43 NO. 4 Fig. 1. Frequency of Enterococcus species from complicated UTI, 1988-1992. the number * of Enterococcus species/the number of cases with complicated UTI. Fig. 3 Epidemiologic characteristics
VOL. 43 NO. 4 Fig. 1. Frequency of Enterococcus species from complicated UTI, 1988-1992. the number * of Enterococcus species/the number of cases with complicated UTI. Fig. 3 Epidemiologic characteristics
R06_01
 Staphylococcus aureus (MSSA) PCG (N=118,334) 57,369 (48.5%) 判定不能 :3 (0.0%) 60,962 (51.5%) CEZ (N=143,723) I:42 (0.0%) 143,635 (99.9%) R:46 (0.0%) CVA/AMPC (N=19,281) R:14 (0.1%) 19,265 (99.9%) 判定不能 :2
Staphylococcus aureus (MSSA) PCG (N=118,334) 57,369 (48.5%) 判定不能 :3 (0.0%) 60,962 (51.5%) CEZ (N=143,723) I:42 (0.0%) 143,635 (99.9%) R:46 (0.0%) CVA/AMPC (N=19,281) R:14 (0.1%) 19,265 (99.9%) 判定不能 :2
PCG = Benzylpenicillin ABPC= Ampicillin AMPC= Amoxicillin MPIPC = Oxacillin MCIPC = Cloxacillin SBPC= Sulbenicillin PIPC= Piperacillin
 Key words : Clinical isolates, Antibacterial susceptibility, Scale of hospital PCG = Benzylpenicillin ABPC= Ampicillin AMPC= Amoxicillin MPIPC = Oxacillin MCIPC = Cloxacillin SBPC= Sulbenicillin PIPC=
Key words : Clinical isolates, Antibacterial susceptibility, Scale of hospital PCG = Benzylpenicillin ABPC= Ampicillin AMPC= Amoxicillin MPIPC = Oxacillin MCIPC = Cloxacillin SBPC= Sulbenicillin PIPC=
 Table 1.Resistance criteria Fig.1.The resistance rates of piperacillin,ceftazidime, cefsulodin,imipenem,aztreonam,gentamicin,tobramycin,amikacin,isepamicin,fosfomycin and ofloxacin against 2,793 strains
Table 1.Resistance criteria Fig.1.The resistance rates of piperacillin,ceftazidime, cefsulodin,imipenem,aztreonam,gentamicin,tobramycin,amikacin,isepamicin,fosfomycin and ofloxacin against 2,793 strains
02-(a)-Łi’ì™·Łv-4.11
 THE JAPANESE JOURNAL OF ANTIBIOTICS 56 2 105( 13 ) 2001 1) 2) 3) JA 2 7 1) 2) 3) 106( 14 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 56 2 Apr. 1982 7 2001 (2001.4 2002.3) 1 221 175 (79.2%) 420 186 234 Staphylococcus
THE JAPANESE JOURNAL OF ANTIBIOTICS 56 2 105( 13 ) 2001 1) 2) 3) JA 2 7 1) 2) 3) 106( 14 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 56 2 Apr. 1982 7 2001 (2001.4 2002.3) 1 221 175 (79.2%) 420 186 234 Staphylococcus
 Table 1.Quality control of MICs for reference strains Table 2.Antimicrobial activity of gatifloxacin against aerobic bacteria Table 4.Antimicrobial activity of gatifloxacin and other quinolones against
Table 1.Quality control of MICs for reference strains Table 2.Antimicrobial activity of gatifloxacin against aerobic bacteria Table 4.Antimicrobial activity of gatifloxacin and other quinolones against
04-c-„FŒ{›xŒ¾-4.01
 544( 56 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 Dec. 25 2003 2. * * Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 545( 57 ) 9 5 2003 8 2004 714 565 719 50 20 39 0 9 70 79 44.4 91.7% Escherichia coli
544( 56 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 Dec. 25 2003 2. * * Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 545( 57 ) 9 5 2003 8 2004 714 565 719 50 20 39 0 9 70 79 44.4 91.7% Escherichia coli
 70( 70 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 Feb. Meropenem 2002 * * * * * * * * * * * * * * * * * * * * * * NTT Feb. THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 71( 71 ) * * * * 2003 12 22 Meropenem
70( 70 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 Feb. Meropenem 2002 * * * * * * * * * * * * * * * * * * * * * * NTT Feb. THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 71( 71 ) * * * * 2003 12 22 Meropenem
 THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 33( 33 ) 2002 JA * 1 * 2 2003 12 15 * 1) * 2) 34( 34 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 Feb. 1982 7 2002 (2002.4 2003.3) 1 174 131 (75.3%) 334 171 163 Staphylococcus
THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 33( 33 ) 2002 JA * 1 * 2 2003 12 15 * 1) * 2) 34( 34 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 Feb. 1982 7 2002 (2002.4 2003.3) 1 174 131 (75.3%) 334 171 163 Staphylococcus
CHEMOTHERAPY Proteus mirabilis GN-79 Escherichia coli No. 35 Proteus vulgaris GN-76 Pseudomonas aeruginosa No. 11 Escherichia coli ML-1410 RGN-823 Kle
 VOL. 29 NO.8 CHEMOTHERAPY 865 CHEMOTHERAPY Proteus mirabilis GN-79 Escherichia coli No. 35 Proteus vulgaris GN-76 Pseudomonas aeruginosa No. 11 Escherichia coli ML-1410 RGN-823 Klebsiella pneumoniae GN-69
VOL. 29 NO.8 CHEMOTHERAPY 865 CHEMOTHERAPY Proteus mirabilis GN-79 Escherichia coli No. 35 Proteus vulgaris GN-76 Pseudomonas aeruginosa No. 11 Escherichia coli ML-1410 RGN-823 Klebsiella pneumoniae GN-69
 Table 1 Sensitivity distribution of clinical isolates 1. Escherichia coli Inoculum size: 106cells/ml 2. Klebsiella pneumoniae 3. Enterobacter cloacae 4. Serratia marcescens Inoculum size: 106cells/nil
Table 1 Sensitivity distribution of clinical isolates 1. Escherichia coli Inoculum size: 106cells/ml 2. Klebsiella pneumoniae 3. Enterobacter cloacae 4. Serratia marcescens Inoculum size: 106cells/nil
THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterococcus avium 5Š, Corynebacterium xerosis 10Š, Corynebacterium pseudodiphtheriticum 10Š, Corynebacterium
 THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterobacter spp., Serratia spp., Burkholderia cepacia, Flavobacterium spp., Alcaligenes spp. THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterococcus avium 5Š, Corynebacterium
THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterobacter spp., Serratia spp., Burkholderia cepacia, Flavobacterium spp., Alcaligenes spp. THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterococcus avium 5Š, Corynebacterium
Staphylococcus sp. K.pneumoniae P.mirabilis C.freundii E. cloacae Serratia sp. P. aeruginosa ml, Enterococcus avium >100ƒÊg/ml
 CHEMOTHERAPY SEPT. 1992 cefoperazone ceftazidime (CAZ), imipenem (IPM) Staphylococcus sp., Enterococcus (CPZ), faecalis, Escherichia coli, Klebsiella pneumoniae, Citrobacter freundii, Enterobacter cloacae,
CHEMOTHERAPY SEPT. 1992 cefoperazone ceftazidime (CAZ), imipenem (IPM) Staphylococcus sp., Enterococcus (CPZ), faecalis, Escherichia coli, Klebsiella pneumoniae, Citrobacter freundii, Enterobacter cloacae,
1272 CHEMOTHERAPY MAR. 1975
 1272 CHEMOTHERAPY MAR. 1975 VOL. 23 NO. 3 CHEMOTHERAPY 1273 Fig. 2 Minimal inhibitory concentration of aminoglycosides against 50 strains of Klebsiella Fig. 1 Minimal inhibitory concentration of aminoglycosides
1272 CHEMOTHERAPY MAR. 1975 VOL. 23 NO. 3 CHEMOTHERAPY 1273 Fig. 2 Minimal inhibitory concentration of aminoglycosides against 50 strains of Klebsiella Fig. 1 Minimal inhibitory concentration of aminoglycosides
Fig. 1 Chemical structure of DL-8280
 Fig. 1 Chemical structure of DL-8280 Fig. 2 Susceptibility of cl in ical isolates to DL4280 Fig. 5 Susceptibility of clinical isolates to DL-8280 Fig. 3 Susceptibility of clinical isolates to DL-8280 Fig.
Fig. 1 Chemical structure of DL-8280 Fig. 2 Susceptibility of cl in ical isolates to DL4280 Fig. 5 Susceptibility of clinical isolates to DL-8280 Fig. 3 Susceptibility of clinical isolates to DL-8280 Fig.
Feb THE JAPANESE JOURNAL OF ANTIBIOTICS Tebipenem pivoxil 1 1, Meiji Seika 2 Meiji Seika G 3 Meiji Seika Tebipen
 Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 53 53 Tebipenem pivoxil 1 1, 3 2 2 1 1 Meiji Seika 2 Meiji Seika G 3 Meiji Seika 2015 12 15 Tebipenem pivoxil 10% 2010 4 2013 3 3,547 3,540 3,540 3,331
Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 53 53 Tebipenem pivoxil 1 1, 3 2 2 1 1 Meiji Seika 2 Meiji Seika G 3 Meiji Seika 2015 12 15 Tebipenem pivoxil 10% 2010 4 2013 3 3,547 3,540 3,540 3,331
VOL.47 NO.5 Table 1. Susceptibility distribution of Ĉ- lactams against clinical isolates of MRSA MRSA: rnethicillin- resistant Staphylococcus aureus
 MAY 1999 VOL.47 NO.5 Table 1. Susceptibility distribution of ƒà- lactams against clinical isolates of MRSA MRSA: rnethicillin- resistant Staphylococcus aureus (oxacillin MIC: 4ƒÊg/ ml) FMOX: flomoxef,
MAY 1999 VOL.47 NO.5 Table 1. Susceptibility distribution of ƒà- lactams against clinical isolates of MRSA MRSA: rnethicillin- resistant Staphylococcus aureus (oxacillin MIC: 4ƒÊg/ ml) FMOX: flomoxef,
Table 1. Antibacterial activitiy of grepafloxacin and other antibiotics against clinical isolates
 Table 1. Antibacterial activitiy of grepafloxacin and other antibiotics against clinical isolates Table 2-1. Summary of patients treated with grepafloxacin for respiratory infection 1) Out: outpatient,
Table 1. Antibacterial activitiy of grepafloxacin and other antibiotics against clinical isolates Table 2-1. Summary of patients treated with grepafloxacin for respiratory infection 1) Out: outpatient,
366 12 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 Dec. 2012 1 8 DNA 2,3 16 12 20 171 2008 12 2010 11 2 3,558 4.44% 1.65% 1.17% 90% 9 Escherichia coli -
 Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 365 11 sita oxacin 1 1 1 1 1 1 2 2 3 3 1 1 1 2 3 2012 9 14 sita oxacin STFX 50 mg 10% 2008 1 2008 12 2010 11 2 STFX 1,452 91.4% 1,235/1,351 95.9% 466/486
Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 365 11 sita oxacin 1 1 1 1 1 1 2 2 3 3 1 1 1 2 3 2012 9 14 sita oxacin STFX 50 mg 10% 2008 1 2008 12 2010 11 2 STFX 1,452 91.4% 1,235/1,351 95.9% 466/486
epidermidis, Enterococcus faecalis, Enterococcus Klebsiella pneumoniae, Proteus mirabilis, indolepositive Proteus spp., Enterobacter spp., Serratia
 epidermidis, Enterococcus faecalis, Enterococcus Klebsiella pneumoniae, Proteus mirabilis, indolepositive Proteus spp., Enterobacter spp., Serratia Table 3. Overall clinical efficacy of cefozopran in
epidermidis, Enterococcus faecalis, Enterococcus Klebsiella pneumoniae, Proteus mirabilis, indolepositive Proteus spp., Enterobacter spp., Serratia Table 3. Overall clinical efficacy of cefozopran in
 Key words : R-plasmid, Urinary tract infection, E. coli Fig. 1. MIC distribution against E. coli isolated from urinary tract (366 strains) and isolation - frequencies of drug-resistant strains Table 1.
Key words : R-plasmid, Urinary tract infection, E. coli Fig. 1. MIC distribution against E. coli isolated from urinary tract (366 strains) and isolation - frequencies of drug-resistant strains Table 1.
Table 1. Antibacterial spectrum SBT ABPC ABPC CPZ : sulbactamiampicillin : ampicillin : cefoperazone
 Table 1. Antibacterial spectrum SBT ABPC ABPC CPZ : sulbactamiampicillin : ampicillin : cefoperazone (inoculum size= 106 CFU/ml) (Ĉ-lactamase producer : 2 strains) Fig. 1. Sensitivity distribution of
Table 1. Antibacterial spectrum SBT ABPC ABPC CPZ : sulbactamiampicillin : ampicillin : cefoperazone (inoculum size= 106 CFU/ml) (Ĉ-lactamase producer : 2 strains) Fig. 1. Sensitivity distribution of
Fig.2. Sensitivity distribution of clinical isolates of S. epidermidis (24 strains, 106 CFU/ml) Staphylococcus aureus Staphylococcus epider- midis Ent
 Fig.2. Sensitivity distribution of clinical isolates of S. epidermidis (24 strains, 106 CFU/ml) Staphylococcus aureus Staphylococcus epider- midis Enterococcus faecalis Klebsiella pneumoniae, Morganella
Fig.2. Sensitivity distribution of clinical isolates of S. epidermidis (24 strains, 106 CFU/ml) Staphylococcus aureus Staphylococcus epider- midis Enterococcus faecalis Klebsiella pneumoniae, Morganella
CHEMOTHERAPY FEB Table 1. Activity of cefpirome and others against clinical isolates
 VOL.39 S-1 CHEMOTHERAPY FEB. 1981 Table 1. Activity of cefpirome and others against clinical isolates VOL.39 S-1 CHEMOTHERAPY FEB. 1991 72 M, 55.5 kg 66 F, 53 kg Chronic bronchitis Bronchopneumonia Peak
VOL.39 S-1 CHEMOTHERAPY FEB. 1981 Table 1. Activity of cefpirome and others against clinical isolates VOL.39 S-1 CHEMOTHERAPY FEB. 1991 72 M, 55.5 kg 66 F, 53 kg Chronic bronchitis Bronchopneumonia Peak
pneumoniae 30, C. freundii 32, E. aerogenes 27, E. cloacae 32, P. mirabilis 31, P. vulgaris 34, M. morganii 32, S. marcescens 31, H. influenzae 27, P.
 pneumoniae 30, C. freundii 32, E. aerogenes 27, E. cloacae 32, P. mirabilis 31, P. vulgaris 34, M. morganii 32, S. marcescens 31, H. influenzae 27, P. aeruginosa 30, P. maltophilia pyogenes 32, Escherichia
pneumoniae 30, C. freundii 32, E. aerogenes 27, E. cloacae 32, P. mirabilis 31, P. vulgaris 34, M. morganii 32, S. marcescens 31, H. influenzae 27, P. aeruginosa 30, P. maltophilia pyogenes 32, Escherichia
 E Societe de Pathologie Infectieuse de Langue Francaise (, 1991) E Spanish Thoracic Society (1992) E American Thoracic Society (ATS : 1993. ü ù2001 ) E British Thoracic Society (1993, ü è2001 ) E Canadian
E Societe de Pathologie Infectieuse de Langue Francaise (, 1991) E Spanish Thoracic Society (1992) E American Thoracic Society (ATS : 1993. ü ù2001 ) E British Thoracic Society (1993, ü è2001 ) E Canadian
 Table 1 Survival rates of infected mice given antibiotic doses producing peak serum a) S. aurcus Smith Challenge dose :7 ~10 (5% mucin) CFU/mouse. LD50: 1 ~103 (5% mucin) CFU/mouse. Table 2 Survival rates
Table 1 Survival rates of infected mice given antibiotic doses producing peak serum a) S. aurcus Smith Challenge dose :7 ~10 (5% mucin) CFU/mouse. LD50: 1 ~103 (5% mucin) CFU/mouse. Table 2 Survival rates
 1.Streptococcus pneumoniae, Streptococcus pyogenes JC-1,S.aureus Smith,methicillin (DMPPC)- susceptible S. aureus subsp. aureus (MSSA) TR101, DMPPC-resistant S. aureus subsp. aureus (MRSA) TR102, Staphylococcus
1.Streptococcus pneumoniae, Streptococcus pyogenes JC-1,S.aureus Smith,methicillin (DMPPC)- susceptible S. aureus subsp. aureus (MSSA) TR101, DMPPC-resistant S. aureus subsp. aureus (MRSA) TR102, Staphylococcus
VOL.32 S-7 CHEMOTHERAPY Table 1 MIC of standard strains of CTRX Fig. 2 Cumulative curves of MIC S. aureus (26 strains )
 CHEMOTHERAPY OCT. 1984 Fig. I Chemical structure of CTRX VOL.32 S-7 CHEMOTHERAPY Table 1 MIC of standard strains of CTRX Fig. 2 Cumulative curves of MIC S. aureus (26 strains ) CHEMOTHERAPY Fig. 3 Cumulative
CHEMOTHERAPY OCT. 1984 Fig. I Chemical structure of CTRX VOL.32 S-7 CHEMOTHERAPY Table 1 MIC of standard strains of CTRX Fig. 2 Cumulative curves of MIC S. aureus (26 strains ) CHEMOTHERAPY Fig. 3 Cumulative
CHEMOTHERAPY APRIL 1992 Acinetobacter calcoaceticus Staphylococcus aureus, Escherichia coli P. aeruginosa E. eoli, Klebsiella pneumoniae Serratia marc
 APRIL 1992 Acinetobacter calcoaceticus Staphylococcus aureus, Escherichia coli P. aeruginosa E. eoli, Klebsiella pneumoniae Serratia marcescens P. aeruginosa P. aeruginosa Streptococcus pyogenes Streptococcus
APRIL 1992 Acinetobacter calcoaceticus Staphylococcus aureus, Escherichia coli P. aeruginosa E. eoli, Klebsiella pneumoniae Serratia marcescens P. aeruginosa P. aeruginosa Streptococcus pyogenes Streptococcus
 Table 1. Antibacterial activity of cefdinir, cefixime, cefteram, cefuroxime, cefaclor and amoxicillin against standard strains Inoculum size: 108 cells/ml CFDN: cefdinir, CFIX: cefixime, CFTM: cefteram,
Table 1. Antibacterial activity of cefdinir, cefixime, cefteram, cefuroxime, cefaclor and amoxicillin against standard strains Inoculum size: 108 cells/ml CFDN: cefdinir, CFIX: cefixime, CFTM: cefteram,
CHEMOTHERAPY JUN Citrobacter freundii 27, Enterobacter aerogenes 26, Enterobacter cloacae 27, Proteus rettgeri 7, Proteus inconstans 20, Proteus
 VOL. 32 S-4 CHEMOTHERAPY Fig. 1 Chemical structure of sodium cefoperazone Fig. 2 Chemical structure of sodium cefoperazone CHEMOTHERAPY JUN. 1984 Citrobacter freundii 27, Enterobacter aerogenes 26, Enterobacter
VOL. 32 S-4 CHEMOTHERAPY Fig. 1 Chemical structure of sodium cefoperazone Fig. 2 Chemical structure of sodium cefoperazone CHEMOTHERAPY JUN. 1984 Citrobacter freundii 27, Enterobacter aerogenes 26, Enterobacter
CHEMOTHERAPY JUNE 1993 Table 1. Background of patients in pharmacokinetic study
 CHEMOTHERAPY JUNE 1993 Table 1. Background of patients in pharmacokinetic study VOL. 41 S 1 Table 2. Levels (Đg/ml or Đg/g) of S-1006 in serum, bile, and tissue (gallbladder) after oral administration
CHEMOTHERAPY JUNE 1993 Table 1. Background of patients in pharmacokinetic study VOL. 41 S 1 Table 2. Levels (Đg/ml or Đg/g) of S-1006 in serum, bile, and tissue (gallbladder) after oral administration
VOL. 40 S- 1 Table 1. Susceptibility of methicillin-resistant Staphylococcus aureus to meropenem Table 2. Coagulase typing of methicillin-resistant St
 CHEMOTHERAPY VOL. 40 S- 1 Table 1. Susceptibility of methicillin-resistant Staphylococcus aureus to meropenem Table 2. Coagulase typing of methicillin-resistant Staphylococcus aureus CHEMOTHERAPY Table
CHEMOTHERAPY VOL. 40 S- 1 Table 1. Susceptibility of methicillin-resistant Staphylococcus aureus to meropenem Table 2. Coagulase typing of methicillin-resistant Staphylococcus aureus CHEMOTHERAPY Table
2 2 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 1 Feb. 2012 CLSI M100-S17benzylpenicillin PCG MIC 0.05 g/ml S. pneumoniae penicillin-susceptible S. pneumon
 Feb. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 1 1 1 2008 2009 2011 10 25 2008 6 2009 4 Streptococcus pneumoniae 377 penicillin-binding protein: PBP 2004 S. pneumoniae 160 2 2 THE JAPANESE JOURNAL OF
Feb. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 1 1 1 2008 2009 2011 10 25 2008 6 2009 4 Streptococcus pneumoniae 377 penicillin-binding protein: PBP 2004 S. pneumoniae 160 2 2 THE JAPANESE JOURNAL OF
CHEMOTHERAPY
 CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of Sulbactam/CPZ against standard strains MIC mg/ml Inoculum size 106 CFU/ml * Sulbactam/CPZ= 1: 1 ** Concentration of Sulbactam+ CPZ CHEMOTHERAPY
CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of Sulbactam/CPZ against standard strains MIC mg/ml Inoculum size 106 CFU/ml * Sulbactam/CPZ= 1: 1 ** Concentration of Sulbactam+ CPZ CHEMOTHERAPY
coccus aureus Corynebacterium sp, Haemophilus parainfluenzae Klebsiella pneumoniae Pseudornonas aeruginosa Pseudomonas sp., Xanthomonas maltophilia, F
 VOL.43 S-1 coccus aureus Corynebacterium sp, Haemophilus parainfluenzae Klebsiella pneumoniae Pseudornonas aeruginosa Pseudomonas sp., Xanthomonas maltophilia, Flavobacter- Table 1. Concentration of grepafloxacin
VOL.43 S-1 coccus aureus Corynebacterium sp, Haemophilus parainfluenzae Klebsiella pneumoniae Pseudornonas aeruginosa Pseudomonas sp., Xanthomonas maltophilia, Flavobacter- Table 1. Concentration of grepafloxacin
400 46 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 Dec. 2012 LVFX 100 mg 3 / 7 150 mg 2 / 7 2 2006 2008 9 LVFX PK PD 2009 7 100 mg 1 3 500 mg 1 1 AUC/MIC
 Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 399 45 2012 11 5 LVFX 500 mg 1 1 20 Chlamydia trachomatis C. trachomatismycoplasma genitalium M. genitalium LVFX 1 500 mg 1 1 7 22 22 C. trachomatis 17
Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 399 45 2012 11 5 LVFX 500 mg 1 1 20 Chlamydia trachomatis C. trachomatismycoplasma genitalium M. genitalium LVFX 1 500 mg 1 1 7 22 22 C. trachomatis 17
988 CHEMOTHERAPY NOV. 1971
 988 CHEMOTHERAPY NOV. 1971 VOL. 19 NO. 8 CHEMOTHERAPY 989 Effect of medium-ph and inoculum size on activity of SB-PC heart infusion agar, mcg/ml Sensitivity distribution of Staphylococci to SB-PC in surgical
988 CHEMOTHERAPY NOV. 1971 VOL. 19 NO. 8 CHEMOTHERAPY 989 Effect of medium-ph and inoculum size on activity of SB-PC heart infusion agar, mcg/ml Sensitivity distribution of Staphylococci to SB-PC in surgical
DIC vegetation 1 nonbacterial thrombogenic e
 2001 2002 Guidelines for the Prevention and Treatment of Infective Endocarditis (JCS 2003) h 1 1 2 3 4 5 6 7 8 9 2 1 2 3 1 2 3 4 1 2 5 1 2 1 G Streptococcus viridans Streptococcus bovis 2 G Streptococcus
2001 2002 Guidelines for the Prevention and Treatment of Infective Endocarditis (JCS 2003) h 1 1 2 3 4 5 6 7 8 9 2 1 2 3 1 2 3 4 1 2 5 1 2 1 G Streptococcus viridans Streptococcus bovis 2 G Streptococcus
 CHEMOTHERAPY OCT. 1994 Tazobactam Piperacillin Fig. I. Chemical structures of tazobactam and piperacillin. Table 1. Media used for preculture and MIC determination BHIB: Brain heart infusion broth (Difco),
CHEMOTHERAPY OCT. 1994 Tazobactam Piperacillin Fig. I. Chemical structures of tazobactam and piperacillin. Table 1. Media used for preculture and MIC determination BHIB: Brain heart infusion broth (Difco),
 Fig.1 MICs of penicillins against 24 strains of B. pertussis Fig.2 MICs of cepherns against 24 strains of B. pertussis Fig.3 MICs of macrolides against 24 strains of B. pertussis Fig.4 MICs of nalidixic
Fig.1 MICs of penicillins against 24 strains of B. pertussis Fig.2 MICs of cepherns against 24 strains of B. pertussis Fig.3 MICs of macrolides against 24 strains of B. pertussis Fig.4 MICs of nalidixic
(ABPC), Carbenicillin (CBPC), Surbenicillin (SBPC), Piperacillin (PIPC), Cephalexin (CEX), Cefaclor (CCL), Cephalothin (CET), Cefazolin (CEZ), Cefotia
 Key words: Blood culture, Trend of bacterial isolation, Increasing of staphylococcus, Use of new cephems (ABPC), Carbenicillin (CBPC), Surbenicillin (SBPC), Piperacillin (PIPC), Cephalexin (CEX), Cefaclor
Key words: Blood culture, Trend of bacterial isolation, Increasing of staphylococcus, Use of new cephems (ABPC), Carbenicillin (CBPC), Surbenicillin (SBPC), Piperacillin (PIPC), Cephalexin (CEX), Cefaclor
CHEMOTHERAPY Methicillin-resistant S.aureus(MRSA) coccus epidermidis 105 Streptococcus pyogenes E.faecali senterococcus avium Enterococcus faecium Str
 cefaclor(ccl),cefuroxime(cxm),cefixime (CFIX),cefteram(CFTM),cefdinir(CFDN) pneumoniae,streptococcus pyogenes Moraxella catarrhalis,haemophilus influenzae,escherichia coli, Klebsiella pneumoniae,proteus
cefaclor(ccl),cefuroxime(cxm),cefixime (CFIX),cefteram(CFTM),cefdinir(CFDN) pneumoniae,streptococcus pyogenes Moraxella catarrhalis,haemophilus influenzae,escherichia coli, Klebsiella pneumoniae,proteus
CHEMOTHERAPY
 CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of BRL 28500 against standard strains of bacteria Fig, 1 Sensitivity distribution of ABPC-resistant E. coli isolated from urinary tract Fig. 2 Sensitivity
CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of BRL 28500 against standard strains of bacteria Fig, 1 Sensitivity distribution of ABPC-resistant E. coli isolated from urinary tract Fig. 2 Sensitivity
R01
 1. 集計対象医療機関数 (1,792 医療機関 ) 13.2% (7 医療機関 ) 900 床以上 N=53 86.8% (46 医療機関 ) 19.2% (70 医療機関 ) 500 899 床 N=365 80.8% (295 医療機関 ) JANIS 参加 * 200 499 床 N=2,231 43.4% (968 医療機関 ) 56.6% (1,263 医療機関 ) JANIS 参加 200
1. 集計対象医療機関数 (1,792 医療機関 ) 13.2% (7 医療機関 ) 900 床以上 N=53 86.8% (46 医療機関 ) 19.2% (70 医療機関 ) 500 899 床 N=365 80.8% (295 医療機関 ) JANIS 参加 * 200 499 床 N=2,231 43.4% (968 医療機関 ) 56.6% (1,263 医療機関 ) JANIS 参加 200
特殊病態下感染症における抗菌薬治験の手引き作成委員会報告書(案)
 VOL.51 NO.6 JUNE 2003 JUNE 2003 9) Niederman MS et al: Guidelines for the management of adults with community-acquired pneumonia. Diagnosis, assessment of severity, antimicrobial therapy and prevention.
VOL.51 NO.6 JUNE 2003 JUNE 2003 9) Niederman MS et al: Guidelines for the management of adults with community-acquired pneumonia. Diagnosis, assessment of severity, antimicrobial therapy and prevention.
 b) Gram-negative bacteria Fig. 2 Sensitivity distribution of clinical isolates : E. coli Fig. 3 Sensitivity distribution of clinical isolates : Pseudomonas Fig. 1 Sensitivity distribution of clinical isolates
b) Gram-negative bacteria Fig. 2 Sensitivity distribution of clinical isolates : E. coli Fig. 3 Sensitivity distribution of clinical isolates : Pseudomonas Fig. 1 Sensitivity distribution of clinical isolates
CHEMOTHERAPY JUNE 1987 Table1 Media used *BHIB, brain heart infusion broth (Difco); /3 -NAD, S -nicotinamidoadeninedinucleotide (Sigma Chemical Co.);
 VOL.35 S-2 CHEMOTHERAPY Fig.1 Chemical structure of carumonam CHEMOTHERAPY JUNE 1987 Table1 Media used *BHIB, brain heart infusion broth (Difco); /3 -NAD, S -nicotinamidoadeninedinucleotide (Sigma Chemical
VOL.35 S-2 CHEMOTHERAPY Fig.1 Chemical structure of carumonam CHEMOTHERAPY JUNE 1987 Table1 Media used *BHIB, brain heart infusion broth (Difco); /3 -NAD, S -nicotinamidoadeninedinucleotide (Sigma Chemical
Fig.1 Chemical structure of BAY o 9867
 Fig.1 Chemical structure of BAY o 9867 CHEMOTHERAPY 43 Table 3 Antibacterial spectrum of gram negative bacteria Medium:Heart infusion agar (Nissui) Method:Agar dilution (Streak) CHEMOTHERAPY DEC 1985
Fig.1 Chemical structure of BAY o 9867 CHEMOTHERAPY 43 Table 3 Antibacterial spectrum of gram negative bacteria Medium:Heart infusion agar (Nissui) Method:Agar dilution (Streak) CHEMOTHERAPY DEC 1985
VOL.30 S-1 CHEMOTHERAPY Table 1 Antibacterial activity of CTT against standard strains Table 2 Antibacterial activity of CTT against standard strains
 CHEMOTHERAPY APR. 1982 Fig. 1 Chemical structure of cefotetan (CTT, YM09330) VOL.30 S-1 CHEMOTHERAPY Table 1 Antibacterial activity of CTT against standard strains Table 2 Antibacterial activity of CTT
CHEMOTHERAPY APR. 1982 Fig. 1 Chemical structure of cefotetan (CTT, YM09330) VOL.30 S-1 CHEMOTHERAPY Table 1 Antibacterial activity of CTT against standard strains Table 2 Antibacterial activity of CTT
180 ( 64 ) THE JAPANESE JOURNAL OF ANTIBIOTICS June 2011 A b group A Streptococcus: GAS GAS 10 meta-analysis 1) 2,3) GAS potential pathogens Tab
 June 2011 THE JAPANESE JOURNAL OF ANTIBIOTICS 64 23 179 ( 63 ) A b cefditoren pivoxil 5 amoxicillin 10 1,2) 1,3) 1) 1) 1) 4) 5) 6) 7) 1) 2) 3) 4) 5) 6) 7) 2011 4 8 2007 5 2009 4 A b GAS cefditoren pivoxil
June 2011 THE JAPANESE JOURNAL OF ANTIBIOTICS 64 23 179 ( 63 ) A b cefditoren pivoxil 5 amoxicillin 10 1,2) 1,3) 1) 1) 1) 4) 5) 6) 7) 1) 2) 3) 4) 5) 6) 7) 2011 4 8 2007 5 2009 4 A b GAS cefditoren pivoxil
VOL.42 S-1 methicillin-susceptible Staphylococcus aureus (MSSA), Staphylococcus epidermidis, Enterococcus faecalis, Escherichia coli, Klebsiella pneum
 VOL.42 S-1 methicillin-susceptible Staphylococcus aureus (MSSA), Staphylococcus epidermidis, Enterococcus faecalis, Escherichia coli, Klebsiella pneumoniae, Enterobacter cloacae methicillin-resistant Staphylococcus
VOL.42 S-1 methicillin-susceptible Staphylococcus aureus (MSSA), Staphylococcus epidermidis, Enterococcus faecalis, Escherichia coli, Klebsiella pneumoniae, Enterobacter cloacae methicillin-resistant Staphylococcus
CHEMOTHERAPY NOV S. aureus, S. epidermidis, E. coli, K. pgeumoniae, E. cloacae, S. marcescens, P. mirabilis, Proteus, P. aeruginosa Inoculum siz
 VOL.33 S-5 CHEMOTHERAPY 381 Fig. 1 Chemical structure of HAPA-B Chemical name 1-N-[(2S)-3-Amino-2-hydroxypropiony1]-4-0-(6-amino- 6-deoxy-a-D-glucopyranosyl)-6-013-deoxy-4-C-methyl- 3-(methylamino)-ƒÀ-L-arabinopyranosyl]-2-deoxystreptamine
VOL.33 S-5 CHEMOTHERAPY 381 Fig. 1 Chemical structure of HAPA-B Chemical name 1-N-[(2S)-3-Amino-2-hydroxypropiony1]-4-0-(6-amino- 6-deoxy-a-D-glucopyranosyl)-6-013-deoxy-4-C-methyl- 3-(methylamino)-ƒÀ-L-arabinopyranosyl]-2-deoxystreptamine
Nationwide surveillance of bacterial respiratory pathogens conducted by the Surveillance Committee of Japanese Society of Chemotherapy, Japanese Assoc
 J Infect Chemother (2012) 18:609 620 DOI 10.1007/s10156-012-0434-3 SURVEILLANCE Nationwide surveillance of bacterial respiratory pathogens conducted by the Surveillance Committee of Japanese Society of
J Infect Chemother (2012) 18:609 620 DOI 10.1007/s10156-012-0434-3 SURVEILLANCE Nationwide surveillance of bacterial respiratory pathogens conducted by the Surveillance Committee of Japanese Society of
CHEMOTHERAPY
 VOL.40 S-1 coagulase negative Staphylococcus sp, methicillin- resistant Staphylococcus aureus (MRSA), Enterococcus faecalis, Escherichia coli, Citrobacter freundii, Klebsiella pneumoniae, Enterobacter
VOL.40 S-1 coagulase negative Staphylococcus sp, methicillin- resistant Staphylococcus aureus (MRSA), Enterococcus faecalis, Escherichia coli, Citrobacter freundii, Klebsiella pneumoniae, Enterobacter
Feb THE JAPANESE JOURNAL OF ANTIBIOTICS ,4 2,4 2,4 2,3,4 2,3,4 2,3, ,3, Garenoxacin GRNX Levofloxacin LV
 Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 27 27 1,4 2,4 2,4 2,3,4 2,3,4 2,3,4 2 1 2,3,4 1 2 3 4 2015 10 21 9 Garenoxacin GRNX Levofloxacin LVFX Sitafloxacin STFX Moxifloxacin MFLX Pharmacokinetics-Pharmacodynamics
Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 27 27 1,4 2,4 2,4 2,3,4 2,3,4 2,3,4 2 1 2,3,4 1 2 3 4 2015 10 21 9 Garenoxacin GRNX Levofloxacin LVFX Sitafloxacin STFX Moxifloxacin MFLX Pharmacokinetics-Pharmacodynamics
VOL. 23 NO. 3 CHEMOTHERAPY 1067 Table 2 Sensitivity of gram positive cocci isolated from various diagnostic materials Table 3 Sensitivity of gram nega
 1066 CHEMOTHERAPY MAR. 1975 Table 1 Sensitivity of standard strains VOL. 23 NO. 3 CHEMOTHERAPY 1067 Table 2 Sensitivity of gram positive cocci isolated from various diagnostic materials Table 3 Sensitivity
1066 CHEMOTHERAPY MAR. 1975 Table 1 Sensitivity of standard strains VOL. 23 NO. 3 CHEMOTHERAPY 1067 Table 2 Sensitivity of gram positive cocci isolated from various diagnostic materials Table 3 Sensitivity
VOL.42 S-1
 CHEMOTHERAPY APR. 1994 VOL.42 S-1 CHEMOTHERAPY APR. 1994 Table 1. Criteria for evaluation of clinical efficacy by the Japanese Society of Oral and Maxillo-Facial Surgeons Grades of symptoms and numerical
CHEMOTHERAPY APR. 1994 VOL.42 S-1 CHEMOTHERAPY APR. 1994 Table 1. Criteria for evaluation of clinical efficacy by the Japanese Society of Oral and Maxillo-Facial Surgeons Grades of symptoms and numerical
CHEMO THE RAPY OCT. 1994
 bilis (0.78), Proteus vulgaris (1.56), Enterococcus faecalis (3.13), Staphylococcus epidermidis (6.25), Klebsiella pneumoniae (6.25), Morganella morganii (6.25), Escherichia coli (12.5), Providencia rettgeri
bilis (0.78), Proteus vulgaris (1.56), Enterococcus faecalis (3.13), Staphylococcus epidermidis (6.25), Klebsiella pneumoniae (6.25), Morganella morganii (6.25), Escherichia coli (12.5), Providencia rettgeri
 Table 1 Antibacterial spectra of CPM and other antimicrobials against anaerobes Fig. 1 In vitro activity of CPM and other antibiotics against B. fragilis (136 strains) Fig. 2 In vitro activity of CPM and
Table 1 Antibacterial spectra of CPM and other antimicrobials against anaerobes Fig. 1 In vitro activity of CPM and other antibiotics against B. fragilis (136 strains) Fig. 2 In vitro activity of CPM and
THE JAPANESE JOURNAL OF ANTIBIOTICS 67 3 June 2014 STFX mg mg mg mg mg 1
 June 2014 THE JAPANESE JOURNAL OF ANTIBIOTICS 67 3 175 29 1 2 2 2 2 2 3 4 4 5 5 2 2 1 2 3 4 5 2014 4 15 STFX 50 mg 10% 2011 8 1 100 mg 1 1 2011 12 2013 5 226 1,186 1,089 1,069 2.11% 23/1,089 1.10% 12/1,089
June 2014 THE JAPANESE JOURNAL OF ANTIBIOTICS 67 3 175 29 1 2 2 2 2 2 3 4 4 5 5 2 2 1 2 3 4 5 2014 4 15 STFX 50 mg 10% 2011 8 1 100 mg 1 1 2011 12 2013 5 226 1,186 1,089 1,069 2.11% 23/1,089 1.10% 12/1,089
CHEMOTHERAPY DEC (NFLX), ofloxacin (OFLX), ciprofloxacin (CPFX) Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, Enterococcus faecali
 CHEMOTHERAPY DEC. 1988 (NFLX), ofloxacin (OFLX), ciprofloxacin (CPFX) Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, Enterococcus faecalis Pseudomonas aeruginosa, Serratia ma- Fig. 1. Chemical
CHEMOTHERAPY DEC. 1988 (NFLX), ofloxacin (OFLX), ciprofloxacin (CPFX) Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, Enterococcus faecalis Pseudomonas aeruginosa, Serratia ma- Fig. 1. Chemical
 概要 (2004 年分 ) 本サーベイランスは 参加医療機関において血液および髄液から分離された各種細菌の検出状況や薬剤感受性パターンの動向を把握するとともに 新たな耐性菌の早期検出等を目的とする これらのデータを経時的に解析し臨床の現場に還元することによって 抗菌薬の安全で有効な使用方法や院内感染制御における具体的かつ確実な情報を提供する 検体 ( ) 内は施設数 2002 年 2003 年 2004
概要 (2004 年分 ) 本サーベイランスは 参加医療機関において血液および髄液から分離された各種細菌の検出状況や薬剤感受性パターンの動向を把握するとともに 新たな耐性菌の早期検出等を目的とする これらのデータを経時的に解析し臨床の現場に還元することによって 抗菌薬の安全で有効な使用方法や院内感染制御における具体的かつ確実な情報を提供する 検体 ( ) 内は施設数 2002 年 2003 年 2004
日本化学療法学会雑誌第53巻第S-3号
 moxifloxacin in vitro moxifloxacin in vitro 17 9 6 17 11 21 moxifloxacinmflx in vitro cefdinir CFDNclavulanic acidamoxicillincvaampcclarithromycincamclindamycincldm levofloxacinlvfx 1MFLX Clostridium clostridiiformeclostridium
moxifloxacin in vitro moxifloxacin in vitro 17 9 6 17 11 21 moxifloxacinmflx in vitro cefdinir CFDNclavulanic acidamoxicillincvaampcclarithromycincamclindamycincldm levofloxacinlvfx 1MFLX Clostridium clostridiiformeclostridium
CHEMOTHERAPY Table 1 Urinary excretion of mezlocillin Fig. 4 Urinary excretion of mezlocillin Fig. 3 Blood levels of mezlocillin
 CHEMOTHERAPY Fig. 2 Urinary excretion of mezlocillin Fig. 1 Blood levels of mezlocillin CHEMOTHERAPY Table 1 Urinary excretion of mezlocillin Fig. 4 Urinary excretion of mezlocillin Fig. 3 Blood levels
CHEMOTHERAPY Fig. 2 Urinary excretion of mezlocillin Fig. 1 Blood levels of mezlocillin CHEMOTHERAPY Table 1 Urinary excretion of mezlocillin Fig. 4 Urinary excretion of mezlocillin Fig. 3 Blood levels
 VOL.30 NO.12 CHEMOTHERAPY Fig. 1 Effect of temperature on the growth curve of A. calcoaceticus A. calcoaceticits Ac 54 A. calcoacetictts Ac 164 Fig. 2 Effect of medium ph on the growth curve of A. calcoaceticus
VOL.30 NO.12 CHEMOTHERAPY Fig. 1 Effect of temperature on the growth curve of A. calcoaceticus A. calcoaceticits Ac 54 A. calcoacetictts Ac 164 Fig. 2 Effect of medium ph on the growth curve of A. calcoaceticus
 概要 (2006 年 1 2 3 月分 ) 本サーベイランスは 参加医療機関において血液および髄液から分離された各種細菌の検出状況や薬剤感受性パターンの動 向を把握するとともに 新たな耐性菌の早期検出等を目的とする これらのデータを経時的に解析し臨床の現場に還元することによって 抗菌薬の安全で有効な使用方法や院内感染制御における具体的かつ確実な情報を提供する 検体 2005 年 2006 年 10~12
概要 (2006 年 1 2 3 月分 ) 本サーベイランスは 参加医療機関において血液および髄液から分離された各種細菌の検出状況や薬剤感受性パターンの動 向を把握するとともに 新たな耐性菌の早期検出等を目的とする これらのデータを経時的に解析し臨床の現場に還元することによって 抗菌薬の安全で有効な使用方法や院内感染制御における具体的かつ確実な情報を提供する 検体 2005 年 2006 年 10~12
小児感染症分離株における感受性サーベイランス
 小児感染症分離株における 感受性サーベイランス 公益社団法人日本化学療法学会, 一般社団法人日本感染症学会, 日本小児感染症学会小児用キノロン薬適正使用推進委員会委員長 : 渡辺彰委員 : 岩田敏, 坂田宏, 佐藤吉壮, 鈴木賢二, 宮下修行, 堀誠治, 山口禎夫協力委員 : 小田島正明, 交久瀬善隆, 長谷川寿一, 牧展子, 和田光市 はじめに 2009 年 12 月に耐性菌感染症治療のために二次選択薬として承認された小児用キノロン薬の再審査期間の
小児感染症分離株における 感受性サーベイランス 公益社団法人日本化学療法学会, 一般社団法人日本感染症学会, 日本小児感染症学会小児用キノロン薬適正使用推進委員会委員長 : 渡辺彰委員 : 岩田敏, 坂田宏, 佐藤吉壮, 鈴木賢二, 宮下修行, 堀誠治, 山口禎夫協力委員 : 小田島正明, 交久瀬善隆, 長谷川寿一, 牧展子, 和田光市 はじめに 2009 年 12 月に耐性菌感染症治療のために二次選択薬として承認された小児用キノロン薬の再審査期間の
 CHEMOTHERAPY APRIL 1992 Table 2. Concentration of meropenem in human prostatic fluid Table 1. Background of 21 chronic complicated UTI cases * NB + BPH, NB + Kidney tumor, NB + Kidney tuberculosis Table
CHEMOTHERAPY APRIL 1992 Table 2. Concentration of meropenem in human prostatic fluid Table 1. Background of 21 chronic complicated UTI cases * NB + BPH, NB + Kidney tumor, NB + Kidney tuberculosis Table
日本化学療法学会雑誌第50巻第6号
 13 11 30 14 4 22 Streptococcus pneumoniae Haemophilus influenzae amoxicillin AMPC cefditoren pivoxil CDTR AMPC 50 mg kg day CDTR 9mg kg day CDTR 18 mg kg day S. pneumoniae H. influenzae 8 17 25 1 25 S.
13 11 30 14 4 22 Streptococcus pneumoniae Haemophilus influenzae amoxicillin AMPC cefditoren pivoxil CDTR AMPC 50 mg kg day CDTR 9mg kg day CDTR 18 mg kg day S. pneumoniae H. influenzae 8 17 25 1 25 S.
VOL. 23 NO. 3 CHEMOTHERAPY 1379 Table 1 Susceptibility of clinical isolated strains to Tobramycin
 VOL. 23 NO. 3 CHEMOTHERAPY 1379 Table 1 Susceptibility of clinical isolated strains to Tobramycin 1380 CHEMOTHERAPY MAR. 1975 Table 2 Susceptibility of isolated Pseudomonas aeruginosa to various antibiotics
VOL. 23 NO. 3 CHEMOTHERAPY 1379 Table 1 Susceptibility of clinical isolated strains to Tobramycin 1380 CHEMOTHERAPY MAR. 1975 Table 2 Susceptibility of isolated Pseudomonas aeruginosa to various antibiotics
 CHEMOTHERAPY APRIL 1992 VOL. 40 S- 1 Table 1-1. Comparative in vitro activity of meropenem against clinical isolates CNS: coagulase-negative staphylococci CHEMOTHERAPY APRIL 1992 Table 1-2. Comparative
CHEMOTHERAPY APRIL 1992 VOL. 40 S- 1 Table 1-1. Comparative in vitro activity of meropenem against clinical isolates CNS: coagulase-negative staphylococci CHEMOTHERAPY APRIL 1992 Table 1-2. Comparative
Title 尿路感染症分離菌の年次的変遷と薬剤感受性の検討 ( ニューキノロン系を中心として ) 深津, 英捷 ; 本多, 靖明 ; 水本, 裕之 ; 瀧, 知弘 ; 三井, Author(s) 々村, 仁志 ; 羽田野, 幸夫 ; 平岩, 親輔 ; 吉川, 和宏 ; 山田彰 ; 瀬川, 昭夫 Ci
 Title 尿路感染症分離菌の年次的変遷と薬剤感受性の検討 ( ニューキノロン系を中心として ) 深津, 英捷 ; 本多, 靖明 ; 水本, 裕之 ; 瀧, 知弘 ; 三井, Author(s) 々村, 仁志 ; 羽田野, 幸夫 ; 平岩, 親輔 ; 吉川, 和宏 ; 山田彰 ; 瀬川, 昭夫 Citation 泌尿器科紀要 (1992), 38(11): 1215-1223 Issue Date
Title 尿路感染症分離菌の年次的変遷と薬剤感受性の検討 ( ニューキノロン系を中心として ) 深津, 英捷 ; 本多, 靖明 ; 水本, 裕之 ; 瀧, 知弘 ; 三井, Author(s) 々村, 仁志 ; 羽田野, 幸夫 ; 平岩, 親輔 ; 吉川, 和宏 ; 山田彰 ; 瀬川, 昭夫 Citation 泌尿器科紀要 (1992), 38(11): 1215-1223 Issue Date
208 ( 2 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 63 _ 3 June 2010 Cefditoren pivoxil (CDTR-PI) MS MS 10%
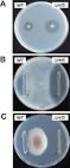 207 ( 1 ) Cefditoren pivoxil G 2010 2 2 2006 3 Cefditoren pivoxil CDTR-PI MS 10% CDTR-PI 305 2,144 2,006 1,958 1.79% 36 2,006 26 (1.30%) CDTR-PI CDTR-PI (9 mg/kg/day) 1.5 2 (2.70%) 2 (1.92%) 93.5% 1,831
207 ( 1 ) Cefditoren pivoxil G 2010 2 2 2006 3 Cefditoren pivoxil CDTR-PI MS 10% CDTR-PI 305 2,144 2,006 1,958 1.79% 36 2,006 26 (1.30%) CDTR-PI CDTR-PI (9 mg/kg/day) 1.5 2 (2.70%) 2 (1.92%) 93.5% 1,831
日本化学療法学会雑誌第59巻第5号
 Streptococcus pneumoniae Haemophilus influenzae Moraxella catarrhalis S. pneumoniae H. influenzae M. catarrhalis S. pneumoniae H. influenzae M. catarrhalis S. pneumoniae H. influenzae M. catarrhalis S.
Streptococcus pneumoniae Haemophilus influenzae Moraxella catarrhalis S. pneumoniae H. influenzae M. catarrhalis S. pneumoniae H. influenzae M. catarrhalis S. pneumoniae H. influenzae M. catarrhalis S.
CHEMOTHERAPY Table 1 Clinical effect of Sultamicillin
 CHEMOTHERAPY CHEMOTHERAPY Table 1 Clinical effect of Sultamicillin CHEMOTHERAPY Fig. 1 MICs of sultamicillin against respiratory pathogenic Branhamella catarrhalis 62 strains, inoculum size 106CFU/m1 Fig.
CHEMOTHERAPY CHEMOTHERAPY Table 1 Clinical effect of Sultamicillin CHEMOTHERAPY Fig. 1 MICs of sultamicillin against respiratory pathogenic Branhamella catarrhalis 62 strains, inoculum size 106CFU/m1 Fig.
2108 CHEMOTHERAPY SEPT Table 1 Antimicrobial spectrum Fig. 1
 2108 CHEMOTHERAPY SEPT. 1977 Table 1 Antimicrobial spectrum Fig. 1 VOL. 25 NO. 7 CHEM 014 HERAPY 2109 Table 2 Susceptibility distribution of Staphylococcus aureus to aminoglycosides (54 strains) Table
2108 CHEMOTHERAPY SEPT. 1977 Table 1 Antimicrobial spectrum Fig. 1 VOL. 25 NO. 7 CHEM 014 HERAPY 2109 Table 2 Susceptibility distribution of Staphylococcus aureus to aminoglycosides (54 strains) Table
スライド タイトルなし
 第 4 回ひびき臨床微生物シンポジュウム June 24,27, 港ハウス 感受性検査を読む ( 同定検査結果確認やスクリーニング検査と捉えて ) ( 株 ) キューリン小林とも子 キューリン微生物検査課 塗抹鏡検グラム染色 分離培養検査血液 BTB, エッグーヨーク 報告書作成結果承認 同定検査 VITEK TSI,LIM クリスタル NF 薬剤感受性検査 MIC2 ディスク法 薬剤感受性結果 (
第 4 回ひびき臨床微生物シンポジュウム June 24,27, 港ハウス 感受性検査を読む ( 同定検査結果確認やスクリーニング検査と捉えて ) ( 株 ) キューリン小林とも子 キューリン微生物検査課 塗抹鏡検グラム染色 分離培養検査血液 BTB, エッグーヨーク 報告書作成結果承認 同定検査 VITEK TSI,LIM クリスタル NF 薬剤感受性検査 MIC2 ディスク法 薬剤感受性結果 (
Clostridium difficile ciprofloxacin, ofloxacin, norfloxacin Bifidobacterium Lactobacillus Lactobacillus Bacteroides fragilis B. fragilis C. difficile
 Clostridium difficile ciprofloxacin, ofloxacin, norfloxacin Bifidobacterium Lactobacillus Lactobacillus Bacteroides fragilis B. fragilis C. difficile Key words: temafloxacin, TA-167, Bacteroides fragilis,
Clostridium difficile ciprofloxacin, ofloxacin, norfloxacin Bifidobacterium Lactobacillus Lactobacillus Bacteroides fragilis B. fragilis C. difficile Key words: temafloxacin, TA-167, Bacteroides fragilis,
08-g-”O−}„j‹ê-4.02
 200( 96 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 2 Apr. 585 1 17 MIC 1. (Transtracheal aspiration: TTA) TTA TTA TTA 1400 TTA (diffuse panbronchiolitis, DPB) 1) erythromycin(em) EM 12.5% 87.5% 2,3) EM EM
200( 96 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 2 Apr. 585 1 17 MIC 1. (Transtracheal aspiration: TTA) TTA TTA TTA 1400 TTA (diffuse panbronchiolitis, DPB) 1) erythromycin(em) EM 12.5% 87.5% 2,3) EM EM
日本化学療法学会雑誌第60巻第4号
 Streptococcus pneumoniae Haemophilus influenzae S. pneumoniae H. influenzae Key words β Streptococcus pneumoniae Haemophilus influenzae S. pneumoniae H. influenzae μ μ S. pneumoniae H. influenzae S. pneumoniae
Streptococcus pneumoniae Haemophilus influenzae S. pneumoniae H. influenzae Key words β Streptococcus pneumoniae Haemophilus influenzae S. pneumoniae H. influenzae μ μ S. pneumoniae H. influenzae S. pneumoniae
 Table 1.Concentration of gatifloxacin (Middle-ear) Table 2.Concentration of gatifloxacin (Paranasal sinuses) Table 3.Concentration of gatifloxacin (Tonsil) Table 4.No.of patients studied Table 5.Background
Table 1.Concentration of gatifloxacin (Middle-ear) Table 2.Concentration of gatifloxacin (Paranasal sinuses) Table 3.Concentration of gatifloxacin (Tonsil) Table 4.No.of patients studied Table 5.Background
Dec THE JAPANESE JOURNAL OF ANTIBIOTICS ( 45 ) ) 1) 2) 2) 3) 4) 4,5) 6) 6) 7) 8) 8) 9) 10) 11) 11) 12) 13) 13) 14) 14) 15) 15) 1
 Dec. 2010 THE JAPANESE JOURNAL OF ANTIBIOTICS 63 46 431 ( 45 ) 2006 1) 1) 2) 2) 3) 4) 4,5) 6) 6) 7) 8) 8) 9) 10) 11) 11) 12) 13) 13) 14) 14) 15) 15) 16) 16) 17) 17) 1) 1) 1) 2) 3) 4) 5) 6) 7) 8) 9) 10)
Dec. 2010 THE JAPANESE JOURNAL OF ANTIBIOTICS 63 46 431 ( 45 ) 2006 1) 1) 2) 2) 3) 4) 4,5) 6) 6) 7) 8) 8) 9) 10) 11) 11) 12) 13) 13) 14) 14) 15) 15) 16) 16) 17) 17) 1) 1) 1) 2) 3) 4) 5) 6) 7) 8) 9) 10)
公開情報 2016 年 1 月 ~12 月年報 ( 全集計対象医療機関 ) 院内感染対策サーベイランス検査部門 Citrobacter koseri Proteus mirabilis Proteus vulgaris Serratia marcescens Pseudomonas aerugino
 公開情報 2016 年 1 月 ~12 月年報 ( 全集計対象医療機関 ) 院内感染対策サーベイランス検査部門 検査部門におけるサーベイランスの概要と目的 本サーベイランスの目的は 細菌検査により検出される主要な細菌の分離頻度とその抗菌薬感受性を継続的に収集 解析し 医療機関における主要な細菌ならびに薬剤耐性菌の分離状況を明らかにすることである サーベイランスの対象となる主要菌ならびに薬剤耐性菌の分離率は
公開情報 2016 年 1 月 ~12 月年報 ( 全集計対象医療機関 ) 院内感染対策サーベイランス検査部門 検査部門におけるサーベイランスの概要と目的 本サーベイランスの目的は 細菌検査により検出される主要な細菌の分離頻度とその抗菌薬感受性を継続的に収集 解析し 医療機関における主要な細菌ならびに薬剤耐性菌の分離状況を明らかにすることである サーベイランスの対象となる主要菌ならびに薬剤耐性菌の分離率は
