CHEMOTHERAPY
|
|
|
- ねんたろう ひろもり
- 5 years ago
- Views:
Transcription
1
2 CHEMOTHERAPY
3 VOL.40 S-3
4 CHEMOTHERAPY
5 Table 1. No.of patients studied
6 CHEMOTHERAPY Table 2. Age of patients Minimum age: 16 years old Maximum age: 93 years old Table 3. Severity of illness of patients Table 4. Daily dose and treatment duration
7
8 CHEMOTHERAPY MAY 1992 Table 7. Relation of severity of illness to clinical efficacy classified by daily dose Excellent+good/no. of patients
9 VOL.40 S-3 Table 8. Relation of diagnosis with or without underlying disease and complication to clinical efficacy * Excellent+good/no. of patients ~100
10 CHEMOTHERAPY MAY 1992 Table 9. Clinical efficacy in respiratory tract infection classified by causative organisms * Excellent+good/no. of patients ~100
11 VOL.40 S-3 Table 10. Clinical efficacy in urinary tract infection classified by causative organisms * Excellent+good/no. of patients ~100 Table 11. Relation of daily dose to clinical efficacy (Granule) Excellent+good/no. of patients
12 CHEMOTHERAPY MAY 1992 Table 12. Bacteriological efficacy in respiratory tract infection classified by causative organisms 1) Eradication rate: eradicated+replaced/(no. of patients-unknown) ~100 (Excluded patients in whom bacteriological examination was not done or causative organism(s) could not be identified.) 2) Including 2 patients with normal flora at beginning of treatment and organisms appeared after treatment
13 VOL.40 S-3 Table 13. Bacteriological efficacy in urinary tract infection classified by causative organisms * Eradicated+replaced/(no. of patients-unknown) ~100
14 CHEMOTHERAPY MAY 1992 Table 14. Relation between MIC and bacteriological response in respiratory tract infection No. of strains eradicated / no. of strains isolated Table 15. Organisms appearing after treatment in respiratory tract infection
15 VOL.40 S-3 Table 16. Clinical adverse reactions Incidence in tablet: 3.4% (13/386), granule: 5.9% (4/68), total: 3.7% (17/454)
16 CHEMOTHERAPY MAY 1992 Table 17. Abnormal laboratory findings * According to the draft of criteria proposed by Japan Society of Chemotherapy
17 VOL.40 S-3 Table 18. Usefulness * Markedly useful+useful/no. of patients ~100
18 CHEMOTHERAPY MAY ) Atarashi S, Yokohama S, Yamazaki K, Sakano K, Imamura M, and Hayakawa I: Synthesis and antibacterial activities of optically active ofloxacin and its fluoromethyl derivative. Chem Pharm Bull 35: , ) Une T, Fujimoto T, Sato K, and Osada Y: In vitro activity of DR- 3355, an optically active ofloxacin. Antimicrob Agents Chemother 32: , ) Nakashima M, Uematsu T, Kanamaru M, Okazaki 0, Hashimoto S, and Tachizawa H: Pharmacokinetics of DR-3355, a new quinolone, in healthy volunteers. Program Abstr 28th ICAAC, abst. no. 951, 1988
19 CLINICAL STUDY ON LEVOFLOXACIN IN THE FIELD OF INTERNAL MEDICINE Atsushi Saito, Yoshiteru Shigeno, Yuei Irabu and Hiroshi Fukuhara The First Department of Internal Medicine, School of Medicine, University of the Ryukyus, 207 Uehara, Nishihara-cho, Nakagami-gun, Okinawa , Japan Akira Saito, Masumi Tomizawa and Ichiro Nakayama College of Medical Technology, Hokkaido University and Affiliated Hospitals Yohmei Hiraga and Mitsuhide Ohmichi Department of Respiratory Diseases, Sapporo Hospital of Hokkaido Railway Company, Sapporo, Japan Kazuo Takebe The Third Department of Internal Medicine, Hirosaki University School of Medicine Masashi Tamura, Kazuki Konishi, Yoshiaki Mori Akio Mizuno and Akiho Obara The Third Department of Internal Medicine, School of Medicine, Iwate Medical University Tamotsu Takishima and Yasuo Tanno The First Department of Internal Medicine, School of Medicine, Tohoku University Jun-ichi Masakichi Motomiya, Kotaro Oizumi#, Akira Watanabe, Yushi Nakai Saito, Kiyoshi Konno, Satoshi Shindo, Kosaku Nagai and Kazunao Niizuma Department of Internal Medicine, Research Institute for Chest Diseases and Cancer, Tohoku University and Affiliated Hospitals (*The First Department of Internal Medicine, Kurume University, School of Medicine) Masataka Katsu, Hiroshi Hirose and Masatoshi Ishii Department of Internal Medicine, Kasumigaura National Hospital Jingoro Shimada# #, Kohya Shiba, Masaki Yoshida and Osamu Sakai The Second Department of Internal Medicine, The Jikei University School of Medicine (##Department of Microbiology and Institute of Medical Science, St. Marianna University School of Medicine)
20 CHEMOTHERAPY Hiroichi Tanimoto and Kazuo Ohara The Fourth Department of Internal Medicine, The Jikei University School of Medicine Kihachiro Shimizu, Kyoichi Totsuka and Junichi Katahira Department of Internal Medicine, Tokyo Women's Medical College Kaoru Shimada, Hazime Goto, Shinichi Oka, Yoshihisa Ogata, Takashi Inamatsu, Yoshishige Masuda, Hiroshi Sakamoto, Fumiko Kojima, Makoto Kodaira, Yasuyuki Sano and Yasufumi Miyamoto Department of Infectious Disease, Institute of Medical Science, University of Tokyo and Affiliated Hospitals Hiroyuki Kobayashi The First Department of Internal Medicine, School of Medicine, Kyorin University Hideo Ikemoto, Takeshi Mori and Masayoshi Inagaki Department of Internal Medicine, Juntendo University School of Medicine Koichiro Nakata, Yoshitaka Nakamori and Tatsuo Nakatani Devision of Respiratory Diseases, Toranomon Hospital Takeshi Kawai and Mitsuo Honma Department of Internal Medicine, School of Medicine, Keio University Junzaburo Kabe, Koichiro Kudo and Hitoshi Arioka Department of Respiratory Disease, National Medical Center Hospital Masaru Koyama Department of Internal Medicine, Tokyo Kyosai Hospital Harumi Shishido Department of Respiratory Diseases, Tokyo National Chest Hospital Norio Kikuchi and Hidetoshi Igari Department of Internal Medicine, Chiba Kaihin Municipal Hospital Hiroshi Tabeta Department of Internal Medicine, Funabashi Municipal Medical Center Shigeki Odagiri, Kaneo Suzuki, Hiroshi Takahashi, Kenichi Takahashi, Yasuhiko Ashikari, Eri Hagiwara, Yasutsugu Amano and Akira Shohji Department of Respiratory Diseases, Kanagawa Prefectural Circulatory and Respiratory Diseases Center
21 Fumio Matsumoto and Takero Imai Department of Internal Medicine, Kanagawa Prefectural Midwives and Nurses Training School Hospital Shoichiro Irimajiri, Yasuo Matsuoka and Mitsuo Obana Department of Internal Medicine, Kawasaki Municipal Hospital Masaaki Arakawa, Kouichi Wada, Hiroki Tukada and Takashi Kawashima The Second Department of Internal Medicine, Niigata University, School of Medicine Osamu Sekine, Yasutoshi Suzuki and Katsuji Uno Department of Internal Medicine, Suibarago Hospital Nobuki Aoki Department of Internal Medicine, Shinrakuen Hospital Atsuhiko Sato, Masatoshi Iwata, Kingo Chida, Izumi Shichi, Hirokazu Okano, Masahiko Okano and Masami Taniguchi The Second Department of Internal Medicine, Hamamatsu University, School of Medicine and Affiliated Hospitals Tatsuo Satake, Kenzo Takagi, Kenichi Yamaki and Hiroyuki Miyatake The Second Department of Internal Medicine, Nagoya University School of Medicine Toshiyuki Yamamoto, Kanzo Suzuki, Satoru Adachi and Toru Matsuura Department of Internal Medicine, Nagoya-shi Koseiin Geriatric Hospital Fumiyuki Kuze, Tatsuyoshi Ikeue, Katsuhiro Suzuki, Kenji Bando, Masaru Chiba, Yoshinori Hasegawa, Ryuhei Nawata, Nobuo Inaba, Akira Kagioka and Mitsuo Hase The First Clinic of Medicine, Chest Disease Research Institute, Kyoto University and Affiliated Hospitals Eiro Tsubura###, Masaru Nakagawa, Susumu Kishimoto, Nakaaki Osawa, Iwao Igarashi, Kiyoshi Komuta, Keiji Maeda, Mitsunori Sakatani, Toshio Sone, Yasutake Takahashi, Tatsuya Okada, Mitsumasa Ogawara, Kazuya Higashino and Takashi Nakano Department of Internal Medicine, Toneyama National Hospital and Affiliated Hospitals (### Osaka Hospital, Anti-Tuberculosis Association Osaka Branch) Fumio Miki Department of Internal Medicine, Tane General Hospital Shigenori Nakashima, Atsushi Yasukawa The Fourth Department of Internal Medicine, Kinki University School of Medicine
22 CHEMOTHERAPY Nobuhiro Narita, Masayoshi Sawaki and Keiichi Mikasa The Second Department of Internal Medicine, Nara Medical College Rinzo Soejima, Niro Okimoto and Masaru Sumi Division of Respiratory Disease, Department of Medicine, Kawasaki Medical School Toshiharu Matsushima and Yoshihiko Tano The Second Department of Medicine, Kawasaki Medical School Kawasaki Hospital Takao Sasaki, Yukio Matsumoto and Yuji Sugimoto The Third Department of Internal Medicine, Tottori University, School of Medicine Michio Yamakido and Kenji Hasegawa The Second Department of Internal Medicine, Hiroshima University, School of Medicine Osamu Kurimura Department of Internal Medicine, Kure National Hospital Yoshiro Sawae, Koji Takagi and Nobuyuki Shimono School of Health Science, and First Department of Internal Medicine, Faculty of Medicine, Kyushu University Atsushi Shinoda, Tsuneo Ishibashi and Masahiro Takamoto Department of Internal Medicine, Ohmuta National Hospital Hozumi Yamada, Osamu Kato, Yosuke Aoki and Shigetaka Kuroki Department of Internal Medicine, Saga Medical School Kohei Hara, Hironobu Koga, Kiyoyasu Fukushima, Hisasuke Nakamura, Tetsuro Kanda, Miyako Ishiguro, Takakazu Kiya and Shiro Kusano The Second Department of Internal Medicine, School of Medicine, Nagasaki University and Affiliated Hospitals Keizo Matsumoto, Hironori Masaki and Hirofumi Tanaka Department of Internal Medicine, Institute of Tropical Medicine, Nagasaki University Masaru Nasu, Yoichiro Goto, Hiroyuki Nagai, Toru Yamasaki and Takayoshi Tashiro The Second Department of Internal Medicine, Medical College of Oita Shinobu Takenaka and Kiyoshi Shima Department of Internal Medicine, Kumamoto Municipal Hospital Mitsuo Kaku, Kazuyuki Sugawara and Keizo Yamaguchi # # # # Clinical Laboratory, Nagasaki University Hospital
23 Levofloxacin (LVFX), an optical isomer of ofloxacin (OFLX), is twice as potent as OFLX against gram-positive and gram-negative bacteria such as Haemophilus influenzae, Streptococcus pneumoniae and Pseudomonas aeruginosa, while it has been shown to be as safe as OFLX in animal experiments. Phase 1 study showed that the pharmacokinetics of LVFX were similar to those of OFLX. We carried out a multicenter collaborative trial at 69 institutions to determine the clinical efficacy and safety of LVFX in the field of internal medicine, mainly in the treatment of respiratory tract infections. LVFX was orally administered to 463 patients in daily doses of 200 mg to 600 mg for 7 to 14 consecutive days. Out of the total patients enrolled, the clinical efficacy was evaluated in 423 patients and was 84.9% (321/378) against respiratory tract infections, 78.8% (26/33) against urinary tract infections, 100% (9/9) against infectious enteritis and 100% (3/3) against other infections. As for respiratory tract infections, the efficacy rate was 90.6% (77/85) for pharyngitis and tonsillitis, 80.2% (174/217) for infectious exacerbation of chronic respiratory disease and 91.8% (67/73) for pneumonia. The efficacy rate, as a function of the daily dose, was 79.2% (38/48) with 100mg b.i.d., 85.5% (253/296) with 100mg t.i.d., 87.7% (50/57) with 200mg t.i.d., and 81.8% (18/22) with other dose regimens. The bacteriological response was evaluated in 179 patients and showed an eradication rate of 77.4% (123/159) for monomicrobial infections and 40.0% (8/20) for polymicrobial infections. The MIC was determined for 78 strains, and the eradication rate was 78.9% (56/71) for strains with an MIC value of 1.56 pg/ml or lower and 0.0% (0/7) for strains with an MIC value of 3.13,ug/ml or higher. Out of 454 patients, clinical adverse reactions were recorded in 17 (3.7%), consisting of gastrointestinal disorder in 9, neurogenic symptoms in 7 and other symptoms in 1. Abnormal laboratory findings were recorded in 41 (10.0%) out of 409 patients, the main item being elevation of the eosinophil count and the transaminase level. None of them were serious. Based on the above results, we concluded that LVFX is a useful antibacterial agent for the treatment of infections in the field of internal medicine, mainly respiratory tract infections.
CHEMOTHERAPY MAY 1992
 CHEMOTHERAPY MAY 1992 Fig. 1. Package of test drugs. CHEMOTHERAPY MAY 1992 VOL.40 S-3 Table 1. Items and schedule of laboratory tests CHEMOTHERAPY MAY 1992 Table 2. Evaluation criteria of symptoms, signs
CHEMOTHERAPY MAY 1992 Fig. 1. Package of test drugs. CHEMOTHERAPY MAY 1992 VOL.40 S-3 Table 1. Items and schedule of laboratory tests CHEMOTHERAPY MAY 1992 Table 2. Evaluation criteria of symptoms, signs
Table 1. Antibacterial activitiy of grepafloxacin and other antibiotics against clinical isolates
 Table 1. Antibacterial activitiy of grepafloxacin and other antibiotics against clinical isolates Table 2-1. Summary of patients treated with grepafloxacin for respiratory infection 1) Out: outpatient,
Table 1. Antibacterial activitiy of grepafloxacin and other antibiotics against clinical isolates Table 2-1. Summary of patients treated with grepafloxacin for respiratory infection 1) Out: outpatient,
CHEMOTHERAPY
 CHEMOTHERAPY VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin CHEMOTHERAPY AUG. 1993 VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin Table 1. Comparative in vitro activity of teicoplanin
CHEMOTHERAPY VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin CHEMOTHERAPY AUG. 1993 VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin Table 1. Comparative in vitro activity of teicoplanin
coccus aureus Corynebacterium sp, Haemophilus parainfluenzae Klebsiella pneumoniae Pseudornonas aeruginosa Pseudomonas sp., Xanthomonas maltophilia, F
 VOL.43 S-1 coccus aureus Corynebacterium sp, Haemophilus parainfluenzae Klebsiella pneumoniae Pseudornonas aeruginosa Pseudomonas sp., Xanthomonas maltophilia, Flavobacter- Table 1. Concentration of grepafloxacin
VOL.43 S-1 coccus aureus Corynebacterium sp, Haemophilus parainfluenzae Klebsiella pneumoniae Pseudornonas aeruginosa Pseudomonas sp., Xanthomonas maltophilia, Flavobacter- Table 1. Concentration of grepafloxacin
Key words: bacterial pneumonia, cefepime, ceftazidime, comparative study
 Key words: bacterial pneumonia, cefepime, ceftazidime, comparative study Staphylococcus aureus, Streptococcus influenzae, S. pneumoniae, Klebsiella Fig. 1 Chemical structure of cefepime Table 1 Clinical
Key words: bacterial pneumonia, cefepime, ceftazidime, comparative study Staphylococcus aureus, Streptococcus influenzae, S. pneumoniae, Klebsiella Fig. 1 Chemical structure of cefepime Table 1 Clinical
Key words : 7432-S, Oral cephem, Urinary tract infection Fig. 1. Chemical structure of 7432-S.
 Key words : 7432-S, Oral cephem, Urinary tract infection Fig. 1. Chemical structure of 7432-S. Table 1. Clinical summary of acute uncomplicated cystitis patients treated with 7432-S UTI : Criteria by the
Key words : 7432-S, Oral cephem, Urinary tract infection Fig. 1. Chemical structure of 7432-S. Table 1. Clinical summary of acute uncomplicated cystitis patients treated with 7432-S UTI : Criteria by the
Fig.2. Sensitivity distribution of clinical isolates of S. epidermidis (24 strains, 106 CFU/ml) Staphylococcus aureus Staphylococcus epider- midis Ent
 Fig.2. Sensitivity distribution of clinical isolates of S. epidermidis (24 strains, 106 CFU/ml) Staphylococcus aureus Staphylococcus epider- midis Enterococcus faecalis Klebsiella pneumoniae, Morganella
Fig.2. Sensitivity distribution of clinical isolates of S. epidermidis (24 strains, 106 CFU/ml) Staphylococcus aureus Staphylococcus epider- midis Enterococcus faecalis Klebsiella pneumoniae, Morganella
VOL.42 S-1
 CHEMOTHERAPY APR. 1994 VOL.42 S-1 CHEMOTHERAPY APR. 1994 Table 1. Criteria for evaluation of clinical efficacy by the Japanese Society of Oral and Maxillo-Facial Surgeons Grades of symptoms and numerical
CHEMOTHERAPY APR. 1994 VOL.42 S-1 CHEMOTHERAPY APR. 1994 Table 1. Criteria for evaluation of clinical efficacy by the Japanese Society of Oral and Maxillo-Facial Surgeons Grades of symptoms and numerical
Fig. 1 Chemical structure of DL-8280
 Fig. 1 Chemical structure of DL-8280 Fig. 2 Susceptibility of cl in ical isolates to DL4280 Fig. 5 Susceptibility of clinical isolates to DL-8280 Fig. 3 Susceptibility of clinical isolates to DL-8280 Fig.
Fig. 1 Chemical structure of DL-8280 Fig. 2 Susceptibility of cl in ical isolates to DL4280 Fig. 5 Susceptibility of clinical isolates to DL-8280 Fig. 3 Susceptibility of clinical isolates to DL-8280 Fig.
CHEMOTHERAPY Fig. 1 Chemical structure of CXM-AX
 Fig. 1 Chemical structure of CXM-AX NOV. 1986 Fig. 2 Sensitivity distribution of clinical isolates organisms (106 cells/ml) a Smurcus 27 strains d) P.m irabilis 15 strains b Ecol i 27 strains 111.morganii
Fig. 1 Chemical structure of CXM-AX NOV. 1986 Fig. 2 Sensitivity distribution of clinical isolates organisms (106 cells/ml) a Smurcus 27 strains d) P.m irabilis 15 strains b Ecol i 27 strains 111.morganii
CHEMOTHERAPY FEB Table 1. Activity of cefpirome and others against clinical isolates
 VOL.39 S-1 CHEMOTHERAPY FEB. 1981 Table 1. Activity of cefpirome and others against clinical isolates VOL.39 S-1 CHEMOTHERAPY FEB. 1991 72 M, 55.5 kg 66 F, 53 kg Chronic bronchitis Bronchopneumonia Peak
VOL.39 S-1 CHEMOTHERAPY FEB. 1981 Table 1. Activity of cefpirome and others against clinical isolates VOL.39 S-1 CHEMOTHERAPY FEB. 1991 72 M, 55.5 kg 66 F, 53 kg Chronic bronchitis Bronchopneumonia Peak
CHEMOTHERAPY JUN Citrobacter freundii 27, Enterobacter aerogenes 26, Enterobacter cloacae 27, Proteus rettgeri 7, Proteus inconstans 20, Proteus
 VOL. 32 S-4 CHEMOTHERAPY Fig. 1 Chemical structure of sodium cefoperazone Fig. 2 Chemical structure of sodium cefoperazone CHEMOTHERAPY JUN. 1984 Citrobacter freundii 27, Enterobacter aerogenes 26, Enterobacter
VOL. 32 S-4 CHEMOTHERAPY Fig. 1 Chemical structure of sodium cefoperazone Fig. 2 Chemical structure of sodium cefoperazone CHEMOTHERAPY JUN. 1984 Citrobacter freundii 27, Enterobacter aerogenes 26, Enterobacter
Key words: RU 28965, roxithromycin, midecamycin acetate Pneumonia, double-blind method
 Key words: RU 28965, roxithromycin, midecamycin acetate Pneumonia, double-blind method Fig. 1 Chemical structure of RU Table 1 Evaluation criteria for signs, symptoms and laboratory findings 1) M: mucous
Key words: RU 28965, roxithromycin, midecamycin acetate Pneumonia, double-blind method Fig. 1 Chemical structure of RU Table 1 Evaluation criteria for signs, symptoms and laboratory findings 1) M: mucous
JULY 1995
 VOL. 43 S-1 JULY 1995 VOL. 43 S-1 Table 1. Patients evaluated and reasons for exclusion Table 2. Background of patients (No. of patients evaluated) Table 3. Number of patients classified by daily dose
VOL. 43 S-1 JULY 1995 VOL. 43 S-1 Table 1. Patients evaluated and reasons for exclusion Table 2. Background of patients (No. of patients evaluated) Table 3. Number of patients classified by daily dose
CHEMOTHERAPY aureus 0.10, Enterococcus faecalis 3.13, Escherichia coli 0.20, Klebsiella pneumoniae, Enterobacter spp., Serratia marcescens 0.78, Prote
 aureus 0.10, Enterococcus faecalis 3.13, Escherichia coli 0.20, Klebsiella pneumoniae, Enterobacter spp., Serratia marcescens 0.78, Proteus mirabilis 3.13, Proteus vulgaris 1.56, Citrobacter freundii 0.39,
aureus 0.10, Enterococcus faecalis 3.13, Escherichia coli 0.20, Klebsiella pneumoniae, Enterobacter spp., Serratia marcescens 0.78, Proteus mirabilis 3.13, Proteus vulgaris 1.56, Citrobacter freundii 0.39,
366 12 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 Dec. 2012 1 8 DNA 2,3 16 12 20 171 2008 12 2010 11 2 3,558 4.44% 1.65% 1.17% 90% 9 Escherichia coli -
 Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 365 11 sita oxacin 1 1 1 1 1 1 2 2 3 3 1 1 1 2 3 2012 9 14 sita oxacin STFX 50 mg 10% 2008 1 2008 12 2010 11 2 STFX 1,452 91.4% 1,235/1,351 95.9% 466/486
Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 365 11 sita oxacin 1 1 1 1 1 1 2 2 3 3 1 1 1 2 3 2012 9 14 sita oxacin STFX 50 mg 10% 2008 1 2008 12 2010 11 2 STFX 1,452 91.4% 1,235/1,351 95.9% 466/486
 CHEMOTHERAPY APRIL 1992 Table 2. Concentration of meropenem in human prostatic fluid Table 1. Background of 21 chronic complicated UTI cases * NB + BPH, NB + Kidney tumor, NB + Kidney tuberculosis Table
CHEMOTHERAPY APRIL 1992 Table 2. Concentration of meropenem in human prostatic fluid Table 1. Background of 21 chronic complicated UTI cases * NB + BPH, NB + Kidney tumor, NB + Kidney tuberculosis Table
400 46 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 Dec. 2012 LVFX 100 mg 3 / 7 150 mg 2 / 7 2 2006 2008 9 LVFX PK PD 2009 7 100 mg 1 3 500 mg 1 1 AUC/MIC
 Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 399 45 2012 11 5 LVFX 500 mg 1 1 20 Chlamydia trachomatis C. trachomatismycoplasma genitalium M. genitalium LVFX 1 500 mg 1 1 7 22 22 C. trachomatis 17
Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 399 45 2012 11 5 LVFX 500 mg 1 1 20 Chlamydia trachomatis C. trachomatismycoplasma genitalium M. genitalium LVFX 1 500 mg 1 1 7 22 22 C. trachomatis 17
 Table 1.Concentration of gatifloxacin (Middle-ear) Table 2.Concentration of gatifloxacin (Paranasal sinuses) Table 3.Concentration of gatifloxacin (Tonsil) Table 4.No.of patients studied Table 5.Background
Table 1.Concentration of gatifloxacin (Middle-ear) Table 2.Concentration of gatifloxacin (Paranasal sinuses) Table 3.Concentration of gatifloxacin (Tonsil) Table 4.No.of patients studied Table 5.Background
Staphylococcus aureus (MSSA), Streptococcus pneumoniae, Enterococcus faecalis Pseudomonas aeru- ginosa, Enterobacter cloacae, Citrobacter freun- Fig.
 Key words : cefluprenam, seven days therapy, respiratory tract infection Staphylococcus aureus (MSSA), Streptococcus pneumoniae, Enterococcus faecalis Pseudomonas aeru- ginosa, Enterobacter cloacae, Citrobacter
Key words : cefluprenam, seven days therapy, respiratory tract infection Staphylococcus aureus (MSSA), Streptococcus pneumoniae, Enterococcus faecalis Pseudomonas aeru- ginosa, Enterobacter cloacae, Citrobacter
04-c-„FŒ{›xŒ¾-4.01
 544( 56 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 Dec. 25 2003 2. * * Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 545( 57 ) 9 5 2003 8 2004 714 565 719 50 20 39 0 9 70 79 44.4 91.7% Escherichia coli
544( 56 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 Dec. 25 2003 2. * * Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 545( 57 ) 9 5 2003 8 2004 714 565 719 50 20 39 0 9 70 79 44.4 91.7% Escherichia coli
CHEMOTHERAPY JUNE 1993 Table 1. Background of patients in pharmacokinetic study
 CHEMOTHERAPY JUNE 1993 Table 1. Background of patients in pharmacokinetic study VOL. 41 S 1 Table 2. Levels (Đg/ml or Đg/g) of S-1006 in serum, bile, and tissue (gallbladder) after oral administration
CHEMOTHERAPY JUNE 1993 Table 1. Background of patients in pharmacokinetic study VOL. 41 S 1 Table 2. Levels (Đg/ml or Đg/g) of S-1006 in serum, bile, and tissue (gallbladder) after oral administration
VOL.35 S-2 CHEMOTHERAPY Table 1 Sex and age distribution Table 2 Applications of treatment with carumonam Table 3 Concentration of carumonam in human
 CHEMOTHERAPY Fig. 1 Chemical structure of carumonam Disodium(+)-(Z)-CCE1-(2-amino-4-thiazoly1)-2-[[(2S, -(carbamoyloxymethyl)-4-oxo-1-sulfonato-3-azetidinyll -2-oxoethylidene] amino] oxy] acetate 3S)-2
CHEMOTHERAPY Fig. 1 Chemical structure of carumonam Disodium(+)-(Z)-CCE1-(2-amino-4-thiazoly1)-2-[[(2S, -(carbamoyloxymethyl)-4-oxo-1-sulfonato-3-azetidinyll -2-oxoethylidene] amino] oxy] acetate 3S)-2
Table 1 Classification of female patients with vesical irritating symptom by their signs : Urinary pain with or without other vesical irritability. s
 Table 1 Classification of female patients with vesical irritating symptom by their signs : Urinary pain with or without other vesical irritability. s Vesical irritability without urinary Pain. Pyuria 10/
Table 1 Classification of female patients with vesical irritating symptom by their signs : Urinary pain with or without other vesical irritability. s Vesical irritability without urinary Pain. Pyuria 10/
pneumoniae 30, C. freundii 32, E. aerogenes 27, E. cloacae 32, P. mirabilis 31, P. vulgaris 34, M. morganii 32, S. marcescens 31, H. influenzae 27, P.
 pneumoniae 30, C. freundii 32, E. aerogenes 27, E. cloacae 32, P. mirabilis 31, P. vulgaris 34, M. morganii 32, S. marcescens 31, H. influenzae 27, P. aeruginosa 30, P. maltophilia pyogenes 32, Escherichia
pneumoniae 30, C. freundii 32, E. aerogenes 27, E. cloacae 32, P. mirabilis 31, P. vulgaris 34, M. morganii 32, S. marcescens 31, H. influenzae 27, P. aeruginosa 30, P. maltophilia pyogenes 32, Escherichia
epidermidis, Enterococcus faecalis, Enterococcus Klebsiella pneumoniae, Proteus mirabilis, indolepositive Proteus spp., Enterobacter spp., Serratia
 epidermidis, Enterococcus faecalis, Enterococcus Klebsiella pneumoniae, Proteus mirabilis, indolepositive Proteus spp., Enterobacter spp., Serratia Table 3. Overall clinical efficacy of cefozopran in
epidermidis, Enterococcus faecalis, Enterococcus Klebsiella pneumoniae, Proteus mirabilis, indolepositive Proteus spp., Enterobacter spp., Serratia Table 3. Overall clinical efficacy of cefozopran in
 Key words: pazufloxacin, infectious enteritis, antibacterial activity, fecal concentration, fecal microflora : Table 1-1 Criteria for bacteriological efficacy of pazufloxacin on Shigella spp. and V. cholerae
Key words: pazufloxacin, infectious enteritis, antibacterial activity, fecal concentration, fecal microflora : Table 1-1 Criteria for bacteriological efficacy of pazufloxacin on Shigella spp. and V. cholerae
JUNE 2000
 VOL.48 NO.6 JUNE 2000 VOL.48 NO.6 Fig. 1. Chemical structure of pazufloxacin and pazufloxacin mesilate. JUNE 2000 VOL.48 NO.6 JUNE 2000 Table 1. Items and schedule of laboratory tests VOL.48 NO.6 Table
VOL.48 NO.6 JUNE 2000 VOL.48 NO.6 Fig. 1. Chemical structure of pazufloxacin and pazufloxacin mesilate. JUNE 2000 VOL.48 NO.6 JUNE 2000 Table 1. Items and schedule of laboratory tests VOL.48 NO.6 Table
VOL.30 S-1 CHEMOTHERAPY Table 1 Antibacterial activity of CTT against standard strains Table 2 Antibacterial activity of CTT against standard strains
 CHEMOTHERAPY APR. 1982 Fig. 1 Chemical structure of cefotetan (CTT, YM09330) VOL.30 S-1 CHEMOTHERAPY Table 1 Antibacterial activity of CTT against standard strains Table 2 Antibacterial activity of CTT
CHEMOTHERAPY APR. 1982 Fig. 1 Chemical structure of cefotetan (CTT, YM09330) VOL.30 S-1 CHEMOTHERAPY Table 1 Antibacterial activity of CTT against standard strains Table 2 Antibacterial activity of CTT
VOL. 45 NO. 6 Fig. 1. Chemical structure of grepafloxacin.
 JUNE 1997 VOL. 45 NO. 6 Fig. 1. Chemical structure of grepafloxacin. JUNE 1997 GPFX: grepafloxacin, OFLX: ofloxacin Fig. 2. Package of test drugs. VOL. 45 NO. 6 Table 1, Clinical study items and schedule
JUNE 1997 VOL. 45 NO. 6 Fig. 1. Chemical structure of grepafloxacin. JUNE 1997 GPFX: grepafloxacin, OFLX: ofloxacin Fig. 2. Package of test drugs. VOL. 45 NO. 6 Table 1, Clinical study items and schedule
CHEMOTHERAPY Table 1 Clinical effect of Sultamicillin
 CHEMOTHERAPY CHEMOTHERAPY Table 1 Clinical effect of Sultamicillin CHEMOTHERAPY Fig. 1 MICs of sultamicillin against respiratory pathogenic Branhamella catarrhalis 62 strains, inoculum size 106CFU/m1 Fig.
CHEMOTHERAPY CHEMOTHERAPY Table 1 Clinical effect of Sultamicillin CHEMOTHERAPY Fig. 1 MICs of sultamicillin against respiratory pathogenic Branhamella catarrhalis 62 strains, inoculum size 106CFU/m1 Fig.
Staphylococcus sp. K.pneumoniae P.mirabilis C.freundii E. cloacae Serratia sp. P. aeruginosa ml, Enterococcus avium >100ƒÊg/ml
 CHEMOTHERAPY SEPT. 1992 cefoperazone ceftazidime (CAZ), imipenem (IPM) Staphylococcus sp., Enterococcus (CPZ), faecalis, Escherichia coli, Klebsiella pneumoniae, Citrobacter freundii, Enterobacter cloacae,
CHEMOTHERAPY SEPT. 1992 cefoperazone ceftazidime (CAZ), imipenem (IPM) Staphylococcus sp., Enterococcus (CPZ), faecalis, Escherichia coli, Klebsiella pneumoniae, Citrobacter freundii, Enterobacter cloacae,
VOL.42 S-1 methicillin-susceptible Staphylococcus aureus (MSSA), Staphylococcus epidermidis, Enterococcus faecalis, Escherichia coli, Klebsiella pneum
 VOL.42 S-1 methicillin-susceptible Staphylococcus aureus (MSSA), Staphylococcus epidermidis, Enterococcus faecalis, Escherichia coli, Klebsiella pneumoniae, Enterobacter cloacae methicillin-resistant Staphylococcus
VOL.42 S-1 methicillin-susceptible Staphylococcus aureus (MSSA), Staphylococcus epidermidis, Enterococcus faecalis, Escherichia coli, Klebsiella pneumoniae, Enterobacter cloacae methicillin-resistant Staphylococcus
Fig. 1 Chemical structure of KW-1070
 Fig. 1 Chemical structure of KW-1070 Fig. 2 Sensitivity distribution of clinical isolates Fig. 4 Sensitivity distribution of clinical isolates Fig. 3 Sensitivity distribution of clinical isolates Fig.
Fig. 1 Chemical structure of KW-1070 Fig. 2 Sensitivity distribution of clinical isolates Fig. 4 Sensitivity distribution of clinical isolates Fig. 3 Sensitivity distribution of clinical isolates Fig.
Table 1. Antibacterial spectrum SBT ABPC ABPC CPZ : sulbactamiampicillin : ampicillin : cefoperazone
 Table 1. Antibacterial spectrum SBT ABPC ABPC CPZ : sulbactamiampicillin : ampicillin : cefoperazone (inoculum size= 106 CFU/ml) (Ĉ-lactamase producer : 2 strains) Fig. 1. Sensitivity distribution of
Table 1. Antibacterial spectrum SBT ABPC ABPC CPZ : sulbactamiampicillin : ampicillin : cefoperazone (inoculum size= 106 CFU/ml) (Ĉ-lactamase producer : 2 strains) Fig. 1. Sensitivity distribution of
 CHEMOTHERAPY APRIL 1992 VOL. 40 S- 1 Table 1-1. Comparative in vitro activity of meropenem against clinical isolates CNS: coagulase-negative staphylococci CHEMOTHERAPY APRIL 1992 Table 1-2. Comparative
CHEMOTHERAPY APRIL 1992 VOL. 40 S- 1 Table 1-1. Comparative in vitro activity of meropenem against clinical isolates CNS: coagulase-negative staphylococci CHEMOTHERAPY APRIL 1992 Table 1-2. Comparative
CHEMOTHERAPY MAY. 1988
 CHEMOTHERAPY MAY. 1988 CHEMOTHERAPY Fig. 1 Chemical structure CHEMOTHERAPY MAY. 1988 VOL.36 5-1 CHEMOTHERAPY CHEMOTHERAPY MAY. 1988 VOL.36 S-1 CHEMOTHERAPY CHEMOTHERAPY MAY. 1988 VOL.36 S-1 CHEMOTHERAPY
CHEMOTHERAPY MAY. 1988 CHEMOTHERAPY Fig. 1 Chemical structure CHEMOTHERAPY MAY. 1988 VOL.36 5-1 CHEMOTHERAPY CHEMOTHERAPY MAY. 1988 VOL.36 S-1 CHEMOTHERAPY CHEMOTHERAPY MAY. 1988 VOL.36 S-1 CHEMOTHERAPY
 Takeji NISHIKAWA, M. D.*, Takashi HARADA, M. D.** and Tatsuya IZUML M. D. Toshiyuki SUGI, M. D. Hiroshi HANYAKU, M. D. Shun-ichi MIYAKAWA, M. D. and Masaru TANAKA, M. D. Nobuko INAMOTO, M. D. and Hironori
Takeji NISHIKAWA, M. D.*, Takashi HARADA, M. D.** and Tatsuya IZUML M. D. Toshiyuki SUGI, M. D. Hiroshi HANYAKU, M. D. Shun-ichi MIYAKAWA, M. D. and Masaru TANAKA, M. D. Nobuko INAMOTO, M. D. and Hironori
Hisao Takayasu Department of Urology, Faculty of Medicine, University of Tokyo Masaaki Ohkoshi Department of Urology, Tokai University School of Medic
 COMPARATIVE CLINICAL EFFECT OF AMIKACIN AND GENTAMICIN ON COMPLICATED URINARY TRACT INFECTIONS BY DOUBLE-BLIND METHOD Tsuneo Nishiura and Yukimichi Kawada Department of Urology, Gifu University School
COMPARATIVE CLINICAL EFFECT OF AMIKACIN AND GENTAMICIN ON COMPLICATED URINARY TRACT INFECTIONS BY DOUBLE-BLIND METHOD Tsuneo Nishiura and Yukimichi Kawada Department of Urology, Gifu University School
 Table 1 Sensitivity distribution of clinical isolates 1. Escherichia coli Inoculum size: 106cells/ml 2. Klebsiella pneumoniae 3. Enterobacter cloacae 4. Serratia marcescens Inoculum size: 106cells/nil
Table 1 Sensitivity distribution of clinical isolates 1. Escherichia coli Inoculum size: 106cells/ml 2. Klebsiella pneumoniae 3. Enterobacter cloacae 4. Serratia marcescens Inoculum size: 106cells/nil
Fig. 1 Chemical structure of norfioxacin (AM-715)
 Fig. 1 Chemical structure of norfioxacin (AM-715) Table 1 Serum and biliary concentration of norfloxacin (AM-715) Table 2 Protocol for clinical evaluation of norfloxacin (AM-715) in the treatment of biliary
Fig. 1 Chemical structure of norfioxacin (AM-715) Table 1 Serum and biliary concentration of norfloxacin (AM-715) Table 2 Protocol for clinical evaluation of norfloxacin (AM-715) in the treatment of biliary
VOL. 40 S- 1 Table 1. Susceptibility of methicillin-resistant Staphylococcus aureus to meropenem Table 2. Coagulase typing of methicillin-resistant St
 CHEMOTHERAPY VOL. 40 S- 1 Table 1. Susceptibility of methicillin-resistant Staphylococcus aureus to meropenem Table 2. Coagulase typing of methicillin-resistant Staphylococcus aureus CHEMOTHERAPY Table
CHEMOTHERAPY VOL. 40 S- 1 Table 1. Susceptibility of methicillin-resistant Staphylococcus aureus to meropenem Table 2. Coagulase typing of methicillin-resistant Staphylococcus aureus CHEMOTHERAPY Table
Key Words: Cefuzonam, Cefotiam Bacterial Pneumoniae Comparative study
 Key Words: Cefuzonam, Cefotiam Bacterial Pneumoniae Comparative study Fig. 1 Chemical structure of CZON Table 1 Collaborating clinics Division of Respiratory Diseases, Department of Medicine, Kawasaki
Key Words: Cefuzonam, Cefotiam Bacterial Pneumoniae Comparative study Fig. 1 Chemical structure of CZON Table 1 Collaborating clinics Division of Respiratory Diseases, Department of Medicine, Kawasaki
Key words: Respiratory tract infections, Comparative study, Cefodizime, Cefotaxime
 Key words: Respiratory tract infections, Comparative study, Cefodizime, Cefotaxime Fig. 1 Chemical structure of Cefodizime Table 1 Collaborating clinics The Third Department of Internal Medicine, Hirosaki
Key words: Respiratory tract infections, Comparative study, Cefodizime, Cefotaxime Fig. 1 Chemical structure of Cefodizime Table 1 Collaborating clinics The Third Department of Internal Medicine, Hirosaki
 Table 1. Influence of urine ph on MBCs of new quinolones against Escherichia coli NIHJ JC-2 and Pseudomonas aeruginosa 18S; MBCs in urine were compared with those in Miieller-Hinton broth. Table 2. Influence
Table 1. Influence of urine ph on MBCs of new quinolones against Escherichia coli NIHJ JC-2 and Pseudomonas aeruginosa 18S; MBCs in urine were compared with those in Miieller-Hinton broth. Table 2. Influence
VOL. 23 NO. 3 CHEMOTHERAPY 1067 Table 2 Sensitivity of gram positive cocci isolated from various diagnostic materials Table 3 Sensitivity of gram nega
 1066 CHEMOTHERAPY MAR. 1975 Table 1 Sensitivity of standard strains VOL. 23 NO. 3 CHEMOTHERAPY 1067 Table 2 Sensitivity of gram positive cocci isolated from various diagnostic materials Table 3 Sensitivity
1066 CHEMOTHERAPY MAR. 1975 Table 1 Sensitivity of standard strains VOL. 23 NO. 3 CHEMOTHERAPY 1067 Table 2 Sensitivity of gram positive cocci isolated from various diagnostic materials Table 3 Sensitivity
1272 CHEMOTHERAPY MAR. 1975
 1272 CHEMOTHERAPY MAR. 1975 VOL. 23 NO. 3 CHEMOTHERAPY 1273 Fig. 2 Minimal inhibitory concentration of aminoglycosides against 50 strains of Klebsiella Fig. 1 Minimal inhibitory concentration of aminoglycosides
1272 CHEMOTHERAPY MAR. 1975 VOL. 23 NO. 3 CHEMOTHERAPY 1273 Fig. 2 Minimal inhibitory concentration of aminoglycosides against 50 strains of Klebsiella Fig. 1 Minimal inhibitory concentration of aminoglycosides
Key words: HAPA-B, AMK, Comparative study, Respiratory tract infections
 Key words: HAPA-B, AMK, Comparative study, Respiratory tract infections Fig. 1 Chemical structure of HAPA-B Table 1 Collaborating clinics The First Department of Internal Medicine, Kyorin University, School
Key words: HAPA-B, AMK, Comparative study, Respiratory tract infections Fig. 1 Chemical structure of HAPA-B Table 1 Collaborating clinics The First Department of Internal Medicine, Kyorin University, School
Key words: Respiratory tract infections, comparative study, ceftriaxone, cefotaxime
 Key words: Respiratory tract infections, comparative study, ceftriaxone, cefotaxime Table 1 Stability of CTRX and CTX Fig.1 Items and Schedule of Laboratory Test indispensable ~: should be performed as
Key words: Respiratory tract infections, comparative study, ceftriaxone, cefotaxime Table 1 Stability of CTRX and CTX Fig.1 Items and Schedule of Laboratory Test indispensable ~: should be performed as
 Table 1 Classification of female patients with vealcal irritating symptom by their signs Urination pain with other vesical irritability or not Table 2 Serum levels of DL-8280 after a single oral administration
Table 1 Classification of female patients with vealcal irritating symptom by their signs Urination pain with other vesical irritability or not Table 2 Serum levels of DL-8280 after a single oral administration
Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS XXXVII (45)
 Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS XXXVII-12 2305(45) 2306(46) THE JAPANESE JOURNAL OF ANTIBIOTICS XXXVII-12 Dec. Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS XXXVII-12 2307(47) 2308(48) THE JAPANESE
Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS XXXVII-12 2305(45) 2306(46) THE JAPANESE JOURNAL OF ANTIBIOTICS XXXVII-12 Dec. Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS XXXVII-12 2307(47) 2308(48) THE JAPANESE
 Table 1.Distribution and number of cases with acute upper respiratory tract infections classified according to antimicrobial agents administered Table 2. Distribution of cases which were enrolled to set
Table 1.Distribution and number of cases with acute upper respiratory tract infections classified according to antimicrobial agents administered Table 2. Distribution of cases which were enrolled to set
VOL.32 S-7 CHEMOTHERAPY Table 1 MIC of standard strains of CTRX Fig. 2 Cumulative curves of MIC S. aureus (26 strains )
 CHEMOTHERAPY OCT. 1984 Fig. I Chemical structure of CTRX VOL.32 S-7 CHEMOTHERAPY Table 1 MIC of standard strains of CTRX Fig. 2 Cumulative curves of MIC S. aureus (26 strains ) CHEMOTHERAPY Fig. 3 Cumulative
CHEMOTHERAPY OCT. 1984 Fig. I Chemical structure of CTRX VOL.32 S-7 CHEMOTHERAPY Table 1 MIC of standard strains of CTRX Fig. 2 Cumulative curves of MIC S. aureus (26 strains ) CHEMOTHERAPY Fig. 3 Cumulative
M CHEMOTHERAPY DEC ciprofloxacin(cpfx), ofloxacin(oflx) Staphylococcus aureus, Streptococcus pneumoniae Bacteroides fragi. Haemophilus influenza
 Mycoplasma pneumoniae M. pneumoniae M. pneumoniae M. pneumoniae M CHEMOTHERAPY DEC. 1993 ciprofloxacin(cpfx), ofloxacin(oflx) Staphylococcus aureus, Streptococcus pneumoniae Bacteroides fragi. Haemophilus
Mycoplasma pneumoniae M. pneumoniae M. pneumoniae M. pneumoniae M CHEMOTHERAPY DEC. 1993 ciprofloxacin(cpfx), ofloxacin(oflx) Staphylococcus aureus, Streptococcus pneumoniae Bacteroides fragi. Haemophilus
VOL. 34 S-2 CHEMOTH8RAPY 913
 VOL. 34 S-2 CHEMOTH8RAPY 913 914 CHEMOTHERAPY APR. 1986 Fig. 1 Chemical structure of T-2588 and T-2525 T- 2588 pivaloyloxymethyl (+ )- (6 R, 7 R)-7-[(Z)-2- (2-amino- 4-thiazolyl)-2-methox yiminoacetamido]-3-[(
VOL. 34 S-2 CHEMOTH8RAPY 913 914 CHEMOTHERAPY APR. 1986 Fig. 1 Chemical structure of T-2588 and T-2525 T- 2588 pivaloyloxymethyl (+ )- (6 R, 7 R)-7-[(Z)-2- (2-amino- 4-thiazolyl)-2-methox yiminoacetamido]-3-[(
 VOL.32 S-9 CHEMOTHERAPY Table 1 Minimum inhibitory concentrations of AC-1370, CPZ and CAZ Table 2 Efficacy of AC-1370 and CPZ against systemic infections in mice *Inoculum size: 106 cells/ml * 95% confidence
VOL.32 S-9 CHEMOTHERAPY Table 1 Minimum inhibitory concentrations of AC-1370, CPZ and CAZ Table 2 Efficacy of AC-1370 and CPZ against systemic infections in mice *Inoculum size: 106 cells/ml * 95% confidence
Key words: Norfloxacin (NFLX), Infectious enteritis, Double-blind method
 Key words: Norfloxacin (NFLX), Infectious enteritis, Double-blind method Fig. 1 Chemical structure Norfloxacin (NFLX) Pipemidic acid (PPA) Fig. 2 Package of test drugs Table 1 Criteria for evaluation
Key words: Norfloxacin (NFLX), Infectious enteritis, Double-blind method Fig. 1 Chemical structure Norfloxacin (NFLX) Pipemidic acid (PPA) Fig. 2 Package of test drugs Table 1 Criteria for evaluation
Fig.1 Chemical structure of BAY o 9867
 Fig.1 Chemical structure of BAY o 9867 CHEMOTHERAPY 43 Table 3 Antibacterial spectrum of gram negative bacteria Medium:Heart infusion agar (Nissui) Method:Agar dilution (Streak) CHEMOTHERAPY DEC 1985
Fig.1 Chemical structure of BAY o 9867 CHEMOTHERAPY 43 Table 3 Antibacterial spectrum of gram negative bacteria Medium:Heart infusion agar (Nissui) Method:Agar dilution (Streak) CHEMOTHERAPY DEC 1985
 VOL.30 NO.10 CHEMOTHERAPY 1123 Fig,1 Group B case 6 hepatolithiasis,e.k.66 y.0.,f.45kg Postoperative wound infection Fig.2 Group B case 15 gastric cancer,k.k.60 y.o.,m. Postoperative peritonitis Fig.3
VOL.30 NO.10 CHEMOTHERAPY 1123 Fig,1 Group B case 6 hepatolithiasis,e.k.66 y.0.,f.45kg Postoperative wound infection Fig.2 Group B case 15 gastric cancer,k.k.60 y.o.,m. Postoperative peritonitis Fig.3
CHEMOTHERAPY
 CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of Sulbactam/CPZ against standard strains MIC mg/ml Inoculum size 106 CFU/ml * Sulbactam/CPZ= 1: 1 ** Concentration of Sulbactam+ CPZ CHEMOTHERAPY
CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of Sulbactam/CPZ against standard strains MIC mg/ml Inoculum size 106 CFU/ml * Sulbactam/CPZ= 1: 1 ** Concentration of Sulbactam+ CPZ CHEMOTHERAPY
CHEMOTHERAPY
 CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of BRL 28500 against standard strains of bacteria Fig, 1 Sensitivity distribution of ABPC-resistant E. coli isolated from urinary tract Fig. 2 Sensitivity
CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of BRL 28500 against standard strains of bacteria Fig, 1 Sensitivity distribution of ABPC-resistant E. coli isolated from urinary tract Fig. 2 Sensitivity
Key words: E. coli O 157: H7, fosfomycin, verotoxin, mouse infection
 Key words: E. coli O 157: H7, fosfomycin, verotoxin, mouse infection Table 1. Bacterial cell counts in feces of mice infected with Esclwrichia coli O 157: H7 NK2 before and during oral dosing with fosfomycin
Key words: E. coli O 157: H7, fosfomycin, verotoxin, mouse infection Table 1. Bacterial cell counts in feces of mice infected with Esclwrichia coli O 157: H7 NK2 before and during oral dosing with fosfomycin
 Key words : R-plasmid, Urinary tract infection, E. coli Fig. 1. MIC distribution against E. coli isolated from urinary tract (366 strains) and isolation - frequencies of drug-resistant strains Table 1.
Key words : R-plasmid, Urinary tract infection, E. coli Fig. 1. MIC distribution against E. coli isolated from urinary tract (366 strains) and isolation - frequencies of drug-resistant strains Table 1.
Table1MIC of BAY o 9867 against standard strains
 Table1MIC of BAY o 9867 against standard strains Fig.2Cumulative and Distribution Curves of MIC (S.aureus 54 strains) 106cfu/ml Fig.3Correlogram of MIC (S.aureus 54 strains) CHEMOTHERAPY 451 Fig.4Cumulative
Table1MIC of BAY o 9867 against standard strains Fig.2Cumulative and Distribution Curves of MIC (S.aureus 54 strains) 106cfu/ml Fig.3Correlogram of MIC (S.aureus 54 strains) CHEMOTHERAPY 451 Fig.4Cumulative
 Table 1.Quality control of MICs for reference strains Table 2.Antimicrobial activity of gatifloxacin against aerobic bacteria Table 4.Antimicrobial activity of gatifloxacin and other quinolones against
Table 1.Quality control of MICs for reference strains Table 2.Antimicrobial activity of gatifloxacin against aerobic bacteria Table 4.Antimicrobial activity of gatifloxacin and other quinolones against
Key words: HAPA-B, Intravenous drip infusion, Fundamental and clinical investigation
 Key words: HAPA-B, Intravenous drip infusion, Fundamental and clinical investigation Fig. 1 Chemical structure of HAPA-B Table 1 Background of 9 patients with Ccr value Table 2 Collaborating Clinics Internal
Key words: HAPA-B, Intravenous drip infusion, Fundamental and clinical investigation Fig. 1 Chemical structure of HAPA-B Table 1 Background of 9 patients with Ccr value Table 2 Collaborating Clinics Internal
Fig. 1 Chemical structure of TE-031 Code number: TE-031 Chemical name: (-) (3R, 4S, 5S, 6R, 7R, 9R, 11R, 12R, 13S, 14R)-4-[(2, 6-dideoxy-3-C-methyl-3-
 Fig. 1 Chemical structure of TE-031 Code number: TE-031 Chemical name: (-) (3R, 4S, 5S, 6R, 7R, 9R, 11R, 12R, 13S, 14R)-4-[(2, 6-dideoxy-3-C-methyl-3-O-methyl-a-L-ribo-hexopyranosyl) oxy]-14-ethyl-12,
Fig. 1 Chemical structure of TE-031 Code number: TE-031 Chemical name: (-) (3R, 4S, 5S, 6R, 7R, 9R, 11R, 12R, 13S, 14R)-4-[(2, 6-dideoxy-3-C-methyl-3-O-methyl-a-L-ribo-hexopyranosyl) oxy]-14-ethyl-12,
Key words : candidemia, endotoxin, D-arabinitol, Candida antigen, serological examination
 Key words : candidemia, endotoxin, D-arabinitol, Candida antigen, serological examination Fig. 1 The value of fungal index and D- arabinitol/creatinine. Fungal index was mesured by Endotoxin D and Endospecy
Key words : candidemia, endotoxin, D-arabinitol, Candida antigen, serological examination Fig. 1 The value of fungal index and D- arabinitol/creatinine. Fungal index was mesured by Endotoxin D and Endospecy
 Table 1 Survival rates of infected mice given antibiotic doses producing peak serum a) S. aurcus Smith Challenge dose :7 ~10 (5% mucin) CFU/mouse. LD50: 1 ~103 (5% mucin) CFU/mouse. Table 2 Survival rates
Table 1 Survival rates of infected mice given antibiotic doses producing peak serum a) S. aurcus Smith Challenge dose :7 ~10 (5% mucin) CFU/mouse. LD50: 1 ~103 (5% mucin) CFU/mouse. Table 2 Survival rates
 Fig. 1. Structures of NM394, NAD-358 and NAD-245 Fig. 2. Typical HPLC chromatograms of NM394 in human plasma by organic solvent extraction method (a): Blank plasma (b): Plasma spiked with NM394 and internal
Fig. 1. Structures of NM394, NAD-358 and NAD-245 Fig. 2. Typical HPLC chromatograms of NM394 in human plasma by organic solvent extraction method (a): Blank plasma (b): Plasma spiked with NM394 and internal
 Fig. 1 Chemical structure of norfloxacin Table 1. Institutes attended to the study The Department of Dermatology, Defense Medical College The Department of Dermatology, School of Medicine, Teikyo University
Fig. 1 Chemical structure of norfloxacin Table 1. Institutes attended to the study The Department of Dermatology, Defense Medical College The Department of Dermatology, School of Medicine, Teikyo University
CHEMOTHERAPY Table 1 Urinary excretion of mezlocillin Fig. 4 Urinary excretion of mezlocillin Fig. 3 Blood levels of mezlocillin
 CHEMOTHERAPY Fig. 2 Urinary excretion of mezlocillin Fig. 1 Blood levels of mezlocillin CHEMOTHERAPY Table 1 Urinary excretion of mezlocillin Fig. 4 Urinary excretion of mezlocillin Fig. 3 Blood levels
CHEMOTHERAPY Fig. 2 Urinary excretion of mezlocillin Fig. 1 Blood levels of mezlocillin CHEMOTHERAPY Table 1 Urinary excretion of mezlocillin Fig. 4 Urinary excretion of mezlocillin Fig. 3 Blood levels
Fig. 1 Chemical structure Lomefloxacin(LFLX,NY-198) Pipemidic acid(ppa)
 Key words : Lomefloxacin (LFLX, NY-198), Infectious enteritis, Double blind method Fig. 1 Chemical structure Lomefloxacin(LFLX,NY-198) Pipemidic acid(ppa) Fig. 2 Package of test drugs LFLX group PPA group
Key words : Lomefloxacin (LFLX, NY-198), Infectious enteritis, Double blind method Fig. 1 Chemical structure Lomefloxacin(LFLX,NY-198) Pipemidic acid(ppa) Fig. 2 Package of test drugs LFLX group PPA group
udc-3.dvi
 49 UDC 371.279.1 3 4 753 1 2 2 1 2 47 6 2005 11 14 50 No.35, 2006 1 1.1 AO 2003 2004 2005 2005 1 1 2005 1998 1999 2002 12 11 2000 SAT ACT Law School Admission Test LSAT Medical College Admission Test MCAT
49 UDC 371.279.1 3 4 753 1 2 2 1 2 47 6 2005 11 14 50 No.35, 2006 1 1.1 AO 2003 2004 2005 2005 1 1 2005 1998 1999 2002 12 11 2000 SAT ACT Law School Admission Test LSAT Medical College Admission Test MCAT
5 3 5 7 5 3 5 2 3 7 5 2 3 7 7 2 2 2 2 3 5 7 5 7 CONTENTS 2 3 5 7 2 2 3 5 2 22 2 2 27 2 2 3 3 32
 27 KE I O UNIVERSITY L AW SCHOOL 5 3 5 7 5 3 5 2 3 7 5 2 3 7 7 2 2 2 2 3 5 7 5 7 CONTENTS 2 3 5 7 2 2 3 5 2 22 2 2 27 2 2 3 3 32 2 3 2 3 2 3 5 7 Weekly Schedule Monday Tuesday 2 3 5 Wednesday Thursday
27 KE I O UNIVERSITY L AW SCHOOL 5 3 5 7 5 3 5 2 3 7 5 2 3 7 7 2 2 2 2 3 5 7 5 7 CONTENTS 2 3 5 7 2 2 3 5 2 22 2 2 27 2 2 3 3 32 2 3 2 3 2 3 5 7 Weekly Schedule Monday Tuesday 2 3 5 Wednesday Thursday
208 ( 2 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 63 _ 3 June 2010 Cefditoren pivoxil (CDTR-PI) MS MS 10%
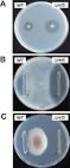 207 ( 1 ) Cefditoren pivoxil G 2010 2 2 2006 3 Cefditoren pivoxil CDTR-PI MS 10% CDTR-PI 305 2,144 2,006 1,958 1.79% 36 2,006 26 (1.30%) CDTR-PI CDTR-PI (9 mg/kg/day) 1.5 2 (2.70%) 2 (1.92%) 93.5% 1,831
207 ( 1 ) Cefditoren pivoxil G 2010 2 2 2006 3 Cefditoren pivoxil CDTR-PI MS 10% CDTR-PI 305 2,144 2,006 1,958 1.79% 36 2,006 26 (1.30%) CDTR-PI CDTR-PI (9 mg/kg/day) 1.5 2 (2.70%) 2 (1.92%) 93.5% 1,831
Feb THE JAPANESE JOURNAL OF ANTIBIOTICS Tebipenem pivoxil 1 1, Meiji Seika 2 Meiji Seika G 3 Meiji Seika Tebipen
 Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 53 53 Tebipenem pivoxil 1 1, 3 2 2 1 1 Meiji Seika 2 Meiji Seika G 3 Meiji Seika 2015 12 15 Tebipenem pivoxil 10% 2010 4 2013 3 3,547 3,540 3,540 3,331
Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 53 53 Tebipenem pivoxil 1 1, 3 2 2 1 1 Meiji Seika 2 Meiji Seika G 3 Meiji Seika 2015 12 15 Tebipenem pivoxil 10% 2010 4 2013 3 3,547 3,540 3,540 3,331
 CHEMOTHERAPY Silver sulfadiazine (T 107) CHEMOTHERAPY Fig. 1 Item of patients Table 1 Criteria of bacteriological efficacy by the Committee xcellent: E Score of infection becomes to 0% at the end of medication.
CHEMOTHERAPY Silver sulfadiazine (T 107) CHEMOTHERAPY Fig. 1 Item of patients Table 1 Criteria of bacteriological efficacy by the Committee xcellent: E Score of infection becomes to 0% at the end of medication.
CHEMOTHERAPY DEC (NFLX), ofloxacin (OFLX), ciprofloxacin (CPFX) Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, Enterococcus faecali
 CHEMOTHERAPY DEC. 1988 (NFLX), ofloxacin (OFLX), ciprofloxacin (CPFX) Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, Enterococcus faecalis Pseudomonas aeruginosa, Serratia ma- Fig. 1. Chemical
CHEMOTHERAPY DEC. 1988 (NFLX), ofloxacin (OFLX), ciprofloxacin (CPFX) Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, Enterococcus faecalis Pseudomonas aeruginosa, Serratia ma- Fig. 1. Chemical
Clostridium difficile ciprofloxacin, ofloxacin, norfloxacin Bifidobacterium Lactobacillus Lactobacillus Bacteroides fragilis B. fragilis C. difficile
 Clostridium difficile ciprofloxacin, ofloxacin, norfloxacin Bifidobacterium Lactobacillus Lactobacillus Bacteroides fragilis B. fragilis C. difficile Key words: temafloxacin, TA-167, Bacteroides fragilis,
Clostridium difficile ciprofloxacin, ofloxacin, norfloxacin Bifidobacterium Lactobacillus Lactobacillus Bacteroides fragilis B. fragilis C. difficile Key words: temafloxacin, TA-167, Bacteroides fragilis,
VOL. 23 NO. 3 CHEMOTHERAPY 1379 Table 1 Susceptibility of clinical isolated strains to Tobramycin
 VOL. 23 NO. 3 CHEMOTHERAPY 1379 Table 1 Susceptibility of clinical isolated strains to Tobramycin 1380 CHEMOTHERAPY MAR. 1975 Table 2 Susceptibility of isolated Pseudomonas aeruginosa to various antibiotics
VOL. 23 NO. 3 CHEMOTHERAPY 1379 Table 1 Susceptibility of clinical isolated strains to Tobramycin 1380 CHEMOTHERAPY MAR. 1975 Table 2 Susceptibility of isolated Pseudomonas aeruginosa to various antibiotics
<95DB8C9288E397C389C88A E696E6462>
 2011 Vol.60 No.4 p.332 338 Usefulness of regional education program for dietary salt reduction: Self-monitoring of urinary salt excretion Kenichiro YASUTAKE[1] Kayoko SAWANO[1] Shoko YAMAGUCHI[1] Hiroko
2011 Vol.60 No.4 p.332 338 Usefulness of regional education program for dietary salt reduction: Self-monitoring of urinary salt excretion Kenichiro YASUTAKE[1] Kayoko SAWANO[1] Shoko YAMAGUCHI[1] Hiroko
 Fig.1 MICs of penicillins against 24 strains of B. pertussis Fig.2 MICs of cepherns against 24 strains of B. pertussis Fig.3 MICs of macrolides against 24 strains of B. pertussis Fig.4 MICs of nalidixic
Fig.1 MICs of penicillins against 24 strains of B. pertussis Fig.2 MICs of cepherns against 24 strains of B. pertussis Fig.3 MICs of macrolides against 24 strains of B. pertussis Fig.4 MICs of nalidixic
CHEMOTHERAPY APR Fig. 2 The inactivation of aminoglycoside antibiotics by PC-904 Fig. 3 Serum concentration of PC-904 (1) Fig. 4 Urinary recover
 VOL.26 S-2 CHEMOTHERAPY Gentamicin (GM), Dibekacin (DKB), Tobramycin Fig. 1 Protein concentration and protein binding rate Table 2 Protein binding rate of PC-904 in serum of healthy adults, and patients
VOL.26 S-2 CHEMOTHERAPY Gentamicin (GM), Dibekacin (DKB), Tobramycin Fig. 1 Protein concentration and protein binding rate Table 2 Protein binding rate of PC-904 in serum of healthy adults, and patients
CHEMOTHERAPY NOV S. aureus, S. epidermidis, E. coli, K. pgeumoniae, E. cloacae, S. marcescens, P. mirabilis, Proteus, P. aeruginosa Inoculum siz
 VOL.33 S-5 CHEMOTHERAPY 381 Fig. 1 Chemical structure of HAPA-B Chemical name 1-N-[(2S)-3-Amino-2-hydroxypropiony1]-4-0-(6-amino- 6-deoxy-a-D-glucopyranosyl)-6-013-deoxy-4-C-methyl- 3-(methylamino)-ƒÀ-L-arabinopyranosyl]-2-deoxystreptamine
VOL.33 S-5 CHEMOTHERAPY 381 Fig. 1 Chemical structure of HAPA-B Chemical name 1-N-[(2S)-3-Amino-2-hydroxypropiony1]-4-0-(6-amino- 6-deoxy-a-D-glucopyranosyl)-6-013-deoxy-4-C-methyl- 3-(methylamino)-ƒÀ-L-arabinopyranosyl]-2-deoxystreptamine
 Table 1-1. Criteria for evaluation Table 2. Criteria for bacteriological efficacy Table 1-2. Criteria for evaluation Table 3. Reasons for exclusion and drop-out from evaluation (clinical efficacy) Table
Table 1-1. Criteria for evaluation Table 2. Criteria for bacteriological efficacy Table 1-2. Criteria for evaluation Table 3. Reasons for exclusion and drop-out from evaluation (clinical efficacy) Table
VOL.39 S-3
 VOL.39 S-3 CHEMOTHERAPY SEPT.1991 Table 1. Background of characteristics and allocation of 5 healthy male volunteers in a multiple-dose study on panipenem/betamipron Day 1 Fig. 1. Schedule of multiple-dose
VOL.39 S-3 CHEMOTHERAPY SEPT.1991 Table 1. Background of characteristics and allocation of 5 healthy male volunteers in a multiple-dose study on panipenem/betamipron Day 1 Fig. 1. Schedule of multiple-dose
 b) Gram-negative bacteria Fig. 2 Sensitivity distribution of clinical isolates : E. coli Fig. 3 Sensitivity distribution of clinical isolates : Pseudomonas Fig. 1 Sensitivity distribution of clinical isolates
b) Gram-negative bacteria Fig. 2 Sensitivity distribution of clinical isolates : E. coli Fig. 3 Sensitivity distribution of clinical isolates : Pseudomonas Fig. 1 Sensitivity distribution of clinical isolates
Key words: Respiratory Tract Infection, Ceftazidime, Cefotiam, Double-blind Method
 Key words: Respiratory Tract Infection, Ceftazidime, Cefotiam, Double-blind Method Fig. 1 Chemical structure of CAZ Table 1 Result of assay on CAZ and CTM samples Table 2 Laboratory examination Table
Key words: Respiratory Tract Infection, Ceftazidime, Cefotiam, Double-blind Method Fig. 1 Chemical structure of CAZ Table 1 Result of assay on CAZ and CTM samples Table 2 Laboratory examination Table
 The clinical characteristics of Mycoplasma pneumoniae pneumonia in children younger than 6 years old Nobue Takeda1,2),Tomomichi Kurosaki1),Naruhiko Ishiwada2),Yoichi Kohno2) 1)Department of Pediatrics,Chiba
The clinical characteristics of Mycoplasma pneumoniae pneumonia in children younger than 6 years old Nobue Takeda1,2),Tomomichi Kurosaki1),Naruhiko Ishiwada2),Yoichi Kohno2) 1)Department of Pediatrics,Chiba
Fig. 1 Trends of TB incidence rates for all forms and smear-positive pulmonary TB in Kawasaki City and Japan. Incidence=newly notified cases of all fo
 Kekkaku Vol. 79, No. 1: 17-24, 2004 17 (Received 21 Aug. 2003/Accepted 18 Nov. 2003) Fig. 1 Trends of TB incidence rates for all forms and smear-positive pulmonary TB in Kawasaki City and Japan. Incidence=newly
Kekkaku Vol. 79, No. 1: 17-24, 2004 17 (Received 21 Aug. 2003/Accepted 18 Nov. 2003) Fig. 1 Trends of TB incidence rates for all forms and smear-positive pulmonary TB in Kawasaki City and Japan. Incidence=newly
 Table 1 Patients with various renal function * Ccr, Creatinine clearance ml/min per 1. 48 m2 ** C.V.D., Cerebral vascular disease ; C.R F., Chronic renal failure ; H.D., Hemoclialysis ; D., Dialyzer ;
Table 1 Patients with various renal function * Ccr, Creatinine clearance ml/min per 1. 48 m2 ** C.V.D., Cerebral vascular disease ; C.R F., Chronic renal failure ; H.D., Hemoclialysis ; D., Dialyzer ;
 CHEMOTHERAPY AUG. 1982 VOL. 30 NO. 8 CHEMOTHERAPY Fig.1 Relation between various-closis of cefazolin and detection rate of organisms in heart blood of dying mice with E. coli and P. aeruginosa infection
CHEMOTHERAPY AUG. 1982 VOL. 30 NO. 8 CHEMOTHERAPY Fig.1 Relation between various-closis of cefazolin and detection rate of organisms in heart blood of dying mice with E. coli and P. aeruginosa infection
THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterococcus avium 5Š, Corynebacterium xerosis 10Š, Corynebacterium pseudodiphtheriticum 10Š, Corynebacterium
 THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterobacter spp., Serratia spp., Burkholderia cepacia, Flavobacterium spp., Alcaligenes spp. THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterococcus avium 5Š, Corynebacterium
THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterobacter spp., Serratia spp., Burkholderia cepacia, Flavobacterium spp., Alcaligenes spp. THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterococcus avium 5Š, Corynebacterium
988 CHEMOTHERAPY NOV. 1971
 988 CHEMOTHERAPY NOV. 1971 VOL. 19 NO. 8 CHEMOTHERAPY 989 Effect of medium-ph and inoculum size on activity of SB-PC heart infusion agar, mcg/ml Sensitivity distribution of Staphylococci to SB-PC in surgical
988 CHEMOTHERAPY NOV. 1971 VOL. 19 NO. 8 CHEMOTHERAPY 989 Effect of medium-ph and inoculum size on activity of SB-PC heart infusion agar, mcg/ml Sensitivity distribution of Staphylococci to SB-PC in surgical
 Table 1. Serum and tissue levels after a single oral administrsion of gatiflozacin ND: not detected(0. 05 ug/g or 0. 05 ug/eml) Table 2. Reason for exclusion and dropped out from evaluation VOL.47 NO.10
Table 1. Serum and tissue levels after a single oral administrsion of gatiflozacin ND: not detected(0. 05 ug/g or 0. 05 ug/eml) Table 2. Reason for exclusion and dropped out from evaluation VOL.47 NO.10
VOL. 21 NO. 2 CHEMOTHERAPY 395
 394 CHEMOTHERAPY MAR. 1973 VOL. 21 NO. 2 CHEMOTHERAPY 395 396 CHEMOTHERAPY MAR. 1973 VOL. 21 NO. 2 CHEMOTHERAPY 397 398 CHEMOTHERAPY MAR. 1973 VOL. 2 1 NO. 2 CHEMOTHERAPY 399 400 CHEMOTHERAPY MAR. 1973
394 CHEMOTHERAPY MAR. 1973 VOL. 21 NO. 2 CHEMOTHERAPY 395 396 CHEMOTHERAPY MAR. 1973 VOL. 21 NO. 2 CHEMOTHERAPY 397 398 CHEMOTHERAPY MAR. 1973 VOL. 2 1 NO. 2 CHEMOTHERAPY 399 400 CHEMOTHERAPY MAR. 1973
 Key words: atypical pulmonary mycobacteriosis, Mycobacterium avium complex, bronchial washing, transbronchial lung biopsy Table 1 Background data of 14 patients Old pul. tbc: sclerosing pulmonary tuberculosis
Key words: atypical pulmonary mycobacteriosis, Mycobacterium avium complex, bronchial washing, transbronchial lung biopsy Table 1 Background data of 14 patients Old pul. tbc: sclerosing pulmonary tuberculosis
 Osamu NEMOTO, M.D. Clinical and Bacteriological Research of Sucrose/ Povidone-Iodine Ointment (U-PASTA kowa) for Pressure Sores and Skin Ulcers Osamu Nemoto Department of Dermatology,Tonan Hosptal
Osamu NEMOTO, M.D. Clinical and Bacteriological Research of Sucrose/ Povidone-Iodine Ointment (U-PASTA kowa) for Pressure Sores and Skin Ulcers Osamu Nemoto Department of Dermatology,Tonan Hosptal
CHEMOTHERAPY OCT Fig. 1 Chemical structure of CVA-K
 OCT. 1986 Fig. 1 Chemical structure of CVA-K VOL.34 S-4 heart infusion broth (Difco) 37.0 g, Resazurin 0.1% alcoholic solution (Wako) 1.0 ml, L-Cystein-HCl H2O (Wako) 0.5 g, Bact agar (Difco) 1.0 g, Deionized
OCT. 1986 Fig. 1 Chemical structure of CVA-K VOL.34 S-4 heart infusion broth (Difco) 37.0 g, Resazurin 0.1% alcoholic solution (Wako) 1.0 ml, L-Cystein-HCl H2O (Wako) 0.5 g, Bact agar (Difco) 1.0 g, Deionized
