2 2 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb Neisseria gonorrhoeae ceftriaxone CTRX % 2010 CTRX 20 FQ staphylococci, E. faecium, N.
|
|
|
- しょうこ かみこ
- 5 years ago
- Views:
Transcription
1 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS , ,762 FQ 33 Streptococcus pyogenes, Streptococcus pneumoniae, Moraxella catarrhalis, Haemophilus influenzae FQ S. pneumoniae 8 H. influenzae 2002 β- H. influenzae %, %, %, %, % FQ Escherichia coli MIC 4 μg/ml levofloxacin 34.4% Klebsiella pneumoniae E. coli FQ Staphylococcus aureus MRSA FQ sitafloxacin 55.3% FQ %S. aureus FQ % Enterococcus faecium FQ % Pseudomonas aeruginosa FQ % % 80% FQ P. aeruginosa % Acinetobacter spp. FQ Imipenem 2.7% 14 Acinetobacter 0.2% 1
2 2 2 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb Neisseria gonorrhoeae ceftriaxone CTRX % 2010 CTRX 20 FQ staphylococci, E. faecium, N. gonorrhoeae, E. coli 30% % ciprofloxacin 80% FQ 80% β- Extended-spectrum β-lactamase: ESBL Escherichia coli, Klebsiella pneumoniae 1 β- Metallo-β-lactamase MBL 2 Carbapenem-resistant Enterobacteriaceae CRE Multiple drug-resistant Acinetobacter : MDRA FQ FQ 4 7 FQ Escherichia coli 2000 FQ FQ ESBL ,762 Quinolone resistance determining region QRDR β ,762 Table 1 Table levofloxacin LVFX ciprofloxacin CPFX tosufloxacin TFLX sitafloxacin STFX pazufloxacin PZFX nalidixic
3 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS Table 1. List of the levofloxacin surveillance group acid NA benzylpenicillin PCG ampicillin gentamicin GM amikacin AMK linezolid ABPC clavulanic acid/amoxicillin CVA/AMPC LZD daptomycin DAP piperacillin PIPC tazobactam/piperacillin TAZ/ PIPC oxacillin MPIPC cefaclor CCL cefotiam 3. CTM cefdinir CFDN cefpodoxime CPDX ceftazidime CAZ cefotaxime CTX ceftriaxone CTRX cefpirome CPR meropenem MEPM panipenem PAPM imipenem IPM aztreonam MIC Neisseria gonorrhoeae AZT minocycline MINO clarithromycin MIC CAM azithromycin AZM vancomycin Table 3 VCM sulfamethoxazole/trimethoprim ST
4 4 4 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb Table 2. The number of isolates Clinical and Laboratory Standards Institute CLSI M100-S24 8 CLSI European Committee on Antimicrobial Susceptibility Testing EUCAST 9 Staphylococcus aureus MIC S. aureus MSSA MPIPC MIC 2 μg/ml S. aureus MRSA MPIPC MIC 4 μg/ ml staphylococci MIC staphylococci MSCNS MPIPC MIC 0.25 μg/ml staphylococci MRCNS MPIPC MIC 0.5 μg/ml Streptococcus pneumoniae S. pneumoniae PSSP PCG MIC 0.06 μg/ml PISP PCG MIC μg/ml S. pneumoniae PRSP PCG MIC 2 μg/ml 4. Haemophilus influenzae β- H. influenzae 10 β-
5 Table 3. Test drugs and the range of their concentrations for determination of MIC Feb THE JAPANESE JOURNAL OF ANTIBIOTICS
6 6 6 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb QRDR S. pneumoniae, Streptococcus pyogenes, H. influenzae, E. coli, K. pneumoniae QRDR 11 S. pneumoniae gyra Ser81, Glu85 gyrb Asp435, Glu474 parc Ser79, Asp83 pare Asp435, Glu474 S. pyogenes gyra Ser81, Glu85 parc Ser79, Asp83 H. influenzae gyra Ser84, Asp88 parc Ser84, Glu88 E. coli gyra Ser83, Asp87 parc Ser80, Glu84 K. pneumoniae gyra Ser83, Asp87 parc Ser80 LVFX MIC 20% 20 MIC 20 LVFX MIC 10 MIC ESBL E. coli, K. pneumoniae, Proteus mirabilis CTX CVA, CAZ CVA MIC CTX, CAZ MIC 8 ESBL PCR CTX-M 7. -β- Metallo-β-lactamase MBL CAZ IPM Acinetobacter spp. Pseudomonas aeruginosa SMA MBL PCR IMP-1 IMP-2 VIM-1 VIM-2 8. P. aeruginosa, Acinetobacter spp. P. aeruginosa Acinetobacter spp. MIC CPFX 4 μg/ml, IPM 16 μg/ml, AMK 32 μg/ml P. aeruginosa MDRP multi-drug resistant P. aeruginosa Acinetobacter spp. MDRA multi-drug resistant Acinetobacter spp Table 4 1 S. aureus MSSA 725 MSSA FQ MIC μg/ ml % FQ STFX FQ ABPC 48.8%, CPDX 53.4%, CAM AZM 74.3%, 72.3%, PIPC 89.9% % 2 S. aureus MRSA 665 MRSA FQ MIC μg/ml STFX 55.3% FQ % FQ VCM, LZD, DAP 100% % MRSA Community-acquired MRSA CA-MRSA LVFX 1 μg/ml MINO 4 μg/ml CAM 2 μg/
7 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS Table 4. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of Clinical and Laboratory Standards Institute
8 8 8 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb Table 4. Continued
9 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS Table 4. Continued ml 9.3% 62/665 3 staphylococci MSCNS 516 MSCNS FQ MIC μg/ml % FQ CAM, AZM 76.7%, 75.2% % 4 staphylococci MRCNS 677 MRCNS MIC 90 MRSA FQ STFX MIC 90 1 μg/ml 93.5% FQ MIC μg/ml % VCM, LZD DAP 100% 5 S. pneumoniae 599 S. pneumoniae FQ MIC μg/ml CPFX 74.3%, PZFX 89.6% FQ % STFX MIC μg/ml 100% FQ VCM, CVA/AMPC, PAPM, CTRX 100%, 98.2%, 98.2%, 97.2% % CAM,
10 10 10 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb AZM 80% S. pneumoniae 599 PSSP, PISP, PRSP % % % PSSP FQ LVFX 98.8%, CPFX 74.5%, TFLX 99.1%, STFX 100%, PZFX 88.1% PRSP LVFX 88.2%, CPFX 41.2%, TFLX 94.1%, STFX 100%, PZFX 76.5% FQ PSSP PRSP CPFX, PZFX STFX PSSP, PRSP 100% 6 S. pyogenes 384 S. pyogenes FQ MIC μg/ml PZFX, CPFX 72.4%, 78.9% % FQ CAM 64.6%, AZM 63.5%, MINO 87.2% 100% 7 Enterococcus faecalis 629 E. faecalis FQ % FQ MPIPC, CCL, CTM, MINO, CAM, AZM % % ABPC, CVA/AMPC, VCM, DAP 8 Enterococcus faecium 511 E. faecium FQ % FQ VCM 100%, LZD 99.4%, DAP 99.4% % Table 5. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of Clinical and Laboratory Standards Institute
11 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS Table 5 1 Moraxella catarrhalis 504 M. catarrhalis FQ MIC μg/ml 100% FQ ABPC 14.1% % CVA/AMPC ABPC β- 2 N. gonorrhoeae 58 N. gonorrhoeae FQ MIC 90 LVFX, CPFX, TFLX μg/ml 25.9% STFX MIC μg/ml FQ ABPC CVA/AMPC 1.7%, 0% CTRX 1 MIC 1 μg/ml, 1.7% MIC LVFX 1 μg/ml, CVA/AMPC 2 μg/ml, AZM 0.5 μg/ml, MINO 1 μg/ml 3 Table 6 1 E. coli 712 E. coli FQ MIC 90 STFX μg/ml % STFX MIC 90 2 μg/ml FQ FQ % IPM, PAPM 2 Klebsiella spp. 662 Klebsiella spp. FQ MIC μg/ml % E. coli 30% FQ ABPC 6.3%, ST 32.2% % 3 Citrobacter spp. 543 Citrobacter spp. FQ MIC μg/ml % FQ ABPC 12.9% % IPM, PAPM, GM, AMK 97% 4 Enterobacter spp. 628 Enterobacter spp. FQ MIC μg/ml % FQ ABPC, CVA/AMPC, CCL, CTM, CFDN, CPDX, ST % % PAPM, MINO, GM, AMK 90% 5 P. mirabilis 512 P. mirabilis FQ MIC μg/ml % FQ MINO 1.6% % TAZ/PIPC 6 Proteus spp. 417 Proteus spp. FQ MIC μg/ml % FQ 90% NA, PIPC, TAZ/PIPC, CAZ, CTX, GM, AMK 7 Serratia spp. 590 Serratia spp. FQ MIC μg/ml % FQ ABPC 3.7%, CVA/AMPC 2.9%, CCL 0.5%, CTM 0.8%, CFDN 3.6, ST 3.7% CAZ, PAPM, GM, AMK 99% AMK
12 12 12 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb Table 6. In vitro activities of drugs against clinical isolates and percentages of isolates susceptible to test drugs on the basis of Clinical and Laboratory Standards Institute 8 Salmonella spp. 123 Salmonella spp. FQ MIC μg/ml % FQ ST 73.2%, ABPC 82.9%, PIPC 83.7, MINO 87.0% 90%
13 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS Table 6. Continued 9 H. influenzae 620 H. influenzae FQ MIC μg/ml % LVFX MIC 8 μg/ml 1 STFX MIC 0.5 μg/ml β- BLNAR,
14 14 14 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb Table 6. Continued ABPC MIC 2 μg/ml % % CFDN MIC 2 μg/ml β- BLPAR, ABPC MIC 2 μg/ ml % % CVA/AMPC MIC 8 μg/ml 10 Acinetobacter spp. 512 Acinetobacter spp. FQ MIC 90
15 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS Table 6. Continued μg/ml % FQ CCL, CTM, CFDN, CPDX, ST, ABPC % TAZ/PIPC, PAPM, IPM, MINO, GM, AMK 90% IPM % 9 Acinetobacter baumannii MDRA 0.2% 1/ P. aeruginosa 1,175 P. aeruginosa FQ MIC μg/ml 1 4 μg/ml MIC % % FQ
16 16 16 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb CTX PAPM 20% 70% CAZ, GM, AMK 90% MDRP 1.6% 9/559 MDRP 2. QRDR S. pneumoniae, S. pyogenes, H. influenzae, E. coli, K. pneumoniae QRDR Table 7 1 S. pneumoniae LVFX MIC 8 μg/ml % QRDR 3 GyrA ParC GyrB ParC LVFX MIC 4 μg/ ml 3 MIC 1 μg/ml, MIC 2 μg/ml % % GyrA ParC, GyrB ParC, GyrA ParE 2 S. pyogenes LVFX MIC 4 μg/ml LVFX MIC 8 μg/ml 15 QRDR 12 GyrA ParC LVFX MIC 2 μg/ml MIC 2 μg/ml, MIC 1 μg/ml % % ParC 1 GyrA ParC MIC 0.5 μg/ml QRDR 3 H. influenzae LVFX MIC 4 μg/ml 1 MIC 8.0 μg/ml 1 GyrA ParC LVFX MIC 2 μg/ml MIC 0.03 μg/ml μg/ml GyrA 0.5 μg/ml, 2 μg/ml GyrA ParC 4 E. coli LVFX MIC 4 μg/ml MIC 8 μg/ml 50 GyrA ParC LVFX MIC 2 μg/ml μg/ml % 0.5 μg/ml 1 1 μg/ml 4 2 μg/ml 3 GyrA ParC 0.06 μg/ml 5 K. pneumoniae LVFX MIC 8 μg/ml % QRDR 12 GyrA ParC LVFX MIC 4 μg/ml % GyrA 1 GyrA ParC 1 LVFX MIC 2 μg/ml % GyrA 1 3. ESBL ESBL E. coli 17.8%
17 Table 7. MICs and types of substitutions identified in genes containing quinolone resistance determining regions Feb THE JAPANESE JOURNAL OF ANTIBIOTICS
18 18 18 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb Table 8. Detection rates of extended-spectrum β-lactamase producing strains Table 9. Detection rates of metallo-β-lactamase producing strains 127/712 K. pneumoniae 6.7% 37/552 P. mirabilis 10.9% 56/ ESBL Table 8 ESBL E. coli % 17.8%, K. pneumoniae 2.1% 6.7% P. mirabilis ESBL 4. MBL MBL Acinetobacter spp. 1.0% 5/512 IMP-1 4 IMP-2 1 P. aeruginosa MBL 1.8% 10/559 IMP MDRP P. aeruginosa MBL Acinetobacter spp P. aeruginosa MBL Table 9 Acinetobacter spp., P. aeruginosa MBL 0 2% P. aeruginosa MBL % % , FQ FQ 1994 LVFX,
19 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS CPFX, TFLX FQ STFX FQ PZFX 5 FQ MSSA FQ % MRSA FQ STFX 55.3% FQ % MRSA VCM, LZD, DAP MSSA VCM, DAP 3 VCM MIC 4 μg/ml 1 DAP MIC 2 μg/ml 1990 CA-MRSA CA-MRSA LVFX 1 μg/ml MINO 4 μg/ml CAM 2 μg/ml % %, % % 47/62 CA-MRSA USA300 12,13 VCM MRSA MIC 2 μg/ml % 8.9% % VCM MIC 2 μg/ml S. pneumoniae FQ CPFX 74.3%, PZFX 89.6% % LVFX MIC 2 μg/ml MIC 1 μg/ml % % FQ DNA IV QRDR 2 14 LVFX MIC 1 μg/ml MIC 2 μg/ ml 20 3 GyrA, GyrB, ParC, ParE MIC 1 μg/ml 2 MIC 2 μg/ml 1 QRDR S. pyogenes FQ PZFX, CPFX 72.4%, 78.9% % LVFX %, % % QRDR LVFX MIC 4 μg/ml GyrA ParC LVFX MIC 1 μg/ml 2 μg/ml ParC QRDR FQ E. coli 2000 FQ 4 7 E. coli FQ % 4 7 E. coli LVFX %, %,
20 20 20 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb %, %, %, %, % % % LVFX 61.6% 76.3% 66.0% 77.2% 15 K. pneumoniae FQ E. coli QRDR E. coli LVFX MIC 2 μg/ml % GyrA ParC K. pneumoniae LVFX % GyrA E. coli, K. pneumoniae, P. mirabilis ESBL 17.8% 127/ % 37/ % 56/512 E. coli % 17.8% ESBL ESBL 16 ESBL LVFX E. coli ESBL 81.1%, ESBL 21.1% χ 2 P K. pneumoniae ESBL 21.6%, ESBL 1.9% χ 2 P P. mirabilis ESBL 48.2%, ESBL 3.3% χ 2 P ESBL LVFXK. pneumoniae, P. mirabilis FQ E. coli FQ ESBL FQ H. influenzae FQ % QRDR LVFX μg/ml GyrA QRDR 0.5 μg/ml, 2 μg/ml, 8 μg/ml GyrA ParC QRDR FQ 17 FQ BLNAR BLNAR % 57.9% % Salmonella spp. CLSI 2012 FQ LVFX S 2 μg/ml 0.12 μg/ml FQ NA FQ NA LVFX LVFX NA LVFX NA 8.1% 10/ % 2/123 P. aeruginosa FQ % % 80% LVFX % %, % FQ
21 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS FQ MDRP MDRP 1.6% 9/559 MDRP MDRP Acinetobacter spp. IPM 96.9%, PAPM 94.5% IPM 14 6 MDRA % N. gonorrhoeae CTRX CTRX % 1 1.7% 20 LVFX FQ MRCNS, MRSA, E. faecium, E. coli, N. gonorrhoeae 30% CPFX 80% FQ 80% JA JA NTT
22 22 22 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb. 2016
23 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS FOUQUET, M.; V. MORANGE & F. BRUYÈRE: Five years following of infections with extended-spectrum beta-lactamase producing enterobacteriaceae. Prog. Urol. 22: 17 21, HIRAKATA, Y.; K. IZUMIKAWA, T. YAMAGUCHI, et al.: Rapid detection and evoluation of clinical characteristics of emerging multiple-drugresistant Gram-negative rods carrying the metallo-β-lactamase gene bla IMP. Antimicrob. Agents Chemother. 42: , , YAMAGUCHI, K.; A. OHNO & Levofloxacin surveillance group: Investigation of the susceptibility trends in Japan to fluoroquinolones and other antimicrobial agents in a nationwide collection of clinical isolates: a longitudinal analysis from 1994 to Diagn. Microbiol. Infect. Dis. 52: , ,639 Jpn. J. Antibiotics 59: , ,919 Jpn. J. Antibiotics 62: , ,866 Jpn. J. Antibiotics 65: , Clinical and Laboratory Standards Institute: Performance standards for antimicrobial susceptibility testing; Twenty-fourth informational Supplement M100-S24, European Committee on Antimicrobial Susceptibility Testing; Breakpoint tables for interpretation of MICs and zone diameters Version4.0, β- 13: 73 83, GERISCHER, U.: Direct sequencing of DNA produced in a polymerase chain reaction. Meth. Mol. Biol. 167: 53 61, MINE, Y.; I. NAKASONE, Y. YAMAMOTO, et al.: Dissemination of Panton-Valentine leukocidinpositive methicillin-resistant Staphylococcus aureus in Okinawa. J. Dermatol. 40: 34 38, MINE, Y.; W. HIGUCHI, K. TAIRA, et al.: Nosocomial outbreak of multidrug-resistant USA300 methicillin-resistant Staphylococcus aureus causing severe furuncles and carbuncles in Japan. J. Dermatol. 38: , WEIGEL, L. M.; G. J. ANDERSON, R. R. FACKLAM, et al.: Genetic analyses of mutations contributing to fluoroquinolone resistance in clinical isolates of Streptococcus pneumoniae. Antimicrob. Agents Chemother. 45: , REINERT, R. R.; D. E. LOW, F. ROSSI, et al.: Antimicrobial susceptibility among organisms from the Asia/Pacific Rim, Europe and Latin and North America collected as part of TEST and the in vitro activity of tigecycline. J. Antimicrob. Chemother. 60: , KOMATSU, M.; M. AIHARA, K. SHIMAKAWA, et al.: Evaluation of MicroScan ESBL confirmation panel for Enterobacteriaceae-producing, extended-spectrum beta-lactamases isolated in Japan. Diagn. Microbiol. Infect. Dis. 46: , KIM, I. S.; N. Y. LEE, S. KIM, et al.: Reduced levofloxacin susceptibility in clinical respiratory isolates of Haemophilus influenzae is not yet associated with mutations in the DNA gyrase and topoisomerase II genes in Korea. Yonsei Med. J. 52: , 2011
24 24 24 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 Feb Surveillance of in vitro susceptibilities to levofloxacin and various antibacterial agents for 11,762 clinical isolates obtained from 69 centers in 2013 KEIZO YAMAGUCHI Department of Microbiology and Infectious Diseases, Department of Advanced and Integrated Analysis of Infectious Diseases, Toho University School of Medicine KAZUHIRO TATEDA, AKIRA OHNO and YOSHIKAZU ISHII Department of Microbiology and Infectious Diseases, Toho University School of Medicine HINAKO MURAKAMI Department of Clinical Laboratory, Toho University Omori Medical Center Antimicrobial susceptibility testing has been conducted continuously as postmarketing surveillance of levofloxacin LVFX since The present survey was undertaken to investigate in vitro susceptibilities of bacteria to 33 selected antibacterial agents, focusing on fluoroquinolones FQs, using 11,762 clinical isolates for 19 species collected from 69 centers during 2013 in Japan. The common respiratory pathogens Streptococcus pyogenes, Streptococcus pneumoniae, Moraxella catarrhalis, and Haemophilus influenzae continue to show a high susceptibility to FQs, while the percentage of macrolide-resistant S. pneumoniae was markedly increased to around 80%. With H. influenzae, the percentage of β-lactamase-negative ampicillinresistant isolates had been increasing continuously from 2002, but no increase was observed from 2010 to % in 2002, 40.0% in 2004, 50.1% in 2007, 57.9% in 2010, and 57.1% in Most strains of Enterobacteriaceae showed a high susceptibility to FQs, but the isolation frequency of levofloxacin-resistant Escherichia coli including intermediate resistance was 34.4%, showing a continuous increase. Another Enterobacteriaceae member, Klebsiella pneumoniae, showed low resistance to FQs in contrast with E. coli. Regarding methicillin-resistant Staphylococcus aureus MRSA, the percentage of FQ-susceptible isolates was low at %, with the exception of 55.3% susceptibility to sitafloxacin. On the other hand, methicillinsusceptible S. aureus MSSA isolates showed high susceptibility to FQs, at %. With Enterococcus faecium, the percentage of FQ-susceptible isolates was %. The percentage of FQ-susceptible Pseudomonas aeruginosa was % among isolates derived from urinary tract infections UTIs, while that from respiratory tract infections RTIs was %. This was summarized as susceptibility to FQs over 80% in both infections. A continuous decrease in FQ-resistant P. aeruginosa was noted, especially among isolates from UTIs. Regarding multidrug-resistant P. aeruginosa, the percentage has been decreasing continuously
25 Feb THE JAPANESE JOURNAL OF ANTIBIOTICS since 2007 and was 1.6% from UTIs and 0% from RTI in this survey. Acinetobacter spp. showed high susceptibility to FQs. The percentage of imipenem-resistant Acinetobacter spp. was 2.7% 14 isolates and that of multidrug-resistant was 0.2% 1 isolate. In Neisseria gonorrhoeae, ceftriaxone CTRX had been showing 100% susceptibility until 2007, but CTRX-resistant strains have been detected in both 2010 and this survey. In conclusion, the resistance of methicillin-resistant staphylococci, E. faecium, N. gonorrhoeae, and E. coli to the FQs, which have been used clinically for over 20 years, was shown to be 30% or more % in the present surveillance regarding susceptibility. These results were similar to those from previous surveillance, and no species that started to show significant resistance to FQs were identified in the present surveillance. Regarding other bacterial species, susceptibility to ciprofloxacin less than 80% was observed in some, while susceptibility to other FQs was maintained at a high level, at 80% or more.
日本化学療法学会雑誌第61巻第6号
 β Moraxella catarrhalis Escherichia coli Citrobacter Klebsiella pneumoniae Enterobacter cloacae Serratia marcescens Proteus Pseudomonas aeruginosa Acinetobacter Bacteroides fragilis β Haemophilus influenzae
β Moraxella catarrhalis Escherichia coli Citrobacter Klebsiella pneumoniae Enterobacter cloacae Serratia marcescens Proteus Pseudomonas aeruginosa Acinetobacter Bacteroides fragilis β Haemophilus influenzae
日本化学療法学会雑誌第64巻第4号
 β β Moraxella catarrhalisescherichia colicitrobacter Klebsiella pneumoniaeenterobacter cloacaeserratia marcescens Proteus Providencia Pseudomonas aeruginosaacinetobacter Bacteroides fragilis β β E. colik.
β β Moraxella catarrhalisescherichia colicitrobacter Klebsiella pneumoniaeenterobacter cloacaeserratia marcescens Proteus Providencia Pseudomonas aeruginosaacinetobacter Bacteroides fragilis β β E. colik.
Table 1. Antimicrobial drugs using for MIC
 Table 1. Antimicrobial drugs using for MIC Table 2. Susceptibilities determined with the VITEK 2 system and agar dilution reference by interpretive eategory for Staphylococcus aureus Table 3. Interpretive
Table 1. Antimicrobial drugs using for MIC Table 2. Susceptibilities determined with the VITEK 2 system and agar dilution reference by interpretive eategory for Staphylococcus aureus Table 3. Interpretive
THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 June 2012 NTT
 June 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 181 27 201072 12,866 JA 182 28 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 June 2012 NTT June 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 183 29 2012 3
June 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 181 27 201072 12,866 JA 182 28 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 June 2012 NTT June 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 3 183 29 2012 3
CHEMOTHERAPY aureus 0.10, Enterococcus faecalis 3.13, Escherichia coli 0.20, Klebsiella pneumoniae, Enterobacter spp., Serratia marcescens 0.78, Prote
 aureus 0.10, Enterococcus faecalis 3.13, Escherichia coli 0.20, Klebsiella pneumoniae, Enterobacter spp., Serratia marcescens 0.78, Proteus mirabilis 3.13, Proteus vulgaris 1.56, Citrobacter freundii 0.39,
aureus 0.10, Enterococcus faecalis 3.13, Escherichia coli 0.20, Klebsiella pneumoniae, Enterobacter spp., Serratia marcescens 0.78, Proteus mirabilis 3.13, Proteus vulgaris 1.56, Citrobacter freundii 0.39,
Staphylococcus epidermidis Streptococcus pneumoniae Staphylococcus epidermidis Streptococcus pneumontae S. epidermidis Table 1. Summary of the organis
 Staphylococcus aureus S. aureus (MRSA) vancomycin (VCM), arbekacin (ABK) Streptococcus pneumoniae cefuzonam (CZON), cefpirome (CPR) S. pneumoniae Enterococcus faecalis ampicillin (ABPC), imipenem (IPM)
Staphylococcus aureus S. aureus (MRSA) vancomycin (VCM), arbekacin (ABK) Streptococcus pneumoniae cefuzonam (CZON), cefpirome (CPR) S. pneumoniae Enterococcus faecalis ampicillin (ABPC), imipenem (IPM)
Streptococcus pneumoniae,streptococcus pyogenes,streptococcus agalactiae,neisseria gonorrhoeae,h.influenzae,moraxella subgenus Branhamella catarrharis
 Streptococcus pneumoniae,streptococcus pyogenes,streptococcus agalactiae,neisseria gonorrhoeae,h.influenzae,moraxella subgenus Branhamella catarrharis, E.coil,Klebsiella pneumoniae,klebsiella oxytoca,proteus
Streptococcus pneumoniae,streptococcus pyogenes,streptococcus agalactiae,neisseria gonorrhoeae,h.influenzae,moraxella subgenus Branhamella catarrharis, E.coil,Klebsiella pneumoniae,klebsiella oxytoca,proteus
THE JAPANESE JOURNAL OF ANTIBIOTICS ( 79)
 346 ( 78) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 2007 72 12,919 NTT THE JAPANESE JOURNAL OF ANTIBIOTICS 62 44 347 ( 79) 348 ( 80) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 THE JAPANESE JOURNAL OF
346 ( 78) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 2007 72 12,919 NTT THE JAPANESE JOURNAL OF ANTIBIOTICS 62 44 347 ( 79) 348 ( 80) THE JAPANESE JOURNAL OF ANTIBIOTICS 62 _ 4 THE JAPANESE JOURNAL OF
VOL.48 NO.7 lase negative staphylococci, Escherichia coli, Klebsiella spp., Citrobacter freundii, Enterobacter spp., indole-positive Proteus, Serratia
 ceftazidime, cefpirome, cefepime, cefoperazone/sulbactam (2: 1), imipenem Staphylococcus aureus oxacillin coagulase negative staphylococci Escherichia coli piperacillin Klebsiellac spp. Citrobacter Pseudomonas
ceftazidime, cefpirome, cefepime, cefoperazone/sulbactam (2: 1), imipenem Staphylococcus aureus oxacillin coagulase negative staphylococci Escherichia coli piperacillin Klebsiellac spp. Citrobacter Pseudomonas
THE JAPANESE JOURNAL OF ANTIBIOTICS 68 3 June 2015 Streptococcus pneumoniae, Haemophilus influenzae, Moraxella catarrhalis % 2 S. pneumon
 June 2015 THE JAPANESE JOURNAL OF ANTIBIOTICS 68 3 189 49 1 : 14 1 2 2 3 1 2 3 2015 4 3 1 : 14 CVA/AMPC 1 : 14 27 CVA/AMPC 1 : 14 88.5% Streptococcus pneumoniae, Haemophilus influenzae, Moraxella catarrhalis
June 2015 THE JAPANESE JOURNAL OF ANTIBIOTICS 68 3 189 49 1 : 14 1 2 2 3 1 2 3 2015 4 3 1 : 14 CVA/AMPC 1 : 14 27 CVA/AMPC 1 : 14 88.5% Streptococcus pneumoniae, Haemophilus influenzae, Moraxella catarrhalis
R06_01
 Staphylococcus aureus (MSSA) PCG (N=118,334) 57,369 (48.5%) 判定不能 :3 (0.0%) 60,962 (51.5%) CEZ (N=143,723) I:42 (0.0%) 143,635 (99.9%) R:46 (0.0%) CVA/AMPC (N=19,281) R:14 (0.1%) 19,265 (99.9%) 判定不能 :2
Staphylococcus aureus (MSSA) PCG (N=118,334) 57,369 (48.5%) 判定不能 :3 (0.0%) 60,962 (51.5%) CEZ (N=143,723) I:42 (0.0%) 143,635 (99.9%) R:46 (0.0%) CVA/AMPC (N=19,281) R:14 (0.1%) 19,265 (99.9%) 判定不能 :2
03-b-„FŒ{›xŒ¾-4.02
 518( 30 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 Dec. 25 2003 1. * * Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 519( 31 ) 9 5 2003 8 2004 7 14 565 701 258 (36.8%) 443 (63.2%) Staphylococcus aureus
518( 30 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 Dec. 25 2003 1. * * Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 519( 31 ) 9 5 2003 8 2004 7 14 565 701 258 (36.8%) 443 (63.2%) Staphylococcus aureus
Oct THE JAPANESE JOURNAL OF ANTIBIOTICS Pseudomonas aeruginosa 186 P. aeruginosa piperacillin PIPC, taz
 Oct. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 5 327 27 2013 2014 2016 7 5 2013 2014 Pseudomonas aeruginosa 186 P. aeruginosa piperacillin PIPC, tazobactam/piperacillin TAZ/PIPC, ceftazidime CAZ, cefepime
Oct. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 5 327 27 2013 2014 2016 7 5 2013 2014 Pseudomonas aeruginosa 186 P. aeruginosa piperacillin PIPC, tazobactam/piperacillin TAZ/PIPC, ceftazidime CAZ, cefepime
Feb THE JAPANESE JOURNAL OF ANTIBIOTICS Tebipenem pivoxil 1 1, Meiji Seika 2 Meiji Seika G 3 Meiji Seika Tebipen
 Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 53 53 Tebipenem pivoxil 1 1, 3 2 2 1 1 Meiji Seika 2 Meiji Seika G 3 Meiji Seika 2015 12 15 Tebipenem pivoxil 10% 2010 4 2013 3 3,547 3,540 3,540 3,331
Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 53 53 Tebipenem pivoxil 1 1, 3 2 2 1 1 Meiji Seika 2 Meiji Seika G 3 Meiji Seika 2015 12 15 Tebipenem pivoxil 10% 2010 4 2013 3 3,547 3,540 3,540 3,331
THE JAPANESE JOURNAL OF ANTIBIOTICS 63 13 243 ( 37 ) 2007 12 2008 5 19 863 methicillin-susceptible Staphylococcus aureus (MSSA) Escherichia coli levof
 242 ( 36 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 63 _ 3 prulifloxacin * ** ** CMC * ** 2010 2 22 Prulifloxacin ulifloxacin (UFX) 3 1 2003 12 2004 5 19 534 2 2005 12 2006 5 19 805 3 THE JAPANESE JOURNAL OF
242 ( 36 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 63 _ 3 prulifloxacin * ** ** CMC * ** 2010 2 22 Prulifloxacin ulifloxacin (UFX) 3 1 2003 12 2004 5 19 534 2 2005 12 2006 5 19 805 3 THE JAPANESE JOURNAL OF
CHEMOTHERAPY
 CHEMOTHERAPY VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin CHEMOTHERAPY AUG. 1993 VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin Table 1. Comparative in vitro activity of teicoplanin
CHEMOTHERAPY VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin CHEMOTHERAPY AUG. 1993 VOL.41 S-2 Laboratory and clinical evaluation of teicoplanin Table 1. Comparative in vitro activity of teicoplanin
 172( 38 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 2 Apr. 2002 1 19 6 2002 5 8 4 254 254 (PBP) 90 83 65 142 PBP pbp1a, pbp2x, pbp2b 121 (49%), pbp1a, pbp2x 30 (12%), pbp2x, pbp2b 16 (6%), pbp2x 61 (24%),
172( 38 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 2 Apr. 2002 1 19 6 2002 5 8 4 254 254 (PBP) 90 83 65 142 PBP pbp1a, pbp2x, pbp2b 121 (49%), pbp1a, pbp2x 30 (12%), pbp2x, pbp2b 16 (6%), pbp2x 61 (24%),
 Table 1.Resistance criteria Fig.1.The resistance rates of piperacillin,ceftazidime, cefsulodin,imipenem,aztreonam,gentamicin,tobramycin,amikacin,isepamicin,fosfomycin and ofloxacin against 2,793 strains
Table 1.Resistance criteria Fig.1.The resistance rates of piperacillin,ceftazidime, cefsulodin,imipenem,aztreonam,gentamicin,tobramycin,amikacin,isepamicin,fosfomycin and ofloxacin against 2,793 strains
 THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 33( 33 ) 2002 JA * 1 * 2 2003 12 15 * 1) * 2) 34( 34 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 Feb. 1982 7 2002 (2002.4 2003.3) 1 174 131 (75.3%) 334 171 163 Staphylococcus
THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 33( 33 ) 2002 JA * 1 * 2 2003 12 15 * 1) * 2) 34( 34 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 Feb. 1982 7 2002 (2002.4 2003.3) 1 174 131 (75.3%) 334 171 163 Staphylococcus
CHEMOTHERAPY Proteus mirabilis GN-79 Escherichia coli No. 35 Proteus vulgaris GN-76 Pseudomonas aeruginosa No. 11 Escherichia coli ML-1410 RGN-823 Kle
 VOL. 29 NO.8 CHEMOTHERAPY 865 CHEMOTHERAPY Proteus mirabilis GN-79 Escherichia coli No. 35 Proteus vulgaris GN-76 Pseudomonas aeruginosa No. 11 Escherichia coli ML-1410 RGN-823 Klebsiella pneumoniae GN-69
VOL. 29 NO.8 CHEMOTHERAPY 865 CHEMOTHERAPY Proteus mirabilis GN-79 Escherichia coli No. 35 Proteus vulgaris GN-76 Pseudomonas aeruginosa No. 11 Escherichia coli ML-1410 RGN-823 Klebsiella pneumoniae GN-69
THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterococcus avium 5Š, Corynebacterium xerosis 10Š, Corynebacterium pseudodiphtheriticum 10Š, Corynebacterium
 THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterobacter spp., Serratia spp., Burkholderia cepacia, Flavobacterium spp., Alcaligenes spp. THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterococcus avium 5Š, Corynebacterium
THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterobacter spp., Serratia spp., Burkholderia cepacia, Flavobacterium spp., Alcaligenes spp. THE JAPANESE JOURNAL OF ANTIBIOTICS 48-8 Enterococcus avium 5Š, Corynebacterium
 70( 70 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 Feb. Meropenem 2002 * * * * * * * * * * * * * * * * * * * * * * NTT Feb. THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 71( 71 ) * * * * 2003 12 22 Meropenem
70( 70 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 Feb. Meropenem 2002 * * * * * * * * * * * * * * * * * * * * * * NTT Feb. THE JAPANESE JOURNAL OF ANTIBIOTICS 57 1 71( 71 ) * * * * 2003 12 22 Meropenem
 1.Streptococcus pneumoniae, Streptococcus pyogenes JC-1,S.aureus Smith,methicillin (DMPPC)- susceptible S. aureus subsp. aureus (MSSA) TR101, DMPPC-resistant S. aureus subsp. aureus (MRSA) TR102, Staphylococcus
1.Streptococcus pneumoniae, Streptococcus pyogenes JC-1,S.aureus Smith,methicillin (DMPPC)- susceptible S. aureus subsp. aureus (MSSA) TR101, DMPPC-resistant S. aureus subsp. aureus (MRSA) TR102, Staphylococcus
366 12 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 Dec. 2012 1 8 DNA 2,3 16 12 20 171 2008 12 2010 11 2 3,558 4.44% 1.65% 1.17% 90% 9 Escherichia coli -
 Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 365 11 sita oxacin 1 1 1 1 1 1 2 2 3 3 1 1 1 2 3 2012 9 14 sita oxacin STFX 50 mg 10% 2008 1 2008 12 2010 11 2 STFX 1,452 91.4% 1,235/1,351 95.9% 466/486
Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 365 11 sita oxacin 1 1 1 1 1 1 2 2 3 3 1 1 1 2 3 2012 9 14 sita oxacin STFX 50 mg 10% 2008 1 2008 12 2010 11 2 STFX 1,452 91.4% 1,235/1,351 95.9% 466/486
1272 CHEMOTHERAPY MAR. 1975
 1272 CHEMOTHERAPY MAR. 1975 VOL. 23 NO. 3 CHEMOTHERAPY 1273 Fig. 2 Minimal inhibitory concentration of aminoglycosides against 50 strains of Klebsiella Fig. 1 Minimal inhibitory concentration of aminoglycosides
1272 CHEMOTHERAPY MAR. 1975 VOL. 23 NO. 3 CHEMOTHERAPY 1273 Fig. 2 Minimal inhibitory concentration of aminoglycosides against 50 strains of Klebsiella Fig. 1 Minimal inhibitory concentration of aminoglycosides
Staphylococcus sp. K.pneumoniae P.mirabilis C.freundii E. cloacae Serratia sp. P. aeruginosa ml, Enterococcus avium >100ƒÊg/ml
 CHEMOTHERAPY SEPT. 1992 cefoperazone ceftazidime (CAZ), imipenem (IPM) Staphylococcus sp., Enterococcus (CPZ), faecalis, Escherichia coli, Klebsiella pneumoniae, Citrobacter freundii, Enterobacter cloacae,
CHEMOTHERAPY SEPT. 1992 cefoperazone ceftazidime (CAZ), imipenem (IPM) Staphylococcus sp., Enterococcus (CPZ), faecalis, Escherichia coli, Klebsiella pneumoniae, Citrobacter freundii, Enterobacter cloacae,
CHEMOTHERAPY FEB Table 1. Activity of cefpirome and others against clinical isolates
 VOL.39 S-1 CHEMOTHERAPY FEB. 1981 Table 1. Activity of cefpirome and others against clinical isolates VOL.39 S-1 CHEMOTHERAPY FEB. 1991 72 M, 55.5 kg 66 F, 53 kg Chronic bronchitis Bronchopneumonia Peak
VOL.39 S-1 CHEMOTHERAPY FEB. 1981 Table 1. Activity of cefpirome and others against clinical isolates VOL.39 S-1 CHEMOTHERAPY FEB. 1991 72 M, 55.5 kg 66 F, 53 kg Chronic bronchitis Bronchopneumonia Peak
 Table 1 Survival rates of infected mice given antibiotic doses producing peak serum a) S. aurcus Smith Challenge dose :7 ~10 (5% mucin) CFU/mouse. LD50: 1 ~103 (5% mucin) CFU/mouse. Table 2 Survival rates
Table 1 Survival rates of infected mice given antibiotic doses producing peak serum a) S. aurcus Smith Challenge dose :7 ~10 (5% mucin) CFU/mouse. LD50: 1 ~103 (5% mucin) CFU/mouse. Table 2 Survival rates
epidermidis, Enterococcus faecalis, Enterococcus Klebsiella pneumoniae, Proteus mirabilis, indolepositive Proteus spp., Enterobacter spp., Serratia
 epidermidis, Enterococcus faecalis, Enterococcus Klebsiella pneumoniae, Proteus mirabilis, indolepositive Proteus spp., Enterobacter spp., Serratia Table 3. Overall clinical efficacy of cefozopran in
epidermidis, Enterococcus faecalis, Enterococcus Klebsiella pneumoniae, Proteus mirabilis, indolepositive Proteus spp., Enterobacter spp., Serratia Table 3. Overall clinical efficacy of cefozopran in
 Table 1 Sensitivity distribution of clinical isolates 1. Escherichia coli Inoculum size: 106cells/ml 2. Klebsiella pneumoniae 3. Enterobacter cloacae 4. Serratia marcescens Inoculum size: 106cells/nil
Table 1 Sensitivity distribution of clinical isolates 1. Escherichia coli Inoculum size: 106cells/ml 2. Klebsiella pneumoniae 3. Enterobacter cloacae 4. Serratia marcescens Inoculum size: 106cells/nil
Fig. 1 Chemical structure of DL-8280
 Fig. 1 Chemical structure of DL-8280 Fig. 2 Susceptibility of cl in ical isolates to DL4280 Fig. 5 Susceptibility of clinical isolates to DL-8280 Fig. 3 Susceptibility of clinical isolates to DL-8280 Fig.
Fig. 1 Chemical structure of DL-8280 Fig. 2 Susceptibility of cl in ical isolates to DL4280 Fig. 5 Susceptibility of clinical isolates to DL-8280 Fig. 3 Susceptibility of clinical isolates to DL-8280 Fig.
 Table 1.Quality control of MICs for reference strains Table 2.Antimicrobial activity of gatifloxacin against aerobic bacteria Table 4.Antimicrobial activity of gatifloxacin and other quinolones against
Table 1.Quality control of MICs for reference strains Table 2.Antimicrobial activity of gatifloxacin against aerobic bacteria Table 4.Antimicrobial activity of gatifloxacin and other quinolones against
VOL. 43 NO. 4
 VOL. 43 NO. 4 Fig. 1. Frequency of Enterococcus species from complicated UTI, 1988-1992. the number * of Enterococcus species/the number of cases with complicated UTI. Fig. 3 Epidemiologic characteristics
VOL. 43 NO. 4 Fig. 1. Frequency of Enterococcus species from complicated UTI, 1988-1992. the number * of Enterococcus species/the number of cases with complicated UTI. Fig. 3 Epidemiologic characteristics
2 2 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 1 Feb. 2012 CLSI M100-S17benzylpenicillin PCG MIC 0.05 g/ml S. pneumoniae penicillin-susceptible S. pneumon
 Feb. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 1 1 1 2008 2009 2011 10 25 2008 6 2009 4 Streptococcus pneumoniae 377 penicillin-binding protein: PBP 2004 S. pneumoniae 160 2 2 THE JAPANESE JOURNAL OF
Feb. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 1 1 1 2008 2009 2011 10 25 2008 6 2009 4 Streptococcus pneumoniae 377 penicillin-binding protein: PBP 2004 S. pneumoniae 160 2 2 THE JAPANESE JOURNAL OF
VOL.32 S-7 CHEMOTHERAPY Table 1 MIC of standard strains of CTRX Fig. 2 Cumulative curves of MIC S. aureus (26 strains )
 CHEMOTHERAPY OCT. 1984 Fig. I Chemical structure of CTRX VOL.32 S-7 CHEMOTHERAPY Table 1 MIC of standard strains of CTRX Fig. 2 Cumulative curves of MIC S. aureus (26 strains ) CHEMOTHERAPY Fig. 3 Cumulative
CHEMOTHERAPY OCT. 1984 Fig. I Chemical structure of CTRX VOL.32 S-7 CHEMOTHERAPY Table 1 MIC of standard strains of CTRX Fig. 2 Cumulative curves of MIC S. aureus (26 strains ) CHEMOTHERAPY Fig. 3 Cumulative
Table 1. Antibacterial activitiy of grepafloxacin and other antibiotics against clinical isolates
 Table 1. Antibacterial activitiy of grepafloxacin and other antibiotics against clinical isolates Table 2-1. Summary of patients treated with grepafloxacin for respiratory infection 1) Out: outpatient,
Table 1. Antibacterial activitiy of grepafloxacin and other antibiotics against clinical isolates Table 2-1. Summary of patients treated with grepafloxacin for respiratory infection 1) Out: outpatient,
PCG = Benzylpenicillin ABPC= Ampicillin AMPC= Amoxicillin MPIPC = Oxacillin MCIPC = Cloxacillin SBPC= Sulbenicillin PIPC= Piperacillin
 Key words : Clinical isolates, Antibacterial susceptibility, Scale of hospital PCG = Benzylpenicillin ABPC= Ampicillin AMPC= Amoxicillin MPIPC = Oxacillin MCIPC = Cloxacillin SBPC= Sulbenicillin PIPC=
Key words : Clinical isolates, Antibacterial susceptibility, Scale of hospital PCG = Benzylpenicillin ABPC= Ampicillin AMPC= Amoxicillin MPIPC = Oxacillin MCIPC = Cloxacillin SBPC= Sulbenicillin PIPC=
 CHEMOTHERAPY OCT. 1994 Tazobactam Piperacillin Fig. I. Chemical structures of tazobactam and piperacillin. Table 1. Media used for preculture and MIC determination BHIB: Brain heart infusion broth (Difco),
CHEMOTHERAPY OCT. 1994 Tazobactam Piperacillin Fig. I. Chemical structures of tazobactam and piperacillin. Table 1. Media used for preculture and MIC determination BHIB: Brain heart infusion broth (Difco),
VOL.47 NO.5 Table 1. Susceptibility distribution of Ĉ- lactams against clinical isolates of MRSA MRSA: rnethicillin- resistant Staphylococcus aureus
 MAY 1999 VOL.47 NO.5 Table 1. Susceptibility distribution of ƒà- lactams against clinical isolates of MRSA MRSA: rnethicillin- resistant Staphylococcus aureus (oxacillin MIC: 4ƒÊg/ ml) FMOX: flomoxef,
MAY 1999 VOL.47 NO.5 Table 1. Susceptibility distribution of ƒà- lactams against clinical isolates of MRSA MRSA: rnethicillin- resistant Staphylococcus aureus (oxacillin MIC: 4ƒÊg/ ml) FMOX: flomoxef,
 Key words : R-plasmid, Urinary tract infection, E. coli Fig. 1. MIC distribution against E. coli isolated from urinary tract (366 strains) and isolation - frequencies of drug-resistant strains Table 1.
Key words : R-plasmid, Urinary tract infection, E. coli Fig. 1. MIC distribution against E. coli isolated from urinary tract (366 strains) and isolation - frequencies of drug-resistant strains Table 1.
R01
 1. 集計対象医療機関数 (1,792 医療機関 ) 13.2% (7 医療機関 ) 900 床以上 N=53 86.8% (46 医療機関 ) 19.2% (70 医療機関 ) 500 899 床 N=365 80.8% (295 医療機関 ) JANIS 参加 * 200 499 床 N=2,231 43.4% (968 医療機関 ) 56.6% (1,263 医療機関 ) JANIS 参加 200
1. 集計対象医療機関数 (1,792 医療機関 ) 13.2% (7 医療機関 ) 900 床以上 N=53 86.8% (46 医療機関 ) 19.2% (70 医療機関 ) 500 899 床 N=365 80.8% (295 医療機関 ) JANIS 参加 * 200 499 床 N=2,231 43.4% (968 医療機関 ) 56.6% (1,263 医療機関 ) JANIS 参加 200
Fig.1 Chemical structure of BAY o 9867
 Fig.1 Chemical structure of BAY o 9867 CHEMOTHERAPY 43 Table 3 Antibacterial spectrum of gram negative bacteria Medium:Heart infusion agar (Nissui) Method:Agar dilution (Streak) CHEMOTHERAPY DEC 1985
Fig.1 Chemical structure of BAY o 9867 CHEMOTHERAPY 43 Table 3 Antibacterial spectrum of gram negative bacteria Medium:Heart infusion agar (Nissui) Method:Agar dilution (Streak) CHEMOTHERAPY DEC 1985
Table 1. Antibacterial spectrum SBT ABPC ABPC CPZ : sulbactamiampicillin : ampicillin : cefoperazone
 Table 1. Antibacterial spectrum SBT ABPC ABPC CPZ : sulbactamiampicillin : ampicillin : cefoperazone (inoculum size= 106 CFU/ml) (Ĉ-lactamase producer : 2 strains) Fig. 1. Sensitivity distribution of
Table 1. Antibacterial spectrum SBT ABPC ABPC CPZ : sulbactamiampicillin : ampicillin : cefoperazone (inoculum size= 106 CFU/ml) (Ĉ-lactamase producer : 2 strains) Fig. 1. Sensitivity distribution of
 Table 1. Antibacterial activity of cefdinir, cefixime, cefteram, cefuroxime, cefaclor and amoxicillin against standard strains Inoculum size: 108 cells/ml CFDN: cefdinir, CFIX: cefixime, CFTM: cefteram,
Table 1. Antibacterial activity of cefdinir, cefixime, cefteram, cefuroxime, cefaclor and amoxicillin against standard strains Inoculum size: 108 cells/ml CFDN: cefdinir, CFIX: cefixime, CFTM: cefteram,
CHEMOTHERAPY APRIL 1992 Acinetobacter calcoaceticus Staphylococcus aureus, Escherichia coli P. aeruginosa E. eoli, Klebsiella pneumoniae Serratia marc
 APRIL 1992 Acinetobacter calcoaceticus Staphylococcus aureus, Escherichia coli P. aeruginosa E. eoli, Klebsiella pneumoniae Serratia marcescens P. aeruginosa P. aeruginosa Streptococcus pyogenes Streptococcus
APRIL 1992 Acinetobacter calcoaceticus Staphylococcus aureus, Escherichia coli P. aeruginosa E. eoli, Klebsiella pneumoniae Serratia marcescens P. aeruginosa P. aeruginosa Streptococcus pyogenes Streptococcus
02-(a)-Łi’ì™·Łv-4.11
 THE JAPANESE JOURNAL OF ANTIBIOTICS 56 2 105( 13 ) 2001 1) 2) 3) JA 2 7 1) 2) 3) 106( 14 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 56 2 Apr. 1982 7 2001 (2001.4 2002.3) 1 221 175 (79.2%) 420 186 234 Staphylococcus
THE JAPANESE JOURNAL OF ANTIBIOTICS 56 2 105( 13 ) 2001 1) 2) 3) JA 2 7 1) 2) 3) 106( 14 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 56 2 Apr. 1982 7 2001 (2001.4 2002.3) 1 221 175 (79.2%) 420 186 234 Staphylococcus
CHEMOTHERAPY JUNE 1987 Table1 Media used *BHIB, brain heart infusion broth (Difco); /3 -NAD, S -nicotinamidoadeninedinucleotide (Sigma Chemical Co.);
 VOL.35 S-2 CHEMOTHERAPY Fig.1 Chemical structure of carumonam CHEMOTHERAPY JUNE 1987 Table1 Media used *BHIB, brain heart infusion broth (Difco); /3 -NAD, S -nicotinamidoadeninedinucleotide (Sigma Chemical
VOL.35 S-2 CHEMOTHERAPY Fig.1 Chemical structure of carumonam CHEMOTHERAPY JUNE 1987 Table1 Media used *BHIB, brain heart infusion broth (Difco); /3 -NAD, S -nicotinamidoadeninedinucleotide (Sigma Chemical
CHEMOTHERAPY Methicillin-resistant S.aureus(MRSA) coccus epidermidis 105 Streptococcus pyogenes E.faecali senterococcus avium Enterococcus faecium Str
 cefaclor(ccl),cefuroxime(cxm),cefixime (CFIX),cefteram(CFTM),cefdinir(CFDN) pneumoniae,streptococcus pyogenes Moraxella catarrhalis,haemophilus influenzae,escherichia coli, Klebsiella pneumoniae,proteus
cefaclor(ccl),cefuroxime(cxm),cefixime (CFIX),cefteram(CFTM),cefdinir(CFDN) pneumoniae,streptococcus pyogenes Moraxella catarrhalis,haemophilus influenzae,escherichia coli, Klebsiella pneumoniae,proteus
Nationwide surveillance of bacterial respiratory pathogens conducted by the Surveillance Committee of Japanese Society of Chemotherapy, Japanese Assoc
 J Infect Chemother (2012) 18:609 620 DOI 10.1007/s10156-012-0434-3 SURVEILLANCE Nationwide surveillance of bacterial respiratory pathogens conducted by the Surveillance Committee of Japanese Society of
J Infect Chemother (2012) 18:609 620 DOI 10.1007/s10156-012-0434-3 SURVEILLANCE Nationwide surveillance of bacterial respiratory pathogens conducted by the Surveillance Committee of Japanese Society of
CHEMOTHERAPY
 CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of Sulbactam/CPZ against standard strains MIC mg/ml Inoculum size 106 CFU/ml * Sulbactam/CPZ= 1: 1 ** Concentration of Sulbactam+ CPZ CHEMOTHERAPY
CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of Sulbactam/CPZ against standard strains MIC mg/ml Inoculum size 106 CFU/ml * Sulbactam/CPZ= 1: 1 ** Concentration of Sulbactam+ CPZ CHEMOTHERAPY
日本化学療法学会雑誌第59巻第5号
 Streptococcus pneumoniae Haemophilus influenzae Moraxella catarrhalis S. pneumoniae H. influenzae M. catarrhalis S. pneumoniae H. influenzae M. catarrhalis S. pneumoniae H. influenzae M. catarrhalis S.
Streptococcus pneumoniae Haemophilus influenzae Moraxella catarrhalis S. pneumoniae H. influenzae M. catarrhalis S. pneumoniae H. influenzae M. catarrhalis S. pneumoniae H. influenzae M. catarrhalis S.
988 CHEMOTHERAPY NOV. 1971
 988 CHEMOTHERAPY NOV. 1971 VOL. 19 NO. 8 CHEMOTHERAPY 989 Effect of medium-ph and inoculum size on activity of SB-PC heart infusion agar, mcg/ml Sensitivity distribution of Staphylococci to SB-PC in surgical
988 CHEMOTHERAPY NOV. 1971 VOL. 19 NO. 8 CHEMOTHERAPY 989 Effect of medium-ph and inoculum size on activity of SB-PC heart infusion agar, mcg/ml Sensitivity distribution of Staphylococci to SB-PC in surgical
 b) Gram-negative bacteria Fig. 2 Sensitivity distribution of clinical isolates : E. coli Fig. 3 Sensitivity distribution of clinical isolates : Pseudomonas Fig. 1 Sensitivity distribution of clinical isolates
b) Gram-negative bacteria Fig. 2 Sensitivity distribution of clinical isolates : E. coli Fig. 3 Sensitivity distribution of clinical isolates : Pseudomonas Fig. 1 Sensitivity distribution of clinical isolates
CHEMO THE RAPY OCT. 1994
 bilis (0.78), Proteus vulgaris (1.56), Enterococcus faecalis (3.13), Staphylococcus epidermidis (6.25), Klebsiella pneumoniae (6.25), Morganella morganii (6.25), Escherichia coli (12.5), Providencia rettgeri
bilis (0.78), Proteus vulgaris (1.56), Enterococcus faecalis (3.13), Staphylococcus epidermidis (6.25), Klebsiella pneumoniae (6.25), Morganella morganii (6.25), Escherichia coli (12.5), Providencia rettgeri
日本化学療法学会雑誌第57巻第1号
 In vitro Streptococcus pneumoniae Escherichia coli in vitro Streptococcus pneumoniae Escherichia coli µs. pneumoniae E. coli µ Key words in vitrostreptococcus pneumoniae Escherichia coli Escherichia coli
In vitro Streptococcus pneumoniae Escherichia coli in vitro Streptococcus pneumoniae Escherichia coli µs. pneumoniae E. coli µ Key words in vitrostreptococcus pneumoniae Escherichia coli Escherichia coli
スライド タイトルなし
 第 4 回ひびき臨床微生物シンポジュウム June 24,27, 港ハウス 感受性検査を読む ( 同定検査結果確認やスクリーニング検査と捉えて ) ( 株 ) キューリン小林とも子 キューリン微生物検査課 塗抹鏡検グラム染色 分離培養検査血液 BTB, エッグーヨーク 報告書作成結果承認 同定検査 VITEK TSI,LIM クリスタル NF 薬剤感受性検査 MIC2 ディスク法 薬剤感受性結果 (
第 4 回ひびき臨床微生物シンポジュウム June 24,27, 港ハウス 感受性検査を読む ( 同定検査結果確認やスクリーニング検査と捉えて ) ( 株 ) キューリン小林とも子 キューリン微生物検査課 塗抹鏡検グラム染色 分離培養検査血液 BTB, エッグーヨーク 報告書作成結果承認 同定検査 VITEK TSI,LIM クリスタル NF 薬剤感受性検査 MIC2 ディスク法 薬剤感受性結果 (
400 46 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 Dec. 2012 LVFX 100 mg 3 / 7 150 mg 2 / 7 2 2006 2008 9 LVFX PK PD 2009 7 100 mg 1 3 500 mg 1 1 AUC/MIC
 Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 399 45 2012 11 5 LVFX 500 mg 1 1 20 Chlamydia trachomatis C. trachomatismycoplasma genitalium M. genitalium LVFX 1 500 mg 1 1 7 22 22 C. trachomatis 17
Dec. 2012 THE JAPANESE JOURNAL OF ANTIBIOTICS 65 6 399 45 2012 11 5 LVFX 500 mg 1 1 20 Chlamydia trachomatis C. trachomatismycoplasma genitalium M. genitalium LVFX 1 500 mg 1 1 7 22 22 C. trachomatis 17
CHEMOTHERAPY JUN Citrobacter freundii 27, Enterobacter aerogenes 26, Enterobacter cloacae 27, Proteus rettgeri 7, Proteus inconstans 20, Proteus
 VOL. 32 S-4 CHEMOTHERAPY Fig. 1 Chemical structure of sodium cefoperazone Fig. 2 Chemical structure of sodium cefoperazone CHEMOTHERAPY JUN. 1984 Citrobacter freundii 27, Enterobacter aerogenes 26, Enterobacter
VOL. 32 S-4 CHEMOTHERAPY Fig. 1 Chemical structure of sodium cefoperazone Fig. 2 Chemical structure of sodium cefoperazone CHEMOTHERAPY JUN. 1984 Citrobacter freundii 27, Enterobacter aerogenes 26, Enterobacter
日本化学療法学会雑誌第53巻第S-3号
 moxifloxacin in vitro moxifloxacin in vitro 17 9 6 17 11 21 moxifloxacinmflx in vitro cefdinir CFDNclavulanic acidamoxicillincvaampcclarithromycincamclindamycincldm levofloxacinlvfx 1MFLX Clostridium clostridiiformeclostridium
moxifloxacin in vitro moxifloxacin in vitro 17 9 6 17 11 21 moxifloxacinmflx in vitro cefdinir CFDNclavulanic acidamoxicillincvaampcclarithromycincamclindamycincldm levofloxacinlvfx 1MFLX Clostridium clostridiiformeclostridium
浜松地区における耐性菌調査の報告
 平成 28 年度浜松地区感染対策地域連携を考える会 2017 年 2 月 22 日 浜松地区 耐性菌サーベイランス報告 浜松医科大学医学部附属病院 感染対策室 概要 平成 19 年 4 月に施行された改正医療法により すべての医療機関において管理者の責任の下で院内感染対策のための体制の確保が義務化されました 本サーベイランスは 静岡県浜松地区 ( 浜松市 湖西市 ) における薬剤耐性菌の分離状況や薬剤感受性の状況を調査し
平成 28 年度浜松地区感染対策地域連携を考える会 2017 年 2 月 22 日 浜松地区 耐性菌サーベイランス報告 浜松医科大学医学部附属病院 感染対策室 概要 平成 19 年 4 月に施行された改正医療法により すべての医療機関において管理者の責任の下で院内感染対策のための体制の確保が義務化されました 本サーベイランスは 静岡県浜松地区 ( 浜松市 湖西市 ) における薬剤耐性菌の分離状況や薬剤感受性の状況を調査し
MIC MIC...
 50 mg 10% 2.7.36 2.7.36 2.7.36... 1 1.6... 1 2.6... 3 3.6... 5 3.16... 5 3.26... 12 3.36... 16 4.6... 17 5.6... 19 6.6... 20 2.7.3.3.16-1 MIC... 9 2.7.3.3.16-2 MIC... 10 2.7.3.3.16-3 MIC E. coli... 11
50 mg 10% 2.7.36 2.7.36 2.7.36... 1 1.6... 1 2.6... 3 3.6... 5 3.16... 5 3.26... 12 3.36... 16 4.6... 17 5.6... 19 6.6... 20 2.7.3.3.16-1 MIC... 9 2.7.3.3.16-2 MIC... 10 2.7.3.3.16-3 MIC E. coli... 11
Feb THE JAPANESE JOURNAL OF ANTIBIOTICS ,4 2,4 2,4 2,3,4 2,3,4 2,3, ,3, Garenoxacin GRNX Levofloxacin LV
 Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 27 27 1,4 2,4 2,4 2,3,4 2,3,4 2,3,4 2 1 2,3,4 1 2 3 4 2015 10 21 9 Garenoxacin GRNX Levofloxacin LVFX Sitafloxacin STFX Moxifloxacin MFLX Pharmacokinetics-Pharmacodynamics
Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 27 27 1,4 2,4 2,4 2,3,4 2,3,4 2,3,4 2 1 2,3,4 1 2 3 4 2015 10 21 9 Garenoxacin GRNX Levofloxacin LVFX Sitafloxacin STFX Moxifloxacin MFLX Pharmacokinetics-Pharmacodynamics
日本化学療法学会雑誌第58巻第4号
 Escherichia coli Enterococcus faecalisstreptococcus agalactiae Klebsiella pneumoniae Staphylococcus epidermidis E. colie. faecalispseudomonas aeruginosa K. pneumoniae S. agalactiae E. coli E. coli μ p
Escherichia coli Enterococcus faecalisstreptococcus agalactiae Klebsiella pneumoniae Staphylococcus epidermidis E. colie. faecalispseudomonas aeruginosa K. pneumoniae S. agalactiae E. coli E. coli μ p
(ABPC), Carbenicillin (CBPC), Surbenicillin (SBPC), Piperacillin (PIPC), Cephalexin (CEX), Cefaclor (CCL), Cephalothin (CET), Cefazolin (CEZ), Cefotia
 Key words: Blood culture, Trend of bacterial isolation, Increasing of staphylococcus, Use of new cephems (ABPC), Carbenicillin (CBPC), Surbenicillin (SBPC), Piperacillin (PIPC), Cephalexin (CEX), Cefaclor
Key words: Blood culture, Trend of bacterial isolation, Increasing of staphylococcus, Use of new cephems (ABPC), Carbenicillin (CBPC), Surbenicillin (SBPC), Piperacillin (PIPC), Cephalexin (CEX), Cefaclor
公開情報 2016 年 1 月 ~12 月年報 ( 全集計対象医療機関 ) 院内感染対策サーベイランス検査部門 Citrobacter koseri Proteus mirabilis Proteus vulgaris Serratia marcescens Pseudomonas aerugino
 公開情報 2016 年 1 月 ~12 月年報 ( 全集計対象医療機関 ) 院内感染対策サーベイランス検査部門 検査部門におけるサーベイランスの概要と目的 本サーベイランスの目的は 細菌検査により検出される主要な細菌の分離頻度とその抗菌薬感受性を継続的に収集 解析し 医療機関における主要な細菌ならびに薬剤耐性菌の分離状況を明らかにすることである サーベイランスの対象となる主要菌ならびに薬剤耐性菌の分離率は
公開情報 2016 年 1 月 ~12 月年報 ( 全集計対象医療機関 ) 院内感染対策サーベイランス検査部門 検査部門におけるサーベイランスの概要と目的 本サーベイランスの目的は 細菌検査により検出される主要な細菌の分離頻度とその抗菌薬感受性を継続的に収集 解析し 医療機関における主要な細菌ならびに薬剤耐性菌の分離状況を明らかにすることである サーベイランスの対象となる主要菌ならびに薬剤耐性菌の分離率は
小児感染症分離株における感受性サーベイランス
 小児感染症分離株における 感受性サーベイランス 公益社団法人日本化学療法学会, 一般社団法人日本感染症学会, 日本小児感染症学会小児用キノロン薬適正使用推進委員会委員長 : 渡辺彰委員 : 岩田敏, 坂田宏, 佐藤吉壮, 鈴木賢二, 宮下修行, 堀誠治, 山口禎夫協力委員 : 小田島正明, 交久瀬善隆, 長谷川寿一, 牧展子, 和田光市 はじめに 2009 年 12 月に耐性菌感染症治療のために二次選択薬として承認された小児用キノロン薬の再審査期間の
小児感染症分離株における 感受性サーベイランス 公益社団法人日本化学療法学会, 一般社団法人日本感染症学会, 日本小児感染症学会小児用キノロン薬適正使用推進委員会委員長 : 渡辺彰委員 : 岩田敏, 坂田宏, 佐藤吉壮, 鈴木賢二, 宮下修行, 堀誠治, 山口禎夫協力委員 : 小田島正明, 交久瀬善隆, 長谷川寿一, 牧展子, 和田光市 はじめに 2009 年 12 月に耐性菌感染症治療のために二次選択薬として承認された小児用キノロン薬の再審査期間の
 CHEMOTHERAPY APRIL 1992 VOL. 40 S- 1 Table 1-1. Comparative in vitro activity of meropenem against clinical isolates CNS: coagulase-negative staphylococci CHEMOTHERAPY APRIL 1992 Table 1-2. Comparative
CHEMOTHERAPY APRIL 1992 VOL. 40 S- 1 Table 1-1. Comparative in vitro activity of meropenem against clinical isolates CNS: coagulase-negative staphylococci CHEMOTHERAPY APRIL 1992 Table 1-2. Comparative
 VOL.30 NO.12 CHEMOTHERAPY Fig. 1 Effect of temperature on the growth curve of A. calcoaceticus A. calcoaceticits Ac 54 A. calcoacetictts Ac 164 Fig. 2 Effect of medium ph on the growth curve of A. calcoaceticus
VOL.30 NO.12 CHEMOTHERAPY Fig. 1 Effect of temperature on the growth curve of A. calcoaceticus A. calcoaceticits Ac 54 A. calcoacetictts Ac 164 Fig. 2 Effect of medium ph on the growth curve of A. calcoaceticus
Clostridium difficile ciprofloxacin, ofloxacin, norfloxacin Bifidobacterium Lactobacillus Lactobacillus Bacteroides fragilis B. fragilis C. difficile
 Clostridium difficile ciprofloxacin, ofloxacin, norfloxacin Bifidobacterium Lactobacillus Lactobacillus Bacteroides fragilis B. fragilis C. difficile Key words: temafloxacin, TA-167, Bacteroides fragilis,
Clostridium difficile ciprofloxacin, ofloxacin, norfloxacin Bifidobacterium Lactobacillus Lactobacillus Bacteroides fragilis B. fragilis C. difficile Key words: temafloxacin, TA-167, Bacteroides fragilis,
VOL. 23 NO. 3 CHEMOTHERAPY 1067 Table 2 Sensitivity of gram positive cocci isolated from various diagnostic materials Table 3 Sensitivity of gram nega
 1066 CHEMOTHERAPY MAR. 1975 Table 1 Sensitivity of standard strains VOL. 23 NO. 3 CHEMOTHERAPY 1067 Table 2 Sensitivity of gram positive cocci isolated from various diagnostic materials Table 3 Sensitivity
1066 CHEMOTHERAPY MAR. 1975 Table 1 Sensitivity of standard strains VOL. 23 NO. 3 CHEMOTHERAPY 1067 Table 2 Sensitivity of gram positive cocci isolated from various diagnostic materials Table 3 Sensitivity
coccus aureus Corynebacterium sp, Haemophilus parainfluenzae Klebsiella pneumoniae Pseudornonas aeruginosa Pseudomonas sp., Xanthomonas maltophilia, F
 VOL.43 S-1 coccus aureus Corynebacterium sp, Haemophilus parainfluenzae Klebsiella pneumoniae Pseudornonas aeruginosa Pseudomonas sp., Xanthomonas maltophilia, Flavobacter- Table 1. Concentration of grepafloxacin
VOL.43 S-1 coccus aureus Corynebacterium sp, Haemophilus parainfluenzae Klebsiella pneumoniae Pseudornonas aeruginosa Pseudomonas sp., Xanthomonas maltophilia, Flavobacter- Table 1. Concentration of grepafloxacin
CHEMOTHERAPY
 CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of BRL 28500 against standard strains of bacteria Fig, 1 Sensitivity distribution of ABPC-resistant E. coli isolated from urinary tract Fig. 2 Sensitivity
CHEMOTHERAPY CHEMOTHERAPY Table 1 Antibacterial activity of BRL 28500 against standard strains of bacteria Fig, 1 Sensitivity distribution of ABPC-resistant E. coli isolated from urinary tract Fig. 2 Sensitivity
CHEMOTHERAPY NOV S. aureus, S. epidermidis, E. coli, K. pgeumoniae, E. cloacae, S. marcescens, P. mirabilis, Proteus, P. aeruginosa Inoculum siz
 VOL.33 S-5 CHEMOTHERAPY 381 Fig. 1 Chemical structure of HAPA-B Chemical name 1-N-[(2S)-3-Amino-2-hydroxypropiony1]-4-0-(6-amino- 6-deoxy-a-D-glucopyranosyl)-6-013-deoxy-4-C-methyl- 3-(methylamino)-ƒÀ-L-arabinopyranosyl]-2-deoxystreptamine
VOL.33 S-5 CHEMOTHERAPY 381 Fig. 1 Chemical structure of HAPA-B Chemical name 1-N-[(2S)-3-Amino-2-hydroxypropiony1]-4-0-(6-amino- 6-deoxy-a-D-glucopyranosyl)-6-013-deoxy-4-C-methyl- 3-(methylamino)-ƒÀ-L-arabinopyranosyl]-2-deoxystreptamine
Fig.2. Sensitivity distribution of clinical isolates of S. epidermidis (24 strains, 106 CFU/ml) Staphylococcus aureus Staphylococcus epider- midis Ent
 Fig.2. Sensitivity distribution of clinical isolates of S. epidermidis (24 strains, 106 CFU/ml) Staphylococcus aureus Staphylococcus epider- midis Enterococcus faecalis Klebsiella pneumoniae, Morganella
Fig.2. Sensitivity distribution of clinical isolates of S. epidermidis (24 strains, 106 CFU/ml) Staphylococcus aureus Staphylococcus epider- midis Enterococcus faecalis Klebsiella pneumoniae, Morganella
 概要 (2004 年分 ) 本サーベイランスは 参加医療機関において血液および髄液から分離された各種細菌の検出状況や薬剤感受性パターンの動向を把握するとともに 新たな耐性菌の早期検出等を目的とする これらのデータを経時的に解析し臨床の現場に還元することによって 抗菌薬の安全で有効な使用方法や院内感染制御における具体的かつ確実な情報を提供する 検体 ( ) 内は施設数 2002 年 2003 年 2004
概要 (2004 年分 ) 本サーベイランスは 参加医療機関において血液および髄液から分離された各種細菌の検出状況や薬剤感受性パターンの動向を把握するとともに 新たな耐性菌の早期検出等を目的とする これらのデータを経時的に解析し臨床の現場に還元することによって 抗菌薬の安全で有効な使用方法や院内感染制御における具体的かつ確実な情報を提供する 検体 ( ) 内は施設数 2002 年 2003 年 2004
pneumoniae 30, C. freundii 32, E. aerogenes 27, E. cloacae 32, P. mirabilis 31, P. vulgaris 34, M. morganii 32, S. marcescens 31, H. influenzae 27, P.
 pneumoniae 30, C. freundii 32, E. aerogenes 27, E. cloacae 32, P. mirabilis 31, P. vulgaris 34, M. morganii 32, S. marcescens 31, H. influenzae 27, P. aeruginosa 30, P. maltophilia pyogenes 32, Escherichia
pneumoniae 30, C. freundii 32, E. aerogenes 27, E. cloacae 32, P. mirabilis 31, P. vulgaris 34, M. morganii 32, S. marcescens 31, H. influenzae 27, P. aeruginosa 30, P. maltophilia pyogenes 32, Escherichia
CHEMOTHERAPY JUNE 1993 Table 1. Background of patients in pharmacokinetic study
 CHEMOTHERAPY JUNE 1993 Table 1. Background of patients in pharmacokinetic study VOL. 41 S 1 Table 2. Levels (Đg/ml or Đg/g) of S-1006 in serum, bile, and tissue (gallbladder) after oral administration
CHEMOTHERAPY JUNE 1993 Table 1. Background of patients in pharmacokinetic study VOL. 41 S 1 Table 2. Levels (Đg/ml or Đg/g) of S-1006 in serum, bile, and tissue (gallbladder) after oral administration
 Table 1 Antibacterial spectra of CPM and other antimicrobials against anaerobes Fig. 1 In vitro activity of CPM and other antibiotics against B. fragilis (136 strains) Fig. 2 In vitro activity of CPM and
Table 1 Antibacterial spectra of CPM and other antimicrobials against anaerobes Fig. 1 In vitro activity of CPM and other antibiotics against B. fragilis (136 strains) Fig. 2 In vitro activity of CPM and
Title 尿路感染症分離菌の年次的変遷と薬剤感受性の検討 ( ニューキノロン系を中心として ) 深津, 英捷 ; 本多, 靖明 ; 水本, 裕之 ; 瀧, 知弘 ; 三井, Author(s) 々村, 仁志 ; 羽田野, 幸夫 ; 平岩, 親輔 ; 吉川, 和宏 ; 山田彰 ; 瀬川, 昭夫 Ci
 Title 尿路感染症分離菌の年次的変遷と薬剤感受性の検討 ( ニューキノロン系を中心として ) 深津, 英捷 ; 本多, 靖明 ; 水本, 裕之 ; 瀧, 知弘 ; 三井, Author(s) 々村, 仁志 ; 羽田野, 幸夫 ; 平岩, 親輔 ; 吉川, 和宏 ; 山田彰 ; 瀬川, 昭夫 Citation 泌尿器科紀要 (1992), 38(11): 1215-1223 Issue Date
Title 尿路感染症分離菌の年次的変遷と薬剤感受性の検討 ( ニューキノロン系を中心として ) 深津, 英捷 ; 本多, 靖明 ; 水本, 裕之 ; 瀧, 知弘 ; 三井, Author(s) 々村, 仁志 ; 羽田野, 幸夫 ; 平岩, 親輔 ; 吉川, 和宏 ; 山田彰 ; 瀬川, 昭夫 Citation 泌尿器科紀要 (1992), 38(11): 1215-1223 Issue Date
Dec THE JAPANESE JOURNAL OF ANTIBIOTICS ( 45 ) ) 1) 2) 2) 3) 4) 4,5) 6) 6) 7) 8) 8) 9) 10) 11) 11) 12) 13) 13) 14) 14) 15) 15) 1
 Dec. 2010 THE JAPANESE JOURNAL OF ANTIBIOTICS 63 46 431 ( 45 ) 2006 1) 1) 2) 2) 3) 4) 4,5) 6) 6) 7) 8) 8) 9) 10) 11) 11) 12) 13) 13) 14) 14) 15) 15) 16) 16) 17) 17) 1) 1) 1) 2) 3) 4) 5) 6) 7) 8) 9) 10)
Dec. 2010 THE JAPANESE JOURNAL OF ANTIBIOTICS 63 46 431 ( 45 ) 2006 1) 1) 2) 2) 3) 4) 4,5) 6) 6) 7) 8) 8) 9) 10) 11) 11) 12) 13) 13) 14) 14) 15) 15) 16) 16) 17) 17) 1) 1) 1) 2) 3) 4) 5) 6) 7) 8) 9) 10)
VOL. 40 S- 1 Table 1. Susceptibility of methicillin-resistant Staphylococcus aureus to meropenem Table 2. Coagulase typing of methicillin-resistant St
 CHEMOTHERAPY VOL. 40 S- 1 Table 1. Susceptibility of methicillin-resistant Staphylococcus aureus to meropenem Table 2. Coagulase typing of methicillin-resistant Staphylococcus aureus CHEMOTHERAPY Table
CHEMOTHERAPY VOL. 40 S- 1 Table 1. Susceptibility of methicillin-resistant Staphylococcus aureus to meropenem Table 2. Coagulase typing of methicillin-resistant Staphylococcus aureus CHEMOTHERAPY Table
日本化学療法学会雑誌第50巻第6号
 13 11 30 14 4 22 Streptococcus pneumoniae Haemophilus influenzae amoxicillin AMPC cefditoren pivoxil CDTR AMPC 50 mg kg day CDTR 9mg kg day CDTR 18 mg kg day S. pneumoniae H. influenzae 8 17 25 1 25 S.
13 11 30 14 4 22 Streptococcus pneumoniae Haemophilus influenzae amoxicillin AMPC cefditoren pivoxil CDTR AMPC 50 mg kg day CDTR 9mg kg day CDTR 18 mg kg day S. pneumoniae H. influenzae 8 17 25 1 25 S.
 概要 (2006 年 1 2 3 月分 ) 本サーベイランスは 参加医療機関において血液および髄液から分離された各種細菌の検出状況や薬剤感受性パターンの動 向を把握するとともに 新たな耐性菌の早期検出等を目的とする これらのデータを経時的に解析し臨床の現場に還元することによって 抗菌薬の安全で有効な使用方法や院内感染制御における具体的かつ確実な情報を提供する 検体 2005 年 2006 年 10~12
概要 (2006 年 1 2 3 月分 ) 本サーベイランスは 参加医療機関において血液および髄液から分離された各種細菌の検出状況や薬剤感受性パターンの動 向を把握するとともに 新たな耐性菌の早期検出等を目的とする これらのデータを経時的に解析し臨床の現場に還元することによって 抗菌薬の安全で有効な使用方法や院内感染制御における具体的かつ確実な情報を提供する 検体 2005 年 2006 年 10~12
CHEMOTHERAPY Table 1 Clinical effect of Sultamicillin
 CHEMOTHERAPY CHEMOTHERAPY Table 1 Clinical effect of Sultamicillin CHEMOTHERAPY Fig. 1 MICs of sultamicillin against respiratory pathogenic Branhamella catarrhalis 62 strains, inoculum size 106CFU/m1 Fig.
CHEMOTHERAPY CHEMOTHERAPY Table 1 Clinical effect of Sultamicillin CHEMOTHERAPY Fig. 1 MICs of sultamicillin against respiratory pathogenic Branhamella catarrhalis 62 strains, inoculum size 106CFU/m1 Fig.
dihydrostreptomycin(sm), sulfanilamide(sa), kanamycin(km), paromomycin(prm), fradiomycin(frm), ampicillin(apc), cephaloridine (CER), nalidixic acid(na
 Key words: Shigella, Bacterial resistance against entibiotics. Distribution of R factors dihydrostreptomycin(sm), sulfanilamide(sa), kanamycin(km), paromomycin(prm), fradiomycin(frm), ampicillin(apc),
Key words: Shigella, Bacterial resistance against entibiotics. Distribution of R factors dihydrostreptomycin(sm), sulfanilamide(sa), kanamycin(km), paromomycin(prm), fradiomycin(frm), ampicillin(apc),
VOL.42 S-1 methicillin-susceptible Staphylococcus aureus (MSSA), Staphylococcus epidermidis, Enterococcus faecalis, Escherichia coli, Klebsiella pneum
 VOL.42 S-1 methicillin-susceptible Staphylococcus aureus (MSSA), Staphylococcus epidermidis, Enterococcus faecalis, Escherichia coli, Klebsiella pneumoniae, Enterobacter cloacae methicillin-resistant Staphylococcus
VOL.42 S-1 methicillin-susceptible Staphylococcus aureus (MSSA), Staphylococcus epidermidis, Enterococcus faecalis, Escherichia coli, Klebsiella pneumoniae, Enterobacter cloacae methicillin-resistant Staphylococcus
04-c-„FŒ{›xŒ¾-4.01
 544( 56 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 Dec. 25 2003 2. * * Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 545( 57 ) 9 5 2003 8 2004 714 565 719 50 20 39 0 9 70 79 44.4 91.7% Escherichia coli
544( 56 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 Dec. 25 2003 2. * * Dec. THE JAPANESE JOURNAL OF ANTIBIOTICS 58 6 545( 57 ) 9 5 2003 8 2004 714 565 719 50 20 39 0 9 70 79 44.4 91.7% Escherichia coli
Key words:group D streptococci,classification,enterococcal infections, Antibiotic susceptibility,vancomycin
 Key words:group D streptococci,classification,enterococcal infections, Antibiotic susceptibility,vancomycin Table 1 Differentiation of group D streptococcia aderived from R.R.Facklam1,2),K.C.Gross-et al3),and
Key words:group D streptococci,classification,enterococcal infections, Antibiotic susceptibility,vancomycin Table 1 Differentiation of group D streptococcia aderived from R.R.Facklam1,2),K.C.Gross-et al3),and
日本化学療法学会雑誌第66巻第2号
 173 Table 1.Detection rates of Neisseria gonorrhoeae, Chlamydia trachomatis, Mycoplasma genitalium, Ureaplasma urealyticum, Haemophilus influenzae and adenovirus from male urethritis in Urethritis No.
173 Table 1.Detection rates of Neisseria gonorrhoeae, Chlamydia trachomatis, Mycoplasma genitalium, Ureaplasma urealyticum, Haemophilus influenzae and adenovirus from male urethritis in Urethritis No.
 Fig.1 MICs of penicillins against 24 strains of B. pertussis Fig.2 MICs of cepherns against 24 strains of B. pertussis Fig.3 MICs of macrolides against 24 strains of B. pertussis Fig.4 MICs of nalidixic
Fig.1 MICs of penicillins against 24 strains of B. pertussis Fig.2 MICs of cepherns against 24 strains of B. pertussis Fig.3 MICs of macrolides against 24 strains of B. pertussis Fig.4 MICs of nalidixic
 CHEMOTHERAPY APRIL 1992 Table 2. Concentration of meropenem in human prostatic fluid Table 1. Background of 21 chronic complicated UTI cases * NB + BPH, NB + Kidney tumor, NB + Kidney tuberculosis Table
CHEMOTHERAPY APRIL 1992 Table 2. Concentration of meropenem in human prostatic fluid Table 1. Background of 21 chronic complicated UTI cases * NB + BPH, NB + Kidney tumor, NB + Kidney tuberculosis Table
_02三浦.indd
 36, 7-11, 2016 IPD PCV 5 3 80% 1 invasive pneumococcal disease ; IPD 2010 7 PCV7 2013 13 PCV13 IPD IPD 2,3 2015 1 2015 12 5 1 IPD 2015 1 12 IPD 5 IPD 1 4 2 5 http://pneumocatch.jp/ 5 Statens Serum Institut
36, 7-11, 2016 IPD PCV 5 3 80% 1 invasive pneumococcal disease ; IPD 2010 7 PCV7 2013 13 PCV13 IPD IPD 2,3 2015 1 2015 12 5 1 IPD 2015 1 12 IPD 5 IPD 1 4 2 5 http://pneumocatch.jp/ 5 Statens Serum Institut
HPM_442_F_TgCHG_1128
 3M TM Chlorhexidine Gluconate IV Securement Dressings Tegaderm TM CHG Support CRBSI Prevention TegadermTM CHG Dressing 2w/w% 60% N. Safdar, Intensive Care Med 2004 30 62-7 Guideline Centers for Disease
3M TM Chlorhexidine Gluconate IV Securement Dressings Tegaderm TM CHG Support CRBSI Prevention TegadermTM CHG Dressing 2w/w% 60% N. Safdar, Intensive Care Med 2004 30 62-7 Guideline Centers for Disease
「薬剤耐性菌判定基準」 改定内容
 Ver.3.1 Ver.3.2 改訂内容 (2019 年 1 月 ) 改訂対象改訂前改訂後 メチシリン耐性黄色ブドウ球菌 (MRSA) ペニシリン耐性肺炎球菌 (PRSP) 多剤耐性緑膿菌 (MDRP) 多剤耐性アシネトバクター属 (MDRA) 概要 MPIPC が R の Staphylococcus aureus ( または CFX がディスク拡散法で R ) または選択培地で MRSA と確認された菌微量液体希釈法の基準
Ver.3.1 Ver.3.2 改訂内容 (2019 年 1 月 ) 改訂対象改訂前改訂後 メチシリン耐性黄色ブドウ球菌 (MRSA) ペニシリン耐性肺炎球菌 (PRSP) 多剤耐性緑膿菌 (MDRP) 多剤耐性アシネトバクター属 (MDRA) 概要 MPIPC が R の Staphylococcus aureus ( または CFX がディスク拡散法で R ) または選択培地で MRSA と確認された菌微量液体希釈法の基準
DIC vegetation 1 nonbacterial thrombogenic e
 2001 2002 Guidelines for the Prevention and Treatment of Infective Endocarditis (JCS 2003) h 1 1 2 3 4 5 6 7 8 9 2 1 2 3 1 2 3 4 1 2 5 1 2 1 G Streptococcus viridans Streptococcus bovis 2 G Streptococcus
2001 2002 Guidelines for the Prevention and Treatment of Infective Endocarditis (JCS 2003) h 1 1 2 3 4 5 6 7 8 9 2 1 2 3 1 2 3 4 1 2 5 1 2 1 G Streptococcus viridans Streptococcus bovis 2 G Streptococcus
208 ( 2 ) THE JAPANESE JOURNAL OF ANTIBIOTICS 63 _ 3 June 2010 Cefditoren pivoxil (CDTR-PI) MS MS 10%
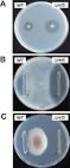 207 ( 1 ) Cefditoren pivoxil G 2010 2 2 2006 3 Cefditoren pivoxil CDTR-PI MS 10% CDTR-PI 305 2,144 2,006 1,958 1.79% 36 2,006 26 (1.30%) CDTR-PI CDTR-PI (9 mg/kg/day) 1.5 2 (2.70%) 2 (1.92%) 93.5% 1,831
207 ( 1 ) Cefditoren pivoxil G 2010 2 2 2006 3 Cefditoren pivoxil CDTR-PI MS 10% CDTR-PI 305 2,144 2,006 1,958 1.79% 36 2,006 26 (1.30%) CDTR-PI CDTR-PI (9 mg/kg/day) 1.5 2 (2.70%) 2 (1.92%) 93.5% 1,831
THE JAPANESE JOURNAL OF ANTIBIOTICS 67 3 June 2014 STFX mg mg mg mg mg 1
 June 2014 THE JAPANESE JOURNAL OF ANTIBIOTICS 67 3 175 29 1 2 2 2 2 2 3 4 4 5 5 2 2 1 2 3 4 5 2014 4 15 STFX 50 mg 10% 2011 8 1 100 mg 1 1 2011 12 2013 5 226 1,186 1,089 1,069 2.11% 23/1,089 1.10% 12/1,089
June 2014 THE JAPANESE JOURNAL OF ANTIBIOTICS 67 3 175 29 1 2 2 2 2 2 3 4 4 5 5 2 2 1 2 3 4 5 2014 4 15 STFX 50 mg 10% 2011 8 1 100 mg 1 1 2011 12 2013 5 226 1,186 1,089 1,069 2.11% 23/1,089 1.10% 12/1,089
CHEMOTHERAPY JUNE 1986
 VOL. 34 S-3 CHEMOTHERAPY Fig. 1 Structural formula of L-105 CHEMOTHERAPY JUNE 1986 VOL. 34 S-3 CHEMOTHERAPY Table 1 Antibacterial spectra of L-105 against gram negative anaerobic rods Inoculum 106 cells/ml
VOL. 34 S-3 CHEMOTHERAPY Fig. 1 Structural formula of L-105 CHEMOTHERAPY JUNE 1986 VOL. 34 S-3 CHEMOTHERAPY Table 1 Antibacterial spectra of L-105 against gram negative anaerobic rods Inoculum 106 cells/ml
Key Words: Klebsiella pneumoniae, CEP-AIS, MIC, "MBC", MIC of drugs in combination
 Key Words: Klebsiella pneumoniae, CEP-AIS, MIC, "MBC", MIC of drugs in combination Fig. 1. The following three kinds of overnight broth cultures of 10 strains of Kl. pneumoniae were inoculated on the agar
Key Words: Klebsiella pneumoniae, CEP-AIS, MIC, "MBC", MIC of drugs in combination Fig. 1. The following three kinds of overnight broth cultures of 10 strains of Kl. pneumoniae were inoculated on the agar
VOL.30 S-1 CHEMOTHERAPY Table 1 Antibacterial activity of CTT against standard strains Table 2 Antibacterial activity of CTT against standard strains
 CHEMOTHERAPY APR. 1982 Fig. 1 Chemical structure of cefotetan (CTT, YM09330) VOL.30 S-1 CHEMOTHERAPY Table 1 Antibacterial activity of CTT against standard strains Table 2 Antibacterial activity of CTT
CHEMOTHERAPY APR. 1982 Fig. 1 Chemical structure of cefotetan (CTT, YM09330) VOL.30 S-1 CHEMOTHERAPY Table 1 Antibacterial activity of CTT against standard strains Table 2 Antibacterial activity of CTT
